Mechanism of Action - Purine Synthesis Sabotage
-
Core Principle: Both drugs disrupt the de novo purine synthesis pathway, which is essential for the proliferation of T and B lymphocytes, as they lack robust salvage pathways.
-
**Azathioprine (AZA):
- Prodrug converted to 6-mercaptopurine (6-MP).
- 6-MP is then converted into fraudulent nucleotides that inhibit multiple steps in purine synthesis.
-
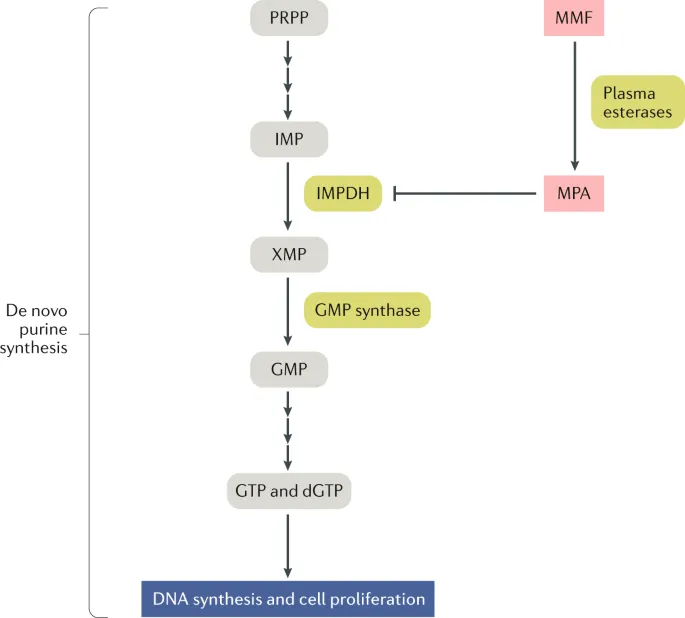
**Mycophenolate Mofetil (MMF):
- Prodrug hydrolyzed to mycophenolic acid (MPA).
- MPA is a potent, reversible inhibitor of Inosine Monophosphate Dehydrogenase (IMPDH), a rate-limiting step in de novo guanosine synthesis.
⭐ Both drugs ultimately disrupt the de novo purine synthesis pathway, starving proliferating lymphocytes of necessary DNA building blocks.
Pharmacokinetics - A Tale of Two Metabolites
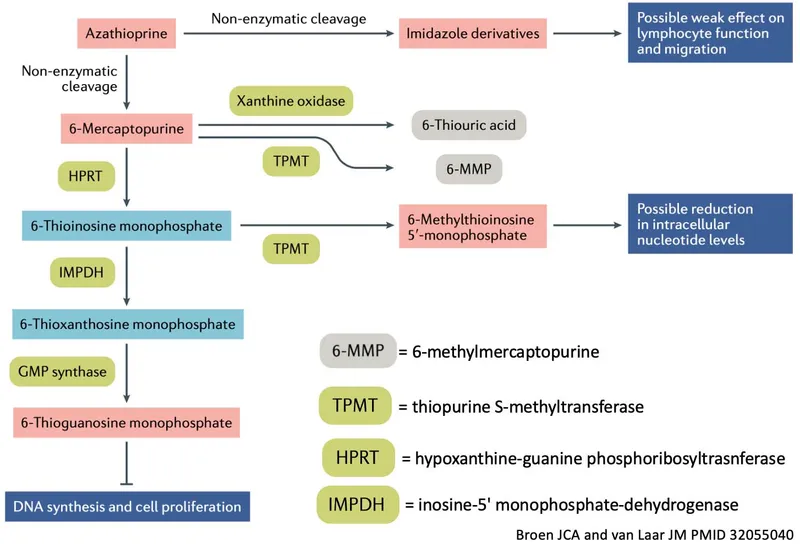
- Azathioprine (AZA): A prodrug, non-enzymatically cleaved to 6-mercaptopurine (6-MP).
- Activation: 6-MP is converted by HGPRT to active thioguanine nucleotides (TGNs), which disrupt DNA/RNA synthesis.
- Inactivation: Metabolized by two key enzymes:
- Thiopurine S-methyltransferase (TPMT)
- Xanthine Oxidase (XO)
- ⚠️ TPMT Deficiency: Genetic polymorphism can lead to ↓TPMT activity, causing ↑TGNs and severe, life-threatening myelosuppression. Screening is crucial.
⭐ Allopurinol, a xanthine oxidase inhibitor, dangerously increases azathioprine/6-MP levels, requiring a significant dose reduction (by ~75%).
- Mycophenolate Mofetil (MMF): A prodrug, rapidly hydrolyzed to the active metabolite, mycophenolic acid (MPA).
- Mechanism: MPA is a selective, non-competitive, reversible inhibitor of inosine monophosphate dehydrogenase (IMPDH).
- Selectivity: IMPDH is vital for the de novo purine synthesis pathway, which lymphocytes exclusively rely on. This provides lymphocyte-specific cytotoxicity.
Clinical Use & Toxicities - Prescribing Points
Azathioprine (AZA)
- Clinical Use:
- Autoimmune conditions (e.g., Rheumatoid Arthritis, IBD).
- Prophylaxis of organ transplant rejection.
- Toxicities & Prescribing Points:
- Myelosuppression: Pancytopenia, especially in patients with low Thiopurine Methyltransferase (TPMT) activity.
- ⚠️ Screen for TPMT deficiency before initiating therapy.
- GI Effects: Nausea, vomiting.
- Hepatotoxicity: Monitor LFTs.
- Drug Interaction: Allopurinol ↑ AZA toxicity by inhibiting xanthine oxidase. Must reduce AZA dose by ~75%.
- Myelosuppression: Pancytopenia, especially in patients with low Thiopurine Methyltransferase (TPMT) activity.
Mycophenolate Mofetil (MMF)
- Clinical Use:
- Prophylaxis of solid organ transplant rejection (kidney, heart, liver).
- Lupus nephritis.
- Toxicities & Prescribing Points:
- GI Effects: Diarrhea and vomiting are very common.
- Myelosuppression: Primarily leukopenia. Monitor CBC.
- Infections: Increased risk of opportunistic infections (e.g., CMV).
- Teratogenicity:
⭐ Mycophenolate is highly teratogenic, requiring a negative pregnancy test before initiation and reliable contraception during treatment (REMS program).
High‑Yield Points - ⚡ Biggest Takeaways
- Azathioprine, a prodrug of 6-mercaptopurine (6-MP), blocks de novo purine synthesis. Its toxicity is markedly increased by allopurinol.
- Mycophenolate mofetil is a reversible inhibitor of inosine monophosphate dehydrogenase (IMPDH), selectively blocking lymphocyte purine synthesis.
- The major dose-limiting toxicity for both is bone marrow suppression (pancytopenia).
- Mycophenolate is strongly associated with GI distress (diarrhea) and is highly teratogenic.
- Monitor for opportunistic infections, especially CMV with mycophenolate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

