Corticosteroids - Cellular Commandos
- Mechanism: Act as synthetic analogs of natural cortisol, binding to intracellular glucocorticoid receptors (GR).
- Genomic Effects: The steroid-receptor complex translocates to the nucleus, where it modulates gene expression by:
- Transactivation: Upregulating anti-inflammatory genes (e.g., annexin A1).
- Transrepression: Downregulating pro-inflammatory genes (e.g., cytokines via NF-κB inhibition).
⭐ Corticosteroids inhibit phospholipase A2 (PLA2) by inducing annexin-1 (lipocortin), which blocks the release of arachidonic acid, the precursor to prostaglandins and leukotrienes.
Effects & Uses - The Good & The Bad
The Good (Therapeutic Uses):
- Anti-inflammatory & Immunosuppressive:
- Autoimmune diseases (RA, SLE), IBD, asthma, allergies.
- Prevents organ transplant rejection.
- Replacement Therapy: For adrenal insufficiency (Addison's disease).
- Fetal Lung Development: Betamethasone/Dexamethasone given to mothers in preterm labor (< 34 weeks) to mature fetal lungs.
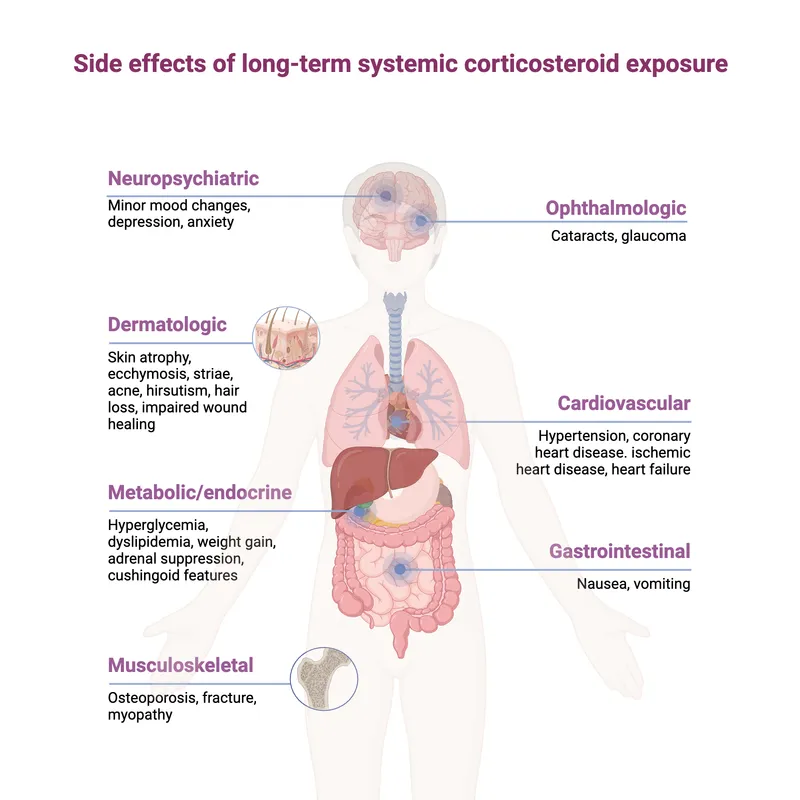
The Bad (Adverse Effects): 📌 CUSHINGOID
- Cataracts & Cushing's Syndrome
- Ulcers (Peptic)
- Skin thinning, Striae
- Hypertension, Hyperglycemia
- Immunosuppression
- Necrosis (Avascular, esp. femoral head)
- Growth retardation (in children)
- Osteoporosis
- Impaired wound healing
- Depression/Psychosis
⭐ Abrupt cessation after prolonged use risks acute adrenal crisis (hypotension, shock). Always taper slowly!
Adverse Effects - The Price of Power
Long-term use is a double-edged sword, leading to iatrogenic Cushing's syndrome.
- Metabolic & Endocrine:
- Hyperglycemia, weight gain
- Iatrogenic Cushing's Syndrome (moon facies, buffalo hump)
- Adrenal suppression (requires tapering)
- Hypogonadism, amenorrhea
- Musculoskeletal:
- Osteoporosis (vertebral compression fractures)
- Myopathy (proximal muscle weakness)
- GI & Renal:
- Peptic ulcers, GI bleeding
- Fluid retention (hypertension), hypokalemia
- CNS & Psychiatric:
- Psychosis, insomnia, anxiety ("steroid rage")
- Immune:
- Immunosuppression (↑ infection risk)
- Reactivation of latent TB
- Dermatologic & Ocular:
- Skin thinning, striae, easy bruising
- Cataracts, glaucoma
⭐ Avascular necrosis of the femoral head is a classic, devastating complication of chronic steroid use, often presenting as hip pain.
Clinical Pearls - Tapering & Tactics
- Goal: Prevent iatrogenic Hypothalamic-Pituitary-Adrenal (HPA) axis suppression, which can lead to adrenal insufficiency.
- Rule of Thumb: Tapering is generally required if treatment exceeds 3 weeks.
- Method: Reduce dose slowly, allowing the HPA axis to recover function. The final steps of the taper are the slowest.
- 💡 Patients on long-term steroids require "stress-dose" steroids during acute illness or surgery to prevent adrenal crisis, even if recently tapered.
⭐ Abrupt cessation after prolonged use can precipitate an Addisonian crisis (hypotension, shock, hypoglycemia).
High‑Yield Points - ⚡ Biggest Takeaways
- Corticosteroids bind intracellular receptors, translocating to the nucleus to modify gene transcription.
- Key anti-inflammatory effect: inhibit Phospholipase A2 via Lipocortin-1 synthesis, blocking prostaglandins and leukotrienes.
- Suppress immunity by inhibiting NF-κB, decreasing pro-inflammatory cytokines like IL-2 and TNF-alpha.
- Cause neutrophilia by demargination, but lymphopenia and eosinopenia.
- Chronic use leads to iatrogenic Cushing's syndrome and osteoporosis.
- Abrupt withdrawal after prolonged use risks acute adrenal insufficiency; always taper the dose.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

