Pathophysiology - The Long & Winding QT
- QT Interval: Represents the duration of the ventricular myocyte action potential (AP), from initial depolarization to complete repolarization.
- Core Defect: Prolongation of AP Phase 3 (ventricular repolarization).
- Primarily due to blockade of the delayed rectifier potassium current ($I_{Kr}$).
- This ↓ K⁺ efflux lengthens repolarization time, stretching the QT interval.
- Trigger for TdP: This prolonged plateau can lead to early afterdepolarizations (EADs), which can initiate polymorphic ventricular tachycardia if they reach threshold.
⭐ Congenital Long QT Syndromes often result from mutations in genes encoding cardiac potassium (e.g., KCNH2) or sodium channels, impairing repolarization.
Etiologies - The Usual Suspects
-
QTc Interval Thresholds: Prolonged if > 450 ms (males) or > 470 ms (females). High risk for TdP if > 500 ms.
-
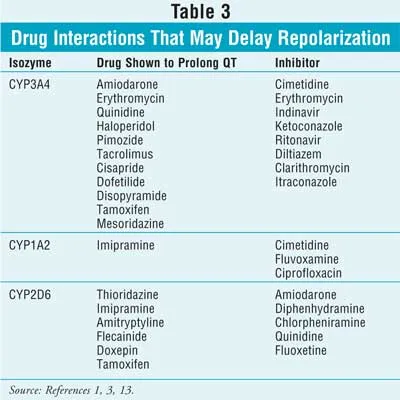
Medications (Most Common Cause)
- 📌 Mnemonic: ABCDE
- Antiarrhythmics: Class IA (Quinidine, Procainamide), Class III (Amiodarone, Sotalol, Dofetilide)
- Biotics (Antibiotics): Macrolides (Erythromycin, Azithromycin), Fluoroquinolones
- Cychotics (Antipsychotics): Haloperidol, Ziprasidone, other atypical antipsychotics
- Depressants (Antidepressants): TCAs (Amitriptyline), SSRIs (Citalopram)
- Emetics (Antiemetics): Ondansetron (5-HT3 antagonists)
- Others: Azole antifungals (e.g., Fluconazole)
-
Electrolyte Disturbances
- ↓ K⁺ (Hypokalemia)
- ↓ Mg²⁺ (Hypomagnesemia)
- ↓ Ca²⁺ (Hypocalcemia)
-
Other Causes
- Congenital Long QT Syndrome (e.g., Romano-Ward, Jervell and Lange-Nielsen)
- Bradycardia, Hypothyroidism
⭐ Exam Favorite: Citalopram carries a dose-dependent risk of QT prolongation. The FDA recommends a maximum dose of 40 mg/day (20 mg/day in patients >60 years, or with hepatic impairment).
Diagnosis - ECG Tells the Tale
- ECG is key: Look for a prolonged QT interval, corrected for heart rate (QTc).
- Bazett's Formula: $QTc = QT / \sqrt{RR}$
- Thresholds: QTc > 450 ms in males, > 470 ms in females.
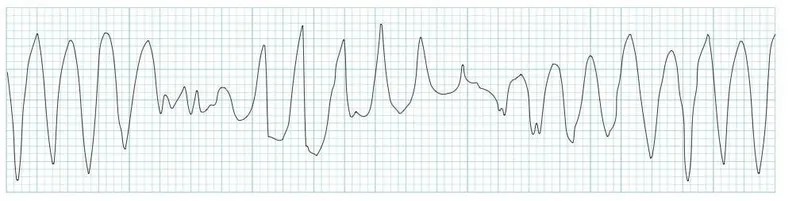
- Torsades de Pointes (TdP): A specific polymorphic ventricular tachycardia.
- ECG shows rapid, irregular, QRS complexes twisting around the isoelectric baseline.
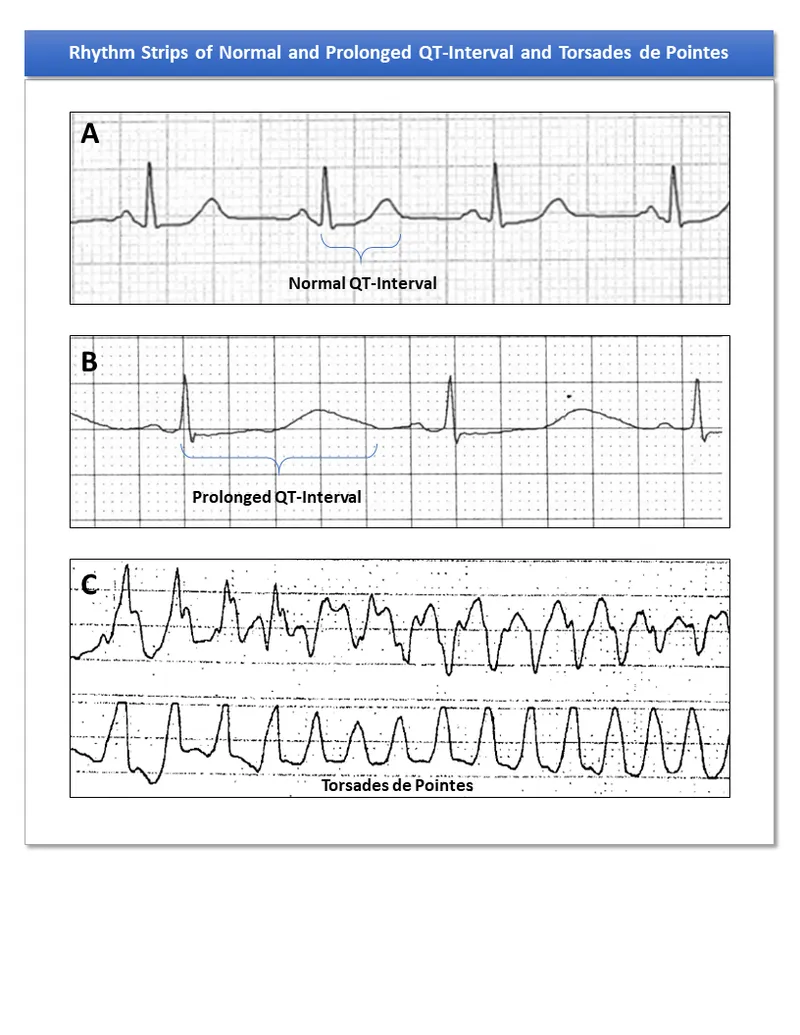
⭐ Exam Favorite: TdP is often initiated by a "short-long-short" R-R interval sequence, where a PVC follows a long pause.
Management - Taming the Twisting Storm
- Immediate Actions: Discontinue all QT-prolonging agents. Correct electrolyte imbalances, especially hypokalemia and hypomagnesemia.
⭐ IV magnesium is the first-line therapy for TdP regardless of the patient's baseline magnesium level; it stabilizes the cardiac membrane.
High‑Yield Points - ⚡ Biggest Takeaways
- QT prolongation is a major risk factor for Torsades de Pointes (TdP), a life-threatening polymorphic ventricular tachycardia.
- Key drug classes include Class IA/III antiarrhythmics, macrolides, fluoroquinolones, antipsychotics, and -azole antifungals.
- Hypokalemia and hypomagnesemia are critical co-factors that significantly increase TdP risk.
- The first-line treatment for TdP is immediate IV magnesium sulfate, which stabilizes the cardiac membrane.
- Always discontinue the offending drug and correct underlying electrolyte imbalances.
- ECG shows characteristic twisting QRS complexes around the isoelectric line.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

