Nicotinic Antagonists - The Two Blockades
- Two major sites of action: Autonomic ganglia & Neuromuscular Junction (NMJ).
- Ganglionic Blockers: (e.g., Hexamethonium, Mecamylamine) Block autonomic ganglia, causing broad, complex effects. Rarely used clinically due to non-specificity.
- Neuromuscular Blockers (NMBs): Target nicotinic receptors at the NMJ for skeletal muscle paralysis, primarily in anesthesia.
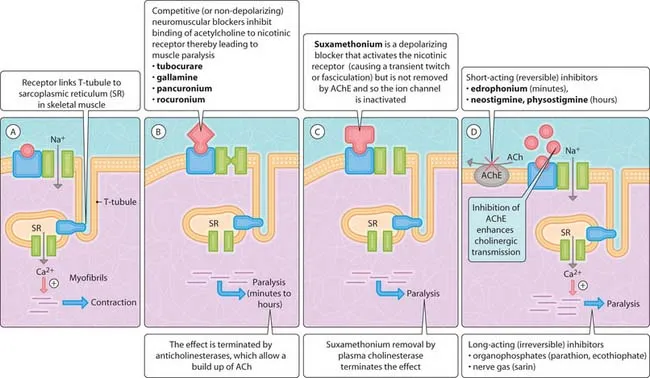
- Non-Depolarizing (Competitive) Blockade:
- Compete with ACh for NMJ receptors.
- Reversal: ↑ ACh levels with cholinesterase inhibitors (e.g., Neostigmine).
- Depolarizing Blockade:
- Succinylcholine: Binds to and activates the nicotinic receptor, causing persistent depolarization.
- Phase I: Initial fasciculations, then flaccid paralysis. Potentiated by cholinesterase inhibitors.
- Phase II: Receptor desensitization. Resembles non-depolarizing block; may be reversed by cholinesterase inhibitors.
⭐ Succinylcholine can cause life-threatening hyperkalemia in patients with burns, crush injuries, or extensive denervation. Avoid use in these settings.
Non-Depolarizing Blockers - Competitive Crew
- Mechanism: Competitive antagonists at the neuromuscular junction (NMJ) nicotinic receptors ($N_M$). They prevent acetylcholine (ACh) from binding, leading to flaccid paralysis.
- Drugs: "-curonium" or "-curium" endings. (e.g., Pancuronium, Rocuronium, Vecuronium, Atracurium, Cisatracurium).
- Clinical Use: Adjuvant in anesthesia for skeletal muscle relaxation.
- Reversal: Overcome blockade by increasing ACh. Use acetylcholinesterase inhibitors (e.g., Neostigmine, Edrophonium). Always co-administer with an antimuscarinic (e.g., Atropine, Glycopyrrolate) to prevent systemic muscarinic effects (bradycardia, salivation).
- Key Side Effects:
- Atracurium/Tubocurarine: Can trigger histamine release → hypotension, flushing, bronchoconstriction.
- Pancuronium: Moderate muscarinic receptor blockade → tachycardia.
⭐ Atracurium and its isomer Cisatracurium are inactivated spontaneously in plasma (Hofmann elimination), making them ideal for patients with hepatic or renal failure.
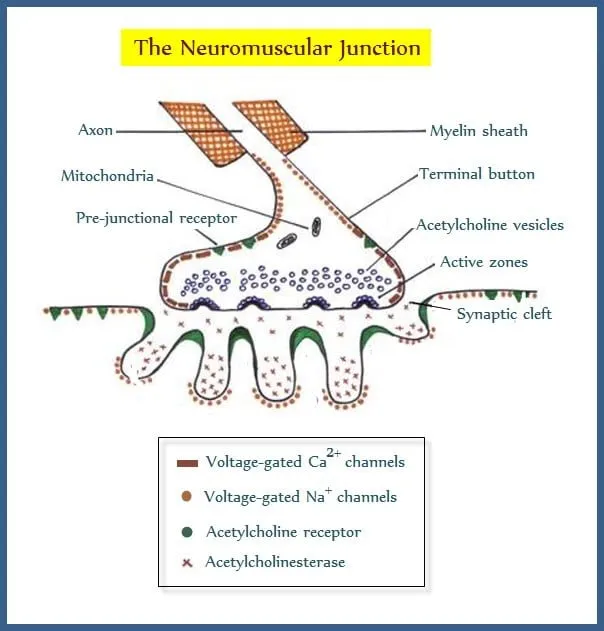
Depolarizing Blockers - Succinylcholine's Twist
- Mechanism: Binds to postsynaptic nicotinic acetylcholine receptors (nAChR) at the neuromuscular junction (NMJ), mimicking acetylcholine (ACh).
- Structure: Essentially two ACh molecules linked end-to-end.
- Metabolism: Rapidly hydrolyzed by plasma butyrylcholinesterase (pseudocholinesterase), not acetylcholinesterase (AChE).
Two-Phase Blockade
Clinical Pearls
- Use: Rapid-sequence intubation due to fast onset (~1 min) and short duration (~10 min).
- Adverse Effects:
- ⚠️ Hyperkalemia: Risk in patients with burns, crush injuries, or neuromuscular disease due to upregulation of nAChRs.
- Malignant Hyperthermia: Especially with halogenated anesthetics. Treat with dantrolene.
- Increased intraocular and intragastric pressure.
⭐ Exam Favorite: Succinylcholine can cause life-threatening hyperkalemia in patients with extensive tissue damage (burns, trauma) or denervation (Guillain-Barré, ALS), leading to cardiac arrest. Avoid in these settings.
High‑Yield Points - ⚡ Biggest Takeaways
- Ganglionic blockers (e.g., hexamethonium) act on both autonomic ganglia; effects depend on the dominant tone of the target organ.
- Neuromuscular blockers are either depolarizing (succinylcholine) or non-depolarizing (e.g., rocuronium, vecuronium).
- Succinylcholine causes initial muscle fasciculations (Phase I block), followed by flaccid paralysis (Phase II block).
- Non-depolarizing agents are competitive antagonists at the NMJ; their blockade is reversed by AChE inhibitors.
- Beware of malignant hyperthermia with succinylcholine and histamine release with atracurium.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

