Mechanism of Action - Closing the Calcium Gates
- Primary Target: Block voltage-gated L-type calcium channels ($Ca_V 1.2$), primarily in cardiac tissue.
- Key Sites of Action: Greatest effect on the sinoatrial (SA) and atrioventricular (AV) nodes, which are calcium-dependent.
- Electrophysiological Effects:
- Decreases the inward calcium current ($I_{Ca}$) that drives the late Phase 0 depolarization in nodal cells.
- Slows the rate of rise of the SA node pacemaker potential → ↓ heart rate (negative chronotropy).
- Slows conduction velocity and increases the effective refractory period (ERP) in the AV node.
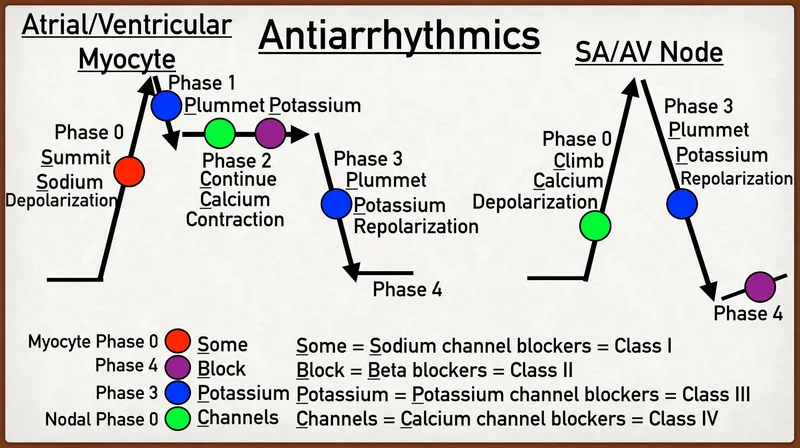
⭐ By slowing AV conduction, Class IV drugs characteristically prolong the PR interval on an ECG. This is their primary antiarrhythmic mechanism for controlling ventricular rate in atrial fibrillation.
Types & Pharmacokinetics - Dihydros vs. Non-dihydros
-
Dihydropyridines (DHPs): Amlodipine, Nifedipine ("-dipine" suffix)
- Vascular-selective: Potent arteriolar vasodilation with minimal effect on cardiac contractility or AV node conduction at therapeutic doses.
- Used for hypertension and angina.
- 📌 Mnemonic: "Di-hydro-Pines" primarily "Di-late" peripheral vessels.
-
Non-dihydropyridines (Non-DHPs): Verapamil, Diltiazem
- Cardio-selective: Act on both the heart and vascular smooth muscle, decreasing cardiac workload.
- Verapamil: Most cardioselective; significant negative inotropic and chronotropic effects. Think Verapamil for Ventricular rate control.
- Diltiazem: Intermediate action on both heart and vessels.
- Used for rate control (atrial fibrillation/flutter) and angina.
⭐ Dihydropyridines can trigger reflex tachycardia due to profound vasodilation and baroreceptor activation. This is counteracted by Non-DHPs, which directly suppress heart rate.
Clinical Applications - The Heart Rescuers
- Supraventricular Tachycardias (SVT): Excellent for terminating re-entrant tachycardias that depend on the AV node for the circuit.
- Atrial Fibrillation & Flutter: A cornerstone of therapy for rate control by directly slowing AV nodal conduction.
- Angina Pectoris (Stable & Vasospastic): Decrease myocardial oxygen demand by reducing heart rate, contractility, and afterload.
- Hypertension: Effective, particularly in patients with comorbid angina or arrhythmias.
- Migraine Prophylaxis: Verapamil is used for prevention.
⭐ In hypertrophic cardiomyopathy (HCM), non-dihydropyridine CCBs are used to improve diastolic relaxation and reduce symptoms related to dynamic outflow tract obstruction.
Adverse Effects & Contraindications - Handle With Care
- Cardiovascular System:
- Bradycardia, high-degree AV block, and worsening heart failure (especially non-dihydropyridines like Verapamil).
- Peripheral edema, flushing, headache, and dizziness (more common with dihydropyridines).
- Symptomatic hypotension.
- Other Key Effects:
- Constipation is a classic side effect of Verapamil. 📌 Verapamil = Very constipating.
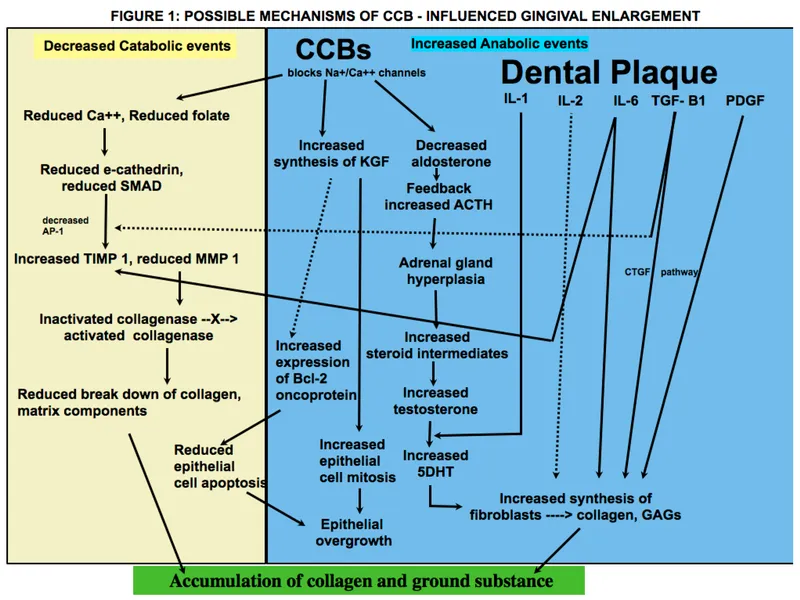
- Gingival hyperplasia can occur with prolonged use.
- Contraindications & Cautions:
- ⚠️ Sick Sinus Syndrome or 2nd/3rd degree AV block without a functioning pacemaker.
- Severe hypotension (Systolic BP < 90 mmHg).
- Decompensated heart failure.
- ⚠️ Avoid concurrent IV non-DHPs with IV β-blockers.
⭐ In Wolff-Parkinson-White (WPW) syndrome, giving a CCB during atrial fibrillation blocks the normal AV node pathway. This forces impulses down the faster accessory pathway, potentially triggering ventricular fibrillation.
High‑Yield Points - ⚡ Biggest Takeaways
- Verapamil and diltiazem primarily block L-type Ca²⁺ channels in cardiac tissue.
- Their main effect is to slow conduction through the AV node, reducing heart rate.
- Clinically used for rate control in atrial fibrillation and other supraventricular tachycardias.
- Key side effects include constipation (especially verapamil), gingival hyperplasia, and bradycardia.
- Avoid use in systolic heart failure and in patients with 2nd or 3rd-degree AV block.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

