Diuretic Classes - The Nephron Hit List
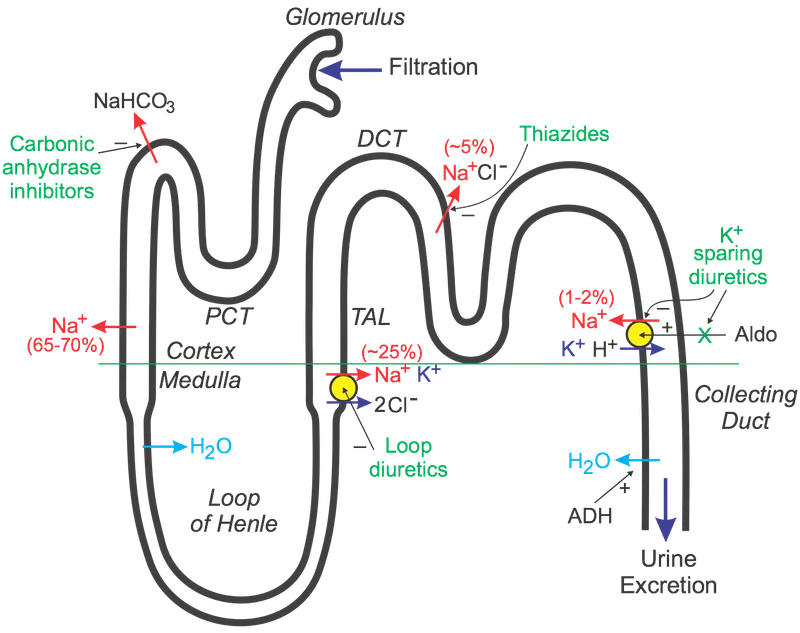
- Proximal Convoluted Tubule (PCT): Carbonic Anhydrase Inhibitors (e.g., Acetazolamide)
- Thick Ascending Limb (TAL): Loop Diuretics (e.g., Furosemide)
- Inhibit Na-K-2Cl cotransporter.
- Distal Convoluted Tubule (DCT): Thiazide Diuretics (e.g., Hydrochlorothiazide)
- Inhibit Na-Cl cotransporter.
- Collecting Duct: K-Sparing Diuretics (e.g., Spironolactone, Amiloride)
⭐ Thiazides can cause hypercalcemia as they increase distal tubular reabsorption of Ca²⁺, making them useful for osteoporosis.
📌 Mnemonic (proximal to distal): Punch The Ticket, Chief!
Loop Diuretics - The Powerhouse Blockers
- MOA: Inhibit the Na⁺/K⁺/2Cl⁻ cotransporter in the thick ascending limb of the Loop of Henle.
- Drugs: Furosemide, Bumetanide, Torsemide. Ethacrynic acid (for sulfa allergy).
- Key Effects:
- Most potent diuretic class; causes significant ↑ in Na⁺, K⁺, Cl⁻ excretion.
- "Loops Lose Ca²⁺" → increases Ca²⁺ excretion.
- Uses: Edema (HF, cirrhosis), HTN with renal failure, hypercalcemia.
- Adverse Effects: Hypokalemia, ototoxicity, hyperuricemia (gout).
- 📌 OHH DAANG! (Ototoxicity, Hypokalemia, Hypomagnesemia, Dehydration, Allergy, Nephritis, Gout).
⭐ Exam Favorite: Loops stimulate prostaglandin release, causing afferent arteriole vasodilation. NSAIDs can blunt their diuretic effect by inhibiting prostaglandins.
Thiazide Diuretics - The Gentle Squeezers
- Mechanism: Inhibit the Na⁺-Cl⁻ cotransporter (NCC) in the Distal Convoluted Tubule (DCT).
- Primary Effect: Modest increase in Na⁺, Cl⁻, and water excretion.
- Electrolyte Changes:
- ↓ Serum: Na⁺, K⁺, Mg²⁺
- ↑ Serum: Ca²⁺ (spares calcium), Uric acid, Glucose, Lipids
- Clinical Uses:
- Hypertension (first-line therapy)
- Edema (mild heart failure)
- Nephrolithiasis (from idiopathic hypercalciuria)
- Nephrogenic diabetes insipidus
- Adverse Effects: Hypokalemic metabolic alkalosis, hyponatremia, sulfa allergy.
- 📌 Remember the "Hyper-GLUC" side effects: HyperGlycemia, HyperLipidemia, HyperUricemia, and HyperCalcemia.
⭐ Thiazides lose efficacy when GFR is < 30 mL/min (exception: metolazone).
K-Sparing Diuretics - The Potassium Keepers
- Mechanism: Act on collecting ducts to ↓Na+ reabsorption & ↓K+ secretion.
- Aldosterone Antagonists: Spironolactone, Eplerenone.
- ENaC Blockers: Amiloride, Triamterene.
- Primary Use: Often co-administered with thiazide or loop diuretics to mitigate hypokalemia. Also used in heart failure and hyperaldosteronism.
- Adverse Effects: ⚠️ Hyperkalemia (risk ↑ with ACEi/ARBs), metabolic acidosis.
- 📌 Mnemonic: The K+ STAys with Spironolactone, Triamterene, Amiloride.
⭐ Spironolactone's anti-androgen activity can lead to painful gynecomastia, a frequently tested side effect.
Other Diuretics - Niche Agents
-
Carbonic Anhydrase Inhibitors (Acetazolamide)
- Site: Proximal Convoluted Tubule (PCT).
- Mechanism: Inhibits carbonic anhydrase → ↓ NaHCO₃ reabsorption → self-limited bicarbonate diuresis.
- Uses: Glaucoma, metabolic alkalosis, altitude sickness.
- Adverse Effect: Hyperchloremic metabolic acidosis. 📌 "ACID"-azolamide.
-
Osmotic Diuretics (Mannitol)
- Site: PCT, thin descending limb.
- Mechanism: ↑ tubular fluid osmolarity, drawing water into the lumen.
- Uses: ↓ intracranial and intraocular pressure.
⭐ Mannitol may cause pulmonary edema by rapidly expanding extracellular fluid volume before the onset of diuresis.
High‑Yield Points - ⚡ Biggest Takeaways
- Thiazides block the Na-Cl cotransporter in the DCT, causing hypercalcemia.
- Loop diuretics inhibit the Na-K-2Cl cotransporter in the thick ascending limb and are most potent; they cause hypocalcemia.
- K+-sparing diuretics (e.g., Spironolactone) are aldosterone antagonists in the collecting duct, risking hyperkalemia.
- Most diuretics cause hypokalemia, except for K+-sparing types.
- Acetazolamide inhibits carbonic anhydrase in the PCT; used for glaucoma and metabolic alkalosis.
- Mannitol is an osmotic diuretic used to decrease intracranial pressure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

