Mechanism of Action - Potent Protein Killers
- Class Members: Gentamicin, Tobramycin, Amikacin, Streptomycin, Neomycin.
- Action: Irreversibly bind to the 30S ribosomal subunit.
- Blocks the initiation of protein synthesis.
- Causes misreading of the mRNA template, leading to nonfunctional proteins.
- Results in a potent, bactericidal effect.
- 📌 Mnemonic: "buy AT 30, CCEL at 50" (Aminoglycosides & Tetracyclines at 30S; Clindamycin, Chloramphenicol, Erythromycin, Linezolid at 50S).
⭐ Aminoglycosides exhibit concentration-dependent killing and a significant post-antibiotic effect (PAE), allowing for effective once-daily dosing regimens.
Spectrum & Uses - The Gram-Negative Busters
Potent bactericidal activity primarily against aerobic Gram-negative rods. They require $O_2$ for uptake, making them ineffective against anaerobes.
- Primary Targets: Pseudomonas aeruginosa, Klebsiella spp., E. coli.
- Synergistic Use: Combined with cell wall inhibitors (β-lactams, vancomycin) to broaden coverage or for a synergistic kill.
- Gram-Positive: Treats serious infections like Enterococcal or Staphylococcal endocarditis.
- Gram-Negative: Empiric therapy for sepsis.
⭐ Aminoglycosides are ineffective against anaerobes because their transport into the bacterial cell is an oxygen-dependent process.
Adverse Effects - Kidneys & Ears Beware
📌 Mnemonic: "Ami-NO" for Nephrotoxicity & Ototoxicity.
- Nephrotoxicity:
- Causes acute tubular necrosis (ATN), leading to ↑ serum creatinine.
- Damage is concentration-dependent and usually reversible upon discontinuation.
- Ototoxicity:
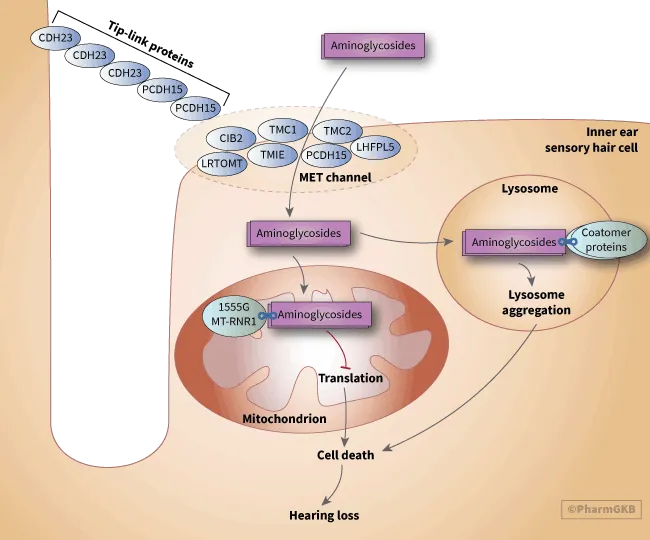
- Causes irreversible damage to inner ear hair cells.
- Auditory (cochlear) damage → tinnitus & hearing loss.
- Vestibular damage → vertigo, ataxia.
- Neuromuscular Blockade:
- Can induce muscle paralysis by inhibiting presynaptic acetylcholine release.
- ⚠️ High risk in patients with Myasthenia Gravis or those receiving neuromuscular blockers.
- Therapeutic Drug Monitoring (TDM):
- Monitor trough levels to prevent accumulation and dose-dependent toxicities.
⭐ Loop diuretics (e.g., furosemide) greatly potentiate the risk of aminoglycoside-induced ototoxicity.
Resistance Mechanisms - The Bacterial Defense
- Enzymatic Modification (Most Common): Bacterial transferase enzymes, often plasmid-mediated, inactivate the drug via:
- Acetylation
- Phosphorylation
- Adenylation
- Impaired Entry: Reduced drug uptake due to porin channel mutations or altered transport systems.
- Altered Target: Mutations in the 30S ribosomal subunit binding site decrease drug affinity.
⭐ Amikacin is often effective against gentamicin and tobramycin-resistant strains as it is a poor substrate for many inactivating enzymes.
High‑Yield Points - ⚡ Biggest Takeaways
- Aminoglycosides are bactericidal inhibitors of the 30S ribosomal subunit, targeting serious aerobic gram-negative infections.
- Exhibit concentration-dependent killing and a significant post-antibiotic effect (PAE), allowing for once-daily dosing.
- Major dose-limiting toxicities are nephrotoxicity (reversible ATN) and irreversible ototoxicity (cochlear and vestibular).
- Can cause neuromuscular blockade, a key contraindication in Myasthenia Gravis.
- Used synergistically with cell wall agents (β-lactams) for certain gram-positive infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

