General Principles - The Ground Rules
- Live vaccines: Generally contraindicated due to risk of vaccine-induced disease.
- Killed/Inactivated vaccines: Safe, but may have ↓ immunogenicity. May require higher doses or extra boosters.
- Optimal Timing:
- Administer necessary vaccines preferably ≥4 weeks before initiating immunosuppressive therapy.
- Postpone live vaccines for ≥3 months after chemotherapy; ≥6 months for anti-B cell antibodies (e.g., Rituximab).
- Household Contacts: Should be fully vaccinated (including MMR, Varicella) to provide a protective cocoon.
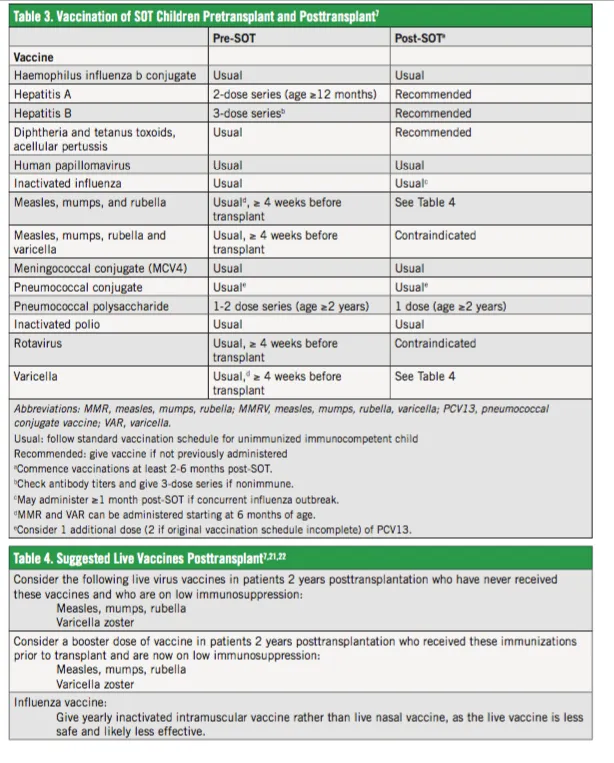
⭐ After solid organ transplantation, live vaccines are generally withheld. Inactivated vaccines can be given starting 3-6 months post-transplant, once immunosuppression is stable.
Primary Immunodeficiencies - Congenital Gaps
- Core Principle: Vaccination strategy hinges on the specific immune defect. The main danger lies with live attenuated vaccines causing iatrogenic disseminated disease.
- Key Contraindications:
- Severe T-cell defects (e.g., SCID, complete DiGeorge): ALL live vaccines (viral & bacterial) are absolutely contraindicated. Household contacts should also avoid OPV.
- Severe Humoral/B-cell defects (e.g., XLA): Live vaccines contraindicated. Inactivated vaccines are safe but may have poor efficacy; check antibody titres post-vaccination.
- Phagocytic defects (e.g., CGD): Live bacterial vaccines (BCG, oral typhoid) are contraindicated. Live viral vaccines (MMR, Varicella) are generally safe.
⭐ In Severe Combined Immunodeficiency (SCID), rotavirus vaccine can cause severe, persistent gastroenteritis, and BCG can lead to fatal disseminated BCG-osis.
Secondary Immunosuppression - Acquired Weaknesses
-
General Principle: Avoid live vaccines in severely immunocompromised states. Inactivated vaccines are safe but may have ↓ immunogenicity.
-
HIV Infection:
- Strategy depends on CD4 count. Live vaccines (MMR, Varicella) are permitted if CD4 count >200 cells/µL & CD4% >15%.
- BCG is absolutely contraindicated regardless of CD4 status.
- Inactivated vaccines are safe but may have a suboptimal response.
-
Malignancy / Chemotherapy:
- Live vaccines: Contraindicated during and for 3-6 months after chemotherapy. Administer ≥4 weeks before starting.
- Inactivated vaccines: Give ≥2 weeks before or 3 months after chemotherapy for optimal response.
-
Asplenia (Anatomic or Functional):
- High risk for encapsulated bacteria: S. pneumoniae, H. influenzae type b, N. meningitidis.
- Vaccinate ≥2 weeks before elective splenectomy or ≥2 weeks after.
- Mandatory vaccines: Pneumococcal (PCV, PPSV23), Meningococcal (conjugate, MenB), Hib.
⭐ For patients post-chemotherapy, the standard waiting period for administering live vaccines is at least 3 months. This ensures immune reconstitution and vaccine safety.
Household Contacts - Cocooning the Vulnerable
"Cocooning" protects the immunocompromised by vaccinating their close contacts.
- Live vaccines: Generally safe for contacts, with key exceptions.
- Avoid: Oral Polio Vaccine (OPV) due to shedding; use IPV instead.
- Recommended: MMR and Varicella vaccines are encouraged.
- Influenza: All household members should receive the annual injectable flu shot.
⭐ If a varicella-vaccinated contact develops a rash, they must avoid the patient until all lesions have crusted over.
High‑Yield Points - ⚡ Biggest Takeaways
- Live vaccines are generally contraindicated in immunocompromised hosts.
- Exceptions include MMR and VZV, which can be given to asymptomatic HIV-infected children with adequate CD4 counts.
- Inactivated vaccines are safe but may elicit a suboptimal immune response.
- Household contacts should receive routine vaccines for cocooning, but must avoid the oral polio vaccine (OPV).
- Administer live vaccines ≥4 weeks before immunosuppression; inactivated vaccines ≥2 weeks before.
- Annual influenza and pneumococcal vaccines are critical in this group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

