Initial Assessment - First Look, Act Fast
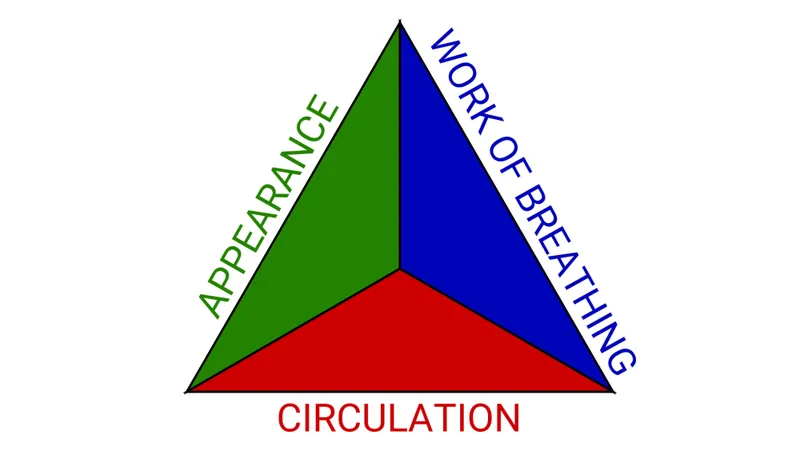
Rapidly assess using the Pediatric Assessment Triangle (PAT) to determine if the child is "sick" or "not sick" before touching them.
- Appearance (TICLS Mnemonic 📌):
- Tone, Interactiveness, Consolability, Look/Gaze, Speech/Cry.
- Most important limb for brain perfusion & CNS function.
- Work of Breathing:
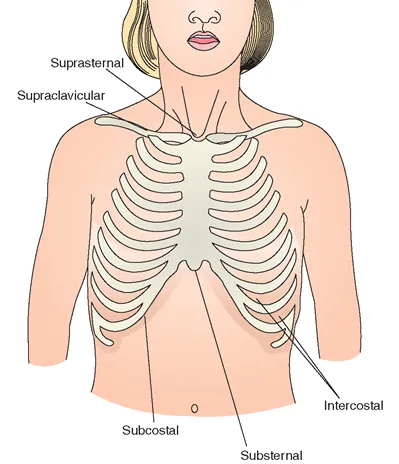
- Visual: Nasal flaring, retractions (subcostal, intercostal, suprasternal), head bobbing.
- Audible: Stridor, wheezing, grunting.
- Circulation to Skin:
- Assesses peripheral perfusion.
- Signs: Pallor, mottling, cyanosis.
⭐ Grunting is an ominous sign of impending respiratory failure. It is the body's attempt to create auto-PEEP (Positive End-Expiratory Pressure) to keep alveoli open.
Etiology & X-Rays - The Usual Suspects
-
Upper Airway Obstruction (Stridor)
-
Croup (Laryngotracheobronchitis): Viral (Parainfluenza). X-Ray (AP Neck) shows Steeple Sign (subglottic narrowing).
-
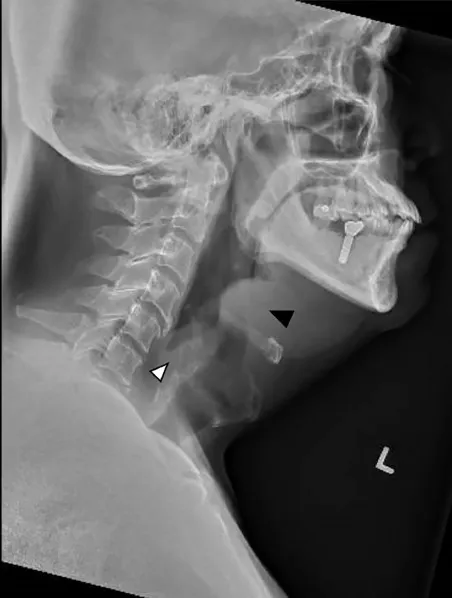
Acute Epiglottitis: Bacterial (H. influenzae, Strep.). X-Ray (Lateral Neck) shows Thumb Sign (swollen epiglottis).
-
-
Lower Airway Obstruction (Wheeze/Crackles)
- Bronchiolitis: RSV is the main cause in children < 2 years. X-Ray shows hyperinflation, atelectasis, and peribronchial thickening.
- Foreign Body Aspiration (FBA): Inspiratory films may be normal. Expiratory X-Ray is key, showing unilateral air trapping (hyperlucency).
- Pneumonia: X-Ray reveals lobar consolidation, interstitial infiltrates, or air bronchograms.
⭐ Exam Favourite: Croup's "Steeple sign" is best seen on an AP view of the neck, whereas the "Thumb sign" of epiglottitis requires a lateral view.
📌 Mnemonic: Think of a church steeple for Croup, and a thumb print for Epiglottitis.
Severity Scoring - Grading the Gasp
- Silverman-Andersen Score (SAS): Assesses respiratory work in neonates. Score 0 (normal) to 10 (severe).
- Downe's Score: Modified for older children; includes respiratory rate, air entry, and cyanosis.
- SAS Components & Scoring (0, 1, or 2):
- Upper Chest Movement (Sync vs. Lag vs. Seesaw)
- Lower Chest Retractions
- Xiphoid Retractions
- Nasal Flaring
- Expiratory Grunt
- Interpretation:
- Score <4: Mild distress
- Score 4-6: Moderate distress
- Score >7: Impending respiratory failure
⭐ Expiratory Grunting: A key sign of significant distress. It's the body's attempt to create auto-PEEP (Positive End-Expiratory Pressure) to keep alveoli from collapsing.
Management - The Rescue Plan
- Universal First Steps:
- Positioning: Position of comfort (e.g., tripod); avoid agitating the child.
- Oxygen: Titrate to maintain SpO₂ >94% via high-flow nasal cannula (HFNC) or mask.
- Monitoring: Continuous cardiac and pulse oximetry.
- Targeted Rescue Therapy:
- Croup: Nebulized Adrenaline (1:1000, max 5ml); Dexamethasone (0.6 mg/kg).
- Anaphylaxis: IM Adrenaline (0.01 mg/kg of 1:1000).
- Asthma: Nebulized Salbutamol + Ipratropium; IV MgSO₄.
- Foreign Body: Heimlich maneuver → Rigid Bronchoscopy.
- Advanced Support:
- Consider Non-Invasive Ventilation (CPAP/BiPAP) for ↑ work of breathing.
- Intubate for impending respiratory failure (exhaustion, ↓ GCS, severe hypoxia/hypercarbia).
⭐ In severe croup, nebulized adrenaline provides rapid relief (10-30 min) but is temporary (~2 hrs). Always pair with steroids for their longer-lasting anti-inflammatory effect.
- The Silverman-Andersen score is crucial for assessing neonatal respiratory distress.
- Grunting is an auto-PEEP mechanism to prevent alveolar collapse; it's a key sign of distress.
- Croup presents with a barking cough and steeple sign; treat with nebulized adrenaline and steroids.
- Epiglottitis shows the thumb sign on X-ray; secure the airway immediately.
- Bronchiolitis (RSV) in infants <2 years is managed supportively; avoid routine steroids.
- Foreign body aspiration requires rigid bronchoscopy for diagnosis and removal.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

