Pre-sedation Checklist - Ready, Set, Sedate!
📌 SOAP ME
- Suction: Yankauer suction catheter, tested & ready.
- Oxygen: High-flow source, Bag-Valve-Mask (BVM).
- Airway: Appropriate size masks, oral/nasal airways, laryngoscope, Endotracheal Tubes (ETT). ETT size: $(Age/4) + 4$ (uncuffed).
- Pharmacy: Sedatives, reversal agents (e.g., Naloxone, Flumazenil), and emergency drugs drawn and labeled.
- Monitors: Continuous pulse oximetry, capnography (EtCO2), ECG, and non-invasive blood pressure (NIBP).
- Equipment: Secure IV access, emergency cart/defibrillator.
⭐ Capnography is the standard of care; it provides the earliest detection of apnea, preceding changes in pulse oximetry.
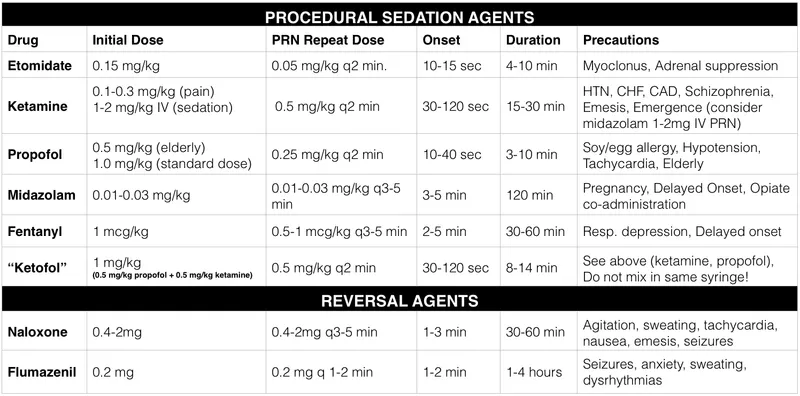
Sedation Pharmacology - The Drug Lineup
-
Ketamine (Dissociative Anesthetic)
- Dose: IV 1-2 mg/kg; IM 4-5 mg/kg.
- Action: NMDA receptor antagonist. Provides potent analgesia, amnesia, and sedation.
- Pros: Preserves airway reflexes, causes bronchodilation.
- Cons: ↑ Secretions (consider atropine), emergence reactions, transient ↑ ICP/IOP.
-
Propofol (Hypnotic Agent)
- Dose: IV 1-2 mg/kg bolus.
- Pros: Ultra-rapid onset & recovery, anti-emetic properties.
- Cons: Hypotension, respiratory depression, pain on injection. No analgesia.
- ⚠️ Risk of Propofol Related Infusion Syndrome (PRIS).
-
Midazolam (Benzodiazepine)
- Dose: IV 0.05-0.1 mg/kg.
- Provides anxiolysis & amnesia. No analgesia. Reversible with Flumazenil.
-
Fentanyl (Opioid)
- Dose: IV 1-2 mcg/kg.
- Provides potent, rapid-onset analgesia. Reversible with Naloxone.
-
"Ketofol"
- Synergistic combination of Ketamine & Propofol (typically 1:1 ratio).
- Balances hemodynamic side effects and lowers required doses of each agent.
⭐ Ketamine is the agent of choice for procedural sedation in asthmatics (due to bronchodilation) and in hypotensive patients (due to its sympathomimetic effects).
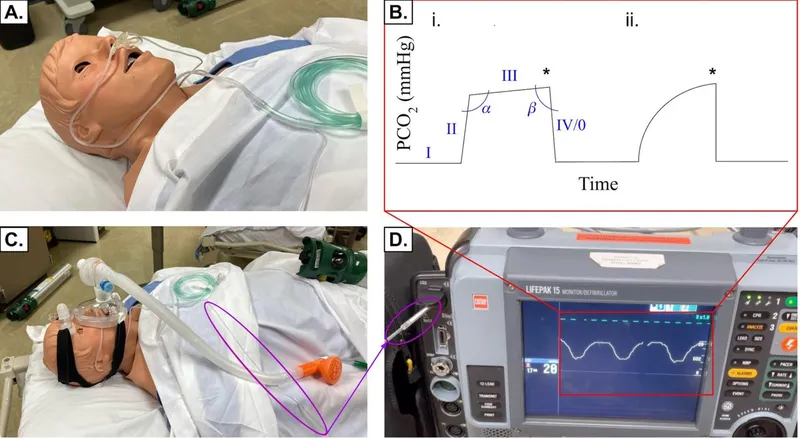
Monitoring & Rescue - The Watchful Guardian
-
Continuous Vigilance: A dedicated trained observer must monitor the child throughout.
- Vitals (HR, RR, BP) & consciousness level documented every 5-10 mins.
- Pulse Oximetry ($SpO_2$): Mandatory for all sedation levels.
- Capnography (ETCO2): The standard for detecting hypoventilation early.
-
Rescue Readiness (📌 SOAP-ME):
- Suction: Ready and available.
- Oxygen: With delivery systems (nasal cannula, bag-valve-mask).
- Airway: Oral/nasal airways, laryngoscope, ETTs.
- Pharmacy: Reversal agents (Naloxone, Flumazenil), emergency meds.
- Monitors & Equipment: As above, plus IV access.
⭐ Capnography is the most sensitive indicator of early respiratory depression, detecting apnea or hypoventilation seconds to minutes before a drop in $SpO_2$ occurs.
Complications & Reversals - Uh-Oh Moments
- Most Common: Respiratory depression (hypoventilation, apnea, hypoxia) & hypotension.
- Management:
- Airway: Jaw thrust, bag-mask ventilation.
- Circulation: IV fluid bolus.
| Drug Class | Reversal Agent | Pediatric Dose (IV/IM) |
|---|---|---|
| Opioids | Naloxone | 0.1 mg/kg; max 2 mg |
| Benzodiazepines | Flumazenil | 0.01 mg/kg; max 0.2 mg per dose |
High‑Yield Points - ⚡ Biggest Takeaways
- Pre-procedure fasting is crucial: 2 hrs for clear fluids, 4 hrs for breast milk, 6 hrs for solids.
- Capnography is the standard of care for monitoring ventilation and detecting apnea early.
- Ketamine is often preferred for its potent analgesia and preservation of airway reflexes.
- Propofol offers rapid onset and recovery but carries a high risk of hypotension and apnea.
- Always have reversal agents available: Flumazenil for benzodiazepines, Naloxone for opioids.
- Use the ASA physical status classification to stratify pre-sedation risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

