Pediatric Triage - Sorting the Smallest
- Primary Goal: Maximize survival in a Mass Casualty Incident (MCI) by sorting patients based on injury severity and resource needs.
- Key System: JumpSTART Triage
- Modified START protocol for children < 8 years or weighing < 45 kg.
- Non-ambulatory children are assessed first.
- Triage Categories & Criteria:
- GREEN (Minor): Ambulatory patients ("walking wounded").
- YELLOW (Delayed): Non-ambulatory, but RR 15-45, palpable pulse, and alert/responds to voice (AVPU: A or V).
- RED (Immediate):
- RR <15 or >45.
- Apnea responsive to 5 rescue breaths.
- No palpable pulse.
- Inappropriate posturing or unresponsive (AVPU: P or U).
- BLACK (Deceased): Apneic and pulseless, unresponsive to rescue breaths.
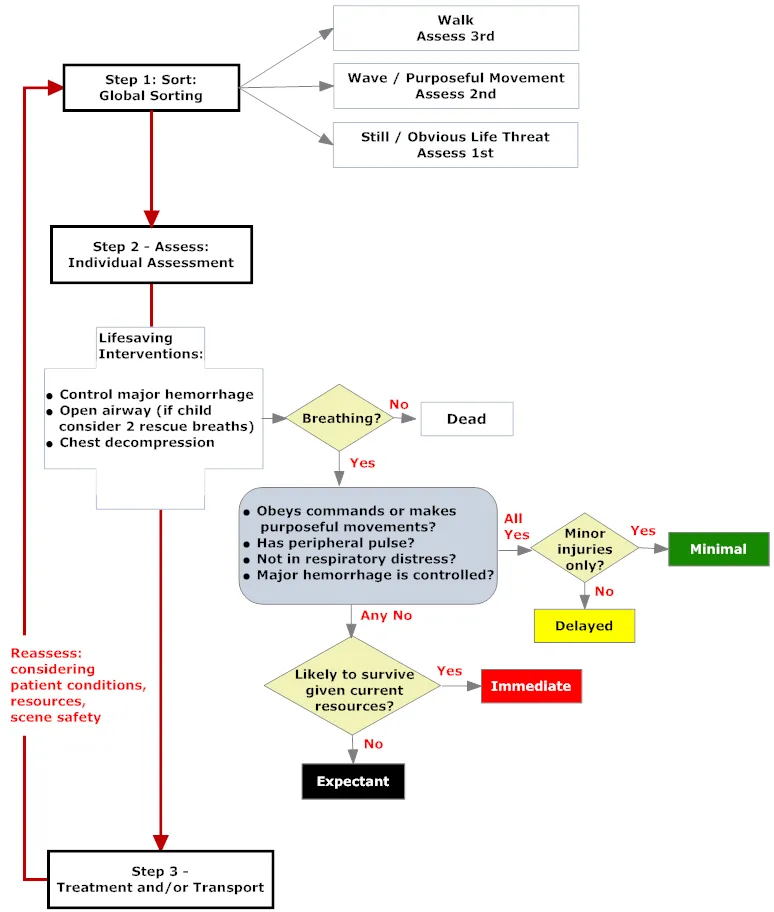
⭐ A key pediatric modification: Unlike adult START, apneic children receive 5 rescue breaths. If breathing starts, they are tagged RED (Immediate); if not, BLACK (Deceased).
Pediatric Vulnerabilities - Little Bodies, Big Risks
-
Physiological & Anatomical Differences:
- ↑BSA:Mass ratio: Leads to rapid heat loss (hypothermia) & ↑fluid loss.
- ↑Metabolic rate: Higher oxygen, fluid, and glucose demands.
- Airway: Smaller diameter, larger tongue; prone to obstruction.
- Immature immune system: ↑Susceptibility to infections.
- Thinner skin: ↑Absorption of toxins & risk of thermal injury.
- Limited glycogen/fat stores: Prone to hypoglycemia.
-
Psychosocial & Developmental Factors:
- Dependence: Rely entirely on adults for safety, transport, and needs.
- Communication: Inability to describe symptoms or locate parents.
- Psychological Trauma: Higher risk of PTSD, anxiety, and developmental regression post-disaster.
⭐ Exam Pearl: In mass casualty incidents, the Broselow Tape is a crucial tool for rapid, length-based estimation of weight, equipment sizes, and drug dosages, bypassing complex calculations under pressure.
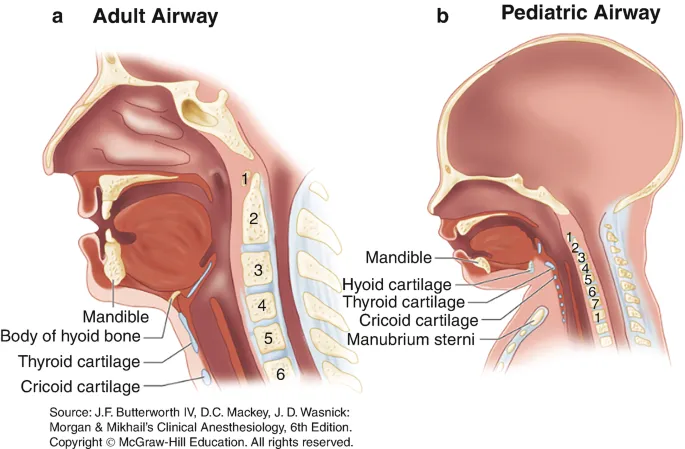
Key Management Steps - Prepare, Protect, Reunite
-
Prepare:
- Family Disaster Plan: Establish designated meeting places & out-of-state contacts.
- "Go-Bag" for Kids: Pack formula, diapers, medications, comfort items (toys), and copies of important documents (vaccination records, prescriptions).
- CSHCN: Ensure a 3-7 day supply of medications and equipment-specific power sources.
-
Protect:
- Psychological First Aid (PFA): Prioritize for all children. Use calming techniques.
- 📌 Mnemonic (The 5 S's for Infants): Swaddling, Side/Stomach position, Shushing, Swinging, Sucking.
- Decontamination: Use gentle soap and water; avoid harsh chemicals. Keep children warm to prevent hypothermia.
-
Reunite:
- Patient Tracking: Use wristbands with unique identifiers.
- Clear Communication: Establish a single point of contact for family reunification information.
⭐ High-Yield Fact: Children are not "little adults." Their unique physiology (↑ surface area-to-mass ratio, ↑ respiratory rate) makes them more vulnerable to hypothermia, dehydration, and toxins during disasters.
High‑Yield Points - ⚡ Biggest Takeaways
- For mass casualty incidents, use pediatric-specific triage systems like JumpSTART or SALT.
- The Broselow Tape is critical for rapid, weight-based drug dosing and equipment sizing.
- Children have a higher body surface area-to-mass ratio, increasing their risk of hypothermia and percutaneous toxin absorption during decontamination.
- Prioritize psychological first aid; children are highly vulnerable to the psychological stress of disasters.
- Family reunification is a primary operational goal in pediatric disaster planning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

