Suspicion & Red Flags - Seeing the Unseen
- History Discrepancies: Vague, changing, or inconsistent history; delay in seeking care; injury blamed on siblings or pets.
- Pathognomonic Injuries: Injuries inconsistent with the child's developmental stage (e.g., fracture in a non-ambulatory infant).
- Bruises: Specific patterns are key. 📌 TEN-4 FACES: Torso, Ears, Neck in child >4 yrs; Frenulum, Auricular, Cheek, Eyelids, Sclera in any child.
- Fractures: Metaphyseal corner fractures, posterior rib fractures, sternal fractures.
- Burns: Stocking-glove distribution, cigarette burns, branding patterns.

⭐ Metaphyseal corner fractures (bucket-handle fractures) are considered virtually pathognomonic of non-accidental trauma in infants.
Physical Abuse - Telltale Trauma Patterns
-
Bruising Patterns:
- 📌 TEN-4 FACES-P Mnemonic: Suspicious if on Torso, Ears, Neck in child ≥4 months; or Frenulum, Auricle, Cheeks, Eyes, Sclera, or Patterned in any child.
- Multiple bruises in different stages of healing.
- Patterned injuries: handprints, belt/loop marks.
-
High-Specificity Fractures:
- Metaphyseal corner/bucket-handle fractures.
- Posterior ribs (from squeezing).
- Scapula, sternum, spinous processes.
-
Characteristic Burns:
- Immersion burns: sharp "stocking-glove" demarcation.
- Cigarette burns: small, circular, deep.
-
Other Major Trauma:
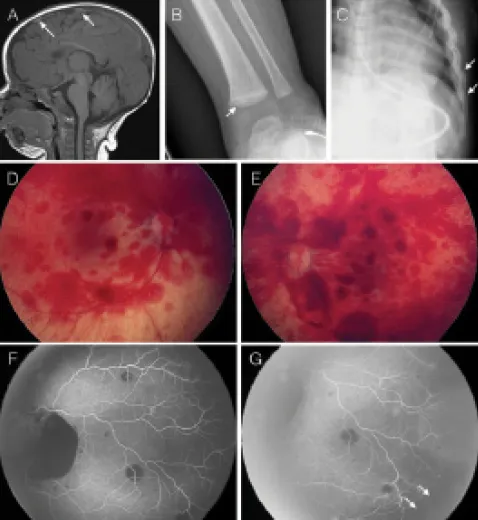
- Abusive Head Trauma (AHT): subdural hematoma, retinal hemorrhages.
- Occult abdominal injury (e.g., duodenal hematoma).
⭐ Posterior rib fractures are considered pathognomonic for child abuse until proven otherwise, often caused by forceful squeezing of the chest.
AHT & Other Abuse - Shakes, Sex & Neglect
- Abusive Head Trauma (AHT):
- Mechanism: Violent shaking → acceleration-deceleration injury.
- Key Findings:
- Subdural hemorrhage (interhemispheric fissure).
- Widespread, multi-layered retinal hemorrhages.
- Metaphyseal corner fractures, posterior rib fractures.
- Apnea, seizures, encephalopathy.
- Evaluation Flowchart:
⭐ Classic Triad of AHT: Encephalopathy, Subdural Hemorrhage, and Retinal Hemorrhages.
-
Sexual Abuse:
- Consider if STIs (e.g., Gonorrhea, Syphilis) in prepubertal child.
- Anogenital findings: acute trauma, scars, ↓ anal tone.
-
Neglect:
- Failure to thrive, poor hygiene, developmental delay.
The Workup - Proof & Protocol
- Initial Steps: Stabilize (ABCDE), then mandatory reporting to Child Welfare Committee (CWC) / Child Protective Services (CPS).
- Investigation Protocol:
- Skeletal Survey: All suspected victims <2 years. Repeat in 2 weeks to detect healing fractures.
- Neuroimaging (CT/MRI): All infants <1 year with suspected abuse, or any child with neurologic signs (seizures, ALTE).
- Ophthalmology Exam: Dilated fundoscopy for retinal hemorrhages.
- Bleeding Screen: Coagulation profile (PT/aPTT) & platelet count.
⭐ Retinal hemorrhages are highly specific for Abusive Head Trauma (AHT), but their absence does not rule it out.

High-Yield Points - ⚡ Biggest Takeaways
- Most common fracture is a skull fracture; most specific is a metaphyseal corner fracture.
- Posterior rib, scapular, and sternal fractures are also highly specific for non-accidental trauma.
- Shaken Baby Syndrome triad: subdural hemorrhage, retinal hemorrhages, and encephalopathy.
- Multiple bruises in varying stages of healing are highly suspicious; dating individual bruises is unreliable.
- A skeletal survey is mandatory for suspected physical abuse in children < 2 years old.
- Suspected child abuse is a legally reportable offense for all healthcare providers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

