Allergy vs. Intolerance - The Great Mix-Up
| Feature | Food Allergy | Food Intolerance |
|---|---|---|
| Mechanism | Immune-mediated (IgE/Non-IgE) | Non-immune (e.g., enzyme defect) |
| Onset | Rapid (mins to 2 hrs) | Gradual (hours to days) |
| Amount | Minute quantity | Dose-dependent |
| Symptoms | Systemic, Anaphylaxis possible | Primarily GI (bloating, diarrhea) |

Common Culprits & Features - The Usual Suspects
- Infancy & Early Childhood: Cow's milk, soy, eggs, wheat.
- Older Children & Adults: Peanuts, tree nuts (cashews, walnuts), fish, shellfish.
Reaction Types:
- IgE-Mediated (Rapid Onset): Urticaria, angioedema, wheezing, vomiting, anaphylaxis within minutes to <2 hours.
- Non-IgE-Mediated (Delayed): Chronic diarrhea, vomiting, FPIES (Food Protein-Induced Enterocolitis Syndrome), eczema flare. Onset >2 hours to days.

⭐ Cow's milk protein allergy (CMPA) is the most common food allergy in infants and young children, presenting with both IgE and non-IgE mediated symptoms.
Diagnostic Workup - The Allergy Detective
- Allergy-focused history: The cornerstone. Inquire about timing, symptoms, reproducibility, and dietary details.
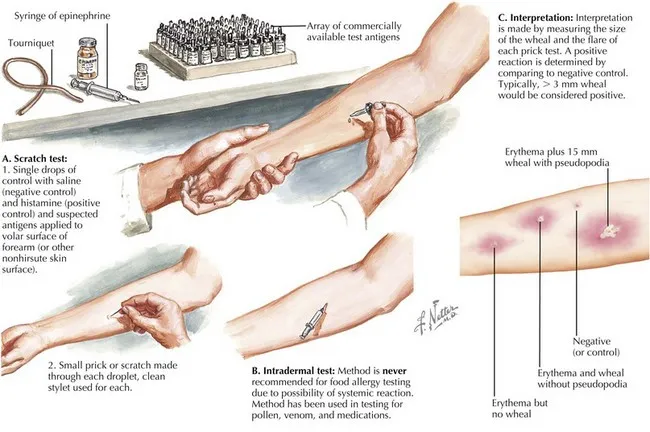
- Skin Prick Test (SPT):
- Wheal >3 mm than negative control is positive.
- Quick, sensitive, but risk of false positives.
- Specific IgE (sIgE) Test:
- Blood test; positive if >0.35 kU/L.
- Safer if risk of anaphylaxis with SPT.
⭐ Gold Standard: The Double-Blind, Placebo-Controlled Food Challenge (DBPCFC) is the definitive method for diagnosing a food allergy.
Key Syndromes - The Special Cases
- FPIES (Food Protein-Induced Enterocolitis Syndrome):
- Non-IgE mediated; presents at 2-6 months.
- Profuse, repetitive vomiting 1-4 hrs post-ingestion → dehydration, lethargy, shock.
- Triggers: Cow's milk, soy, rice, oats.
- Heiner Syndrome:
- Food hypersensitivity pulmonary hemosiderosis (rare).
- Triad: Pulmonary infiltrates, hemosiderosis (hemoptysis), and iron deficiency anemia with cow's milk allergy.
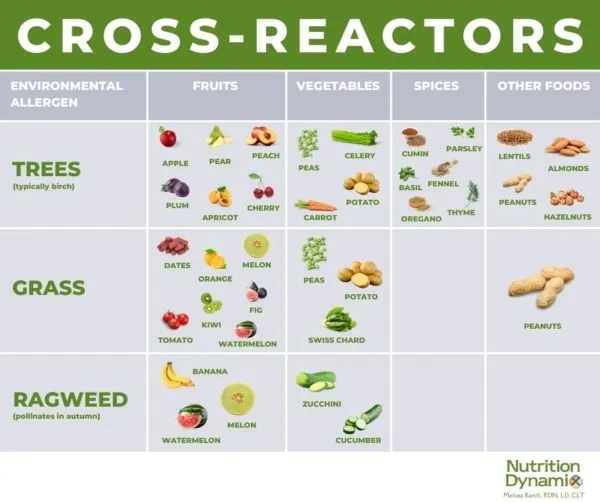
- Oral Allergy Syndrome (OAS):
- Pollen-food allergy; IgE-mediated.
- Itching/tingling of mouth/throat with raw fruits/veg.
⭐ FPIES is a clinical diagnosis; allergy tests (skin prick, specific IgE) are typically negative.
Management & Prevention - The Action Plan
- Core Strategy: Strict dietary avoidance of the offending food allergen.
- Written Emergency Plan: Essential for patients, families, and schools.
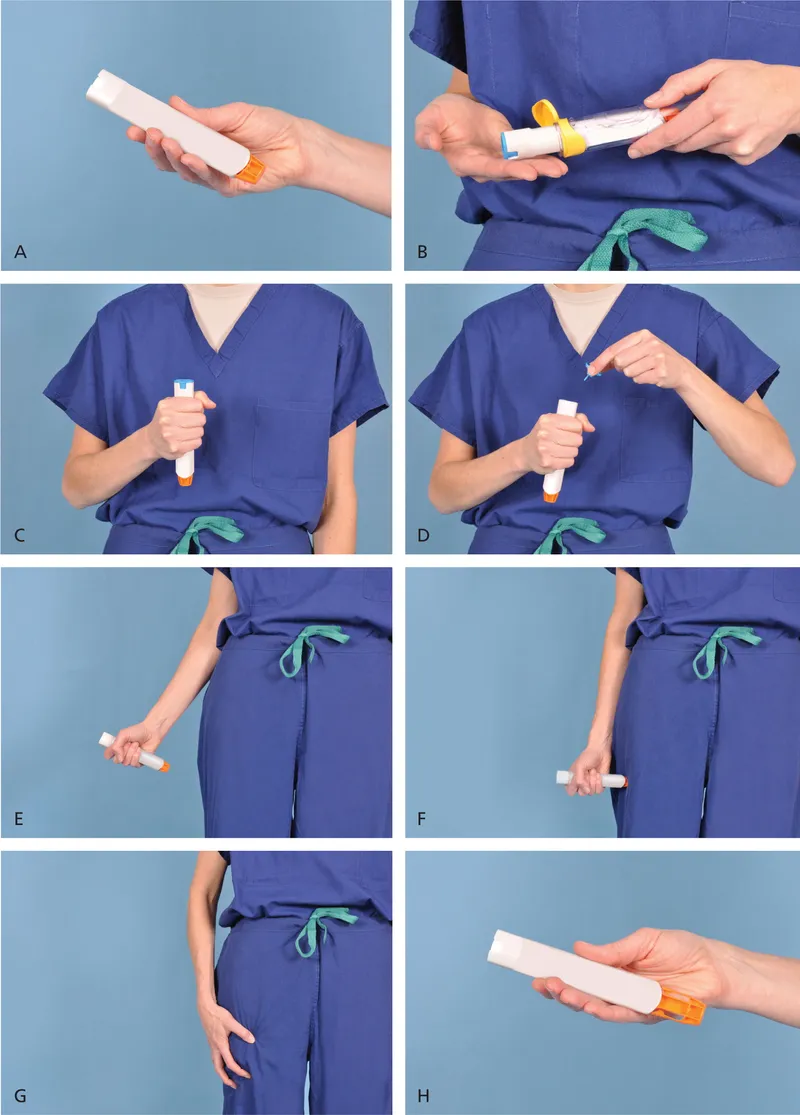
- Anaphylaxis: Immediate intramuscular Epinephrine (0.01 mg/kg of 1:1000, max 0.5 mg) is life-saving.
- Oral Immunotherapy (OIT): Medically supervised desensitization is an emerging option.
⭐ A biphasic reaction (second wave of anaphylaxis) can occur 1-72 hours after the initial reaction, requiring prolonged observation.
High‑Yield Points - ⚡ Biggest Takeaways
- Cow's milk protein allergy (CMPA) is the most common food allergy in infancy, typically resolving by age 5.
- Most reactions are IgE-mediated (Type I hypersensitivity), with rapid onset of urticaria, angioedema, or anaphylaxis.
- The gold standard for diagnosis is a physician-supervised Oral Food Challenge (OFC).
- Food Protein-Induced Enterocolitis Syndrome (FPIES) is a severe, non-IgE-mediated gut allergy causing delayed vomiting and lethargy.
- Lactose intolerance is a non-immune reaction due to lactase deficiency, diagnosed via a hydrogen breath test.
- Strict allergen avoidance is key; epinephrine is the first-line treatment for anaphylaxis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

