IEM Basics - Metabolic Mayhem
- Core Defect: Monogenic enzyme/transporter deficiency → substrate accumulation or product deficiency.
- Classic Presentation: Acutely ill neonate mimicking sepsis. Key features: poor feeding, vomiting, lethargy, seizures, altered sensorium.
- Initial Lab Red Flags:
- Hypoglycemia
- Metabolic acidosis (especially with ↑ anion gap)
- Hyperammonemia
- Ketosis (or inappropriate absence of ketones)
⭐ Suspect an IEM in any term neonate with a sepsis-like picture but negative cultures.
Carbohydrate Disorders - Sugar Rush Gone Wrong
-
Galactosemia (GALT deficiency): Presents in neonates after milk feeds.
- Features: Jaundice, hepatomegaly, vomiting, cataracts, FTT.
- Dx: ↑ Galactose-1-P in RBCs; reducing substances in urine.
- Rx: Lifelong lactose-free diet.
⭐ High-Yield: Classic Galactosemia is strongly associated with E. coli neonatal sepsis.
-
Hereditary Fructose Intolerance (Aldolase B deficiency): Symptoms start with weaning (fruits/honey).
- Features: Hypoglycemia, vomiting, jaundice, hepatomegaly.
- Rx: Avoid fructose, sucrose, sorbitol.
-
Glycogen Storage Diseases (GSDs):
- Type I (von Gierke): G6Pase def. Severe fasting hypoglycemia, lactic acidosis, hepatomegaly, doll-like face.
- Type II (Pompe): α-glucosidase def. Cardiomegaly, hypotonia, macroglossia.
- Type V (McArdle): Muscle phosphorylase def. Exercise intolerance, cramps, myoglobinuria.
- 📌 Mnemonic: McArdle = Muscle.

Amino Acidopathies - Protein Problems
- Phenylketonuria (PKU): Deficient Phenylalanine Hydroxylase → ↑ Phe.
- Features: Musty/mousy odor, intellectual disability, seizures, eczema.
- Screening: Guthrie test / Mass spectrometry. Rx: Low Phe diet.
- Maple Syrup Urine Disease (MSUD): Deficient Branched-Chain α-ketoacid Dehydrogenase.
- ↑ BCAAs (Leucine, Isoleucine, Valine). 📌 I Love Vermont maple syrup.
- Features: Urine/cerumen smells of burnt sugar; neurotoxic.
- Homocystinuria: Deficient Cystathionine β-synthase → ↑ Homocysteine & Methionine.
- Rx: ↓ Met, ↑ Cys diet; Vitamin B6 (pyridoxine).
- Alkaptonuria: Deficient Homogentisate Oxidase.
- Urine turns black on standing; ochronosis (dark cartilage/sclera), arthritis.
⭐ Homocystinuria vs. Marfan Syndrome: Both have marfanoid habitus & ectopia lentis. Homocystinuria features intellectual disability, thrombosis, and downward lens dislocation (vs. upward in Marfan's).

Lysosomal Storage - Cellular Cleanup Crisis
- Pathophysiology: Inherited defects in lysosomal hydrolase enzymes → accumulation of undigested substrates → cellular dysfunction & organ damage.
- Key Types:
- Gaucher: ↓ Glucocerebrosidase. Hepatosplenomegaly, pancytopenia, bone crises. Gaucher cells (crinkled paper cytoplasm).
- Tay-Sachs: ↓ Hexosaminidase A. Cherry-red spot, neurodegeneration. NO hepatosplenomegaly.
- Niemann-Pick: ↓ Sphingomyelinase. Cherry-red spot, hepatosplenomegaly. Foam cells.
- Fabry: X-Linked Recessive. ↓ α-galactosidase A. Angiokeratomas, neuropathic pain, renal failure.
- Hurler (MPS I): ↓ α-L-iduronidase. Coarse facies, corneal clouding, dysostosis multiplex.
⭐ Gaucher Disease is the most common LSD. Diagnosis is confirmed by finding lipid-laden macrophages with a characteristic "crinkled tissue paper" appearance.

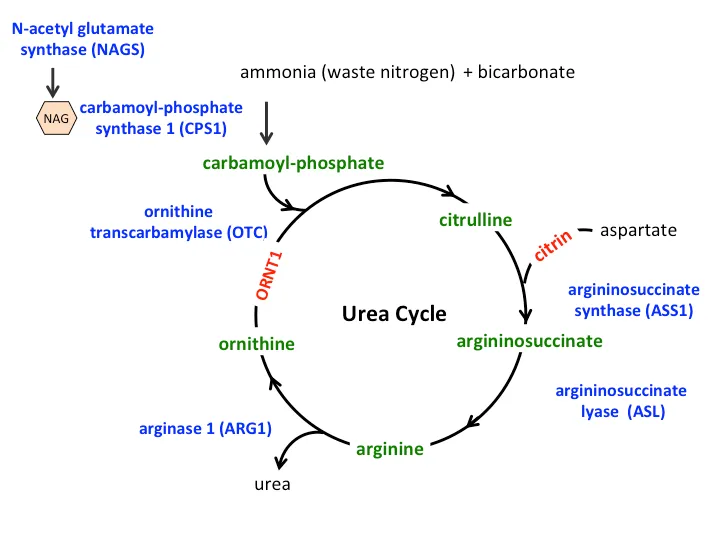
Urea Cycle & Acidemias - Ammonia Alert
- Presentation: Neonatal encephalopathy (lethargy, seizures, coma), vomiting. Key lab: ↑ Ammonia.
- Key Differentiation: Acid-base status is crucial.
- Organic Acidemias (Methylmalonic, Propionic): Severe high anion gap metabolic acidosis.
- Urea Cycle Defects (OTC deficiency): Primary respiratory alkalosis, minimal acidosis.
⭐ Ornithine Transcarbamylase (OTC) deficiency is the most common urea cycle disorder and is X-linked recessive.
High‑Yield Points - ⚡ Biggest Takeaways
- PKU: Presents with a characteristic mousy odor, fair skin, and eczema; neonatal screening is key.
- Galactosemia: Features include jaundice, cataracts, and reducing substances in the urine.
- MSUD: Characterized by maple syrup odor in urine, poor feeding, and encephalopathy.
- Homocystinuria: Look for Marfanoid habitus, downward lens dislocation, and a high risk of thrombosis.
- Von Gierke's (GSD-I): Severe fasting hypoglycemia, lactic acidosis, and massive hepatomegaly.
- Tay-Sachs: Cherry-red spot, developmental regression, and hyperacusis, but no hepatosplenomegaly.
- Gaucher Disease: Presents with massive hepatosplenomegaly, pancytopenia, and bone crises.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

