Genomic Medicine - Editing Our Code
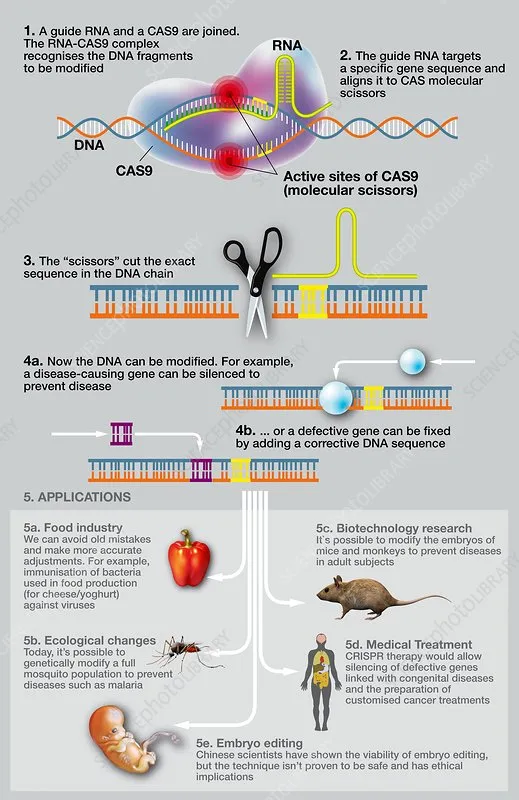
- Core Technology: CRISPR-Cas9 enables precise DNA modification to correct pathogenic mutations.
- Key Ethical Distinction:
- Somatic Editing: Affects only the individual (non-heritable). Ethically viewed similarly to advanced medical treatments.
- Germline Editing: Alters sperm, eggs, or embryos. Changes are permanent and heritable, impacting future generations.
- Primary Ethical Issues:
- Safety: Risk of off-target mutations and unforeseen long-term health consequences.
- Consent: Inability to obtain consent from future generations for germline changes.
- Justice: Concerns over equitable access and creating a genetic class divide ("designer babies").
⭐ High-Yield Point: The fundamental ethical boundary in gene editing is between somatic (non-heritable, therapeutic) and germline (heritable) modifications. US regulations currently restrict federal funding for research involving heritable human germline editing.
AI & Robotics - Rise of Robot Docs
-
AI in Medicine: Double-Edged Sword
- Benefits: ↑Precision in diagnostics (radiology), analyzing massive datasets, potential to ↓human error.
- Risks: Algorithmic bias from non-diverse training data, patient data privacy (HIPAA), "black box" decision-making, physician deskilling.
-
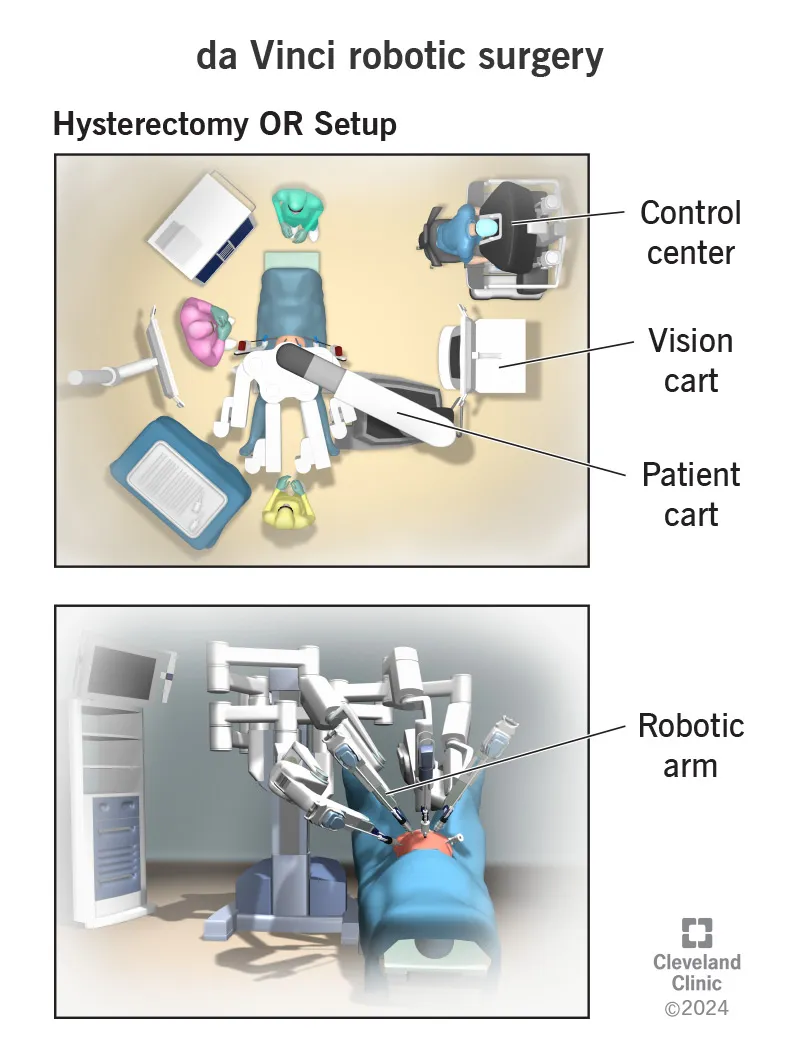
Robotic Surgery (e.g., Da Vinci)
- Pros: Enhanced dexterity, tremor filtration, minimally invasive approaches.
- Cons: High cost, loss of haptic feedback, steep learning curve, rare but critical mechanical failures.
-
Core Ethical & Legal Challenges
- Accountability: Who is liable for an AI-driven error? The clinician, hospital, or developer?
- Informed Consent: How to adequately explain AI's role and risks to patients.
- Justice: Ensuring equitable access and avoiding a two-tiered system of care.
⭐ The FDA regulates many AI systems as Software as a Medical Device (SaMD). A primary concern is that biased training data can cause AI to perpetuate or even amplify existing health disparities in minority populations.
Telehealth & Big Data - The Virtual Patient
-
Telehealth: Remote healthcare delivery via telecommunication.
- Benefits: ↑ Access to care, patient convenience, potential cost savings.
- Ethical/Legal Hurdles:
- Privacy/Security: Platforms must be HIPAA-compliant to protect against data breaches.
- Digital Divide: Can worsen health disparities for patients lacking tech access/literacy.
- Licensure: Physicians must be licensed in the state where the patient is located.
-
Big Data/AI in Medicine: Analyzing large health datasets to predict outcomes.
- Challenges:
- Algorithmic Bias: Models trained on non-representative data can perpetuate inequities.
- Accountability: Determining liability for AI-driven medical errors.
- Challenges:
⭐ High-Yield: A major telehealth challenge is maintaining the standard of care, ensuring it is equivalent to an in-person consultation, particularly for making a new diagnosis.
Reproductive Technologies - Designer Baby Dilemmas
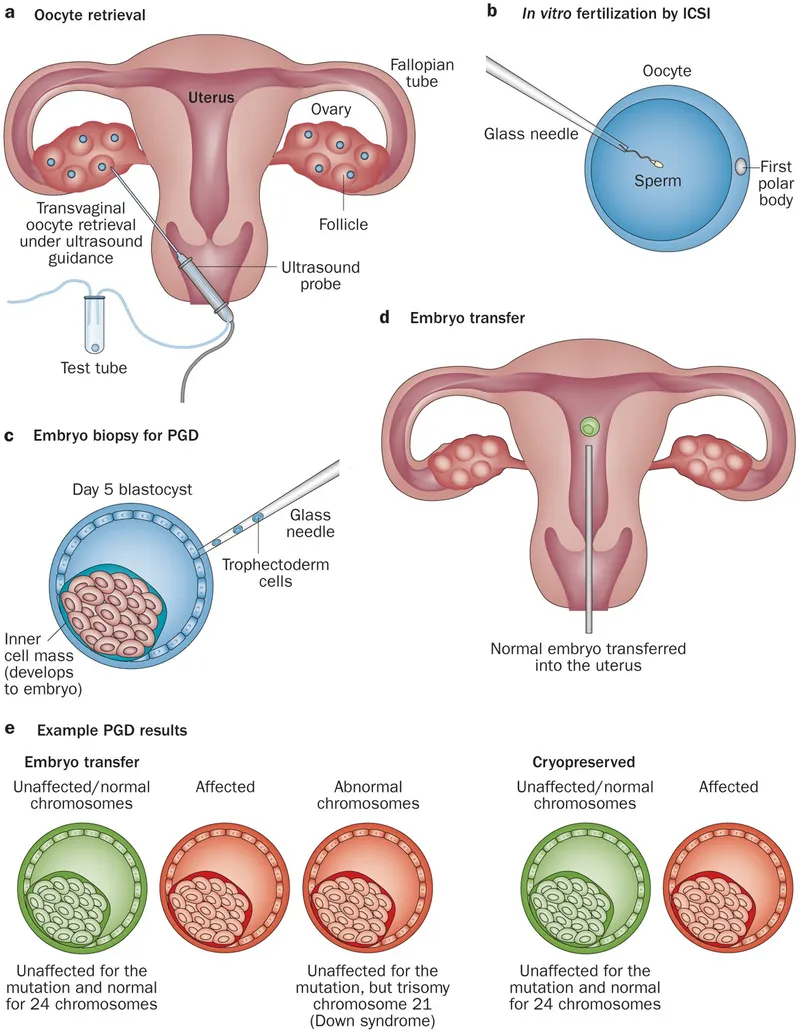
- Preimplantation Genetic Diagnosis (PGD): Screening embryos for monogenic diseases (e.g., Cystic Fibrosis, Huntington's) or chromosomal abnormalities before implantation.
- **Ethical Pros (Proponents' View):
- Beneficence: Prevents suffering from severe genetic disorders.
- Autonomy: Respects parental rights to make reproductive choices.
- **Ethical Cons (Opponents' View):
- Non-Maleficence: Potential for unforeseen long-term health risks from manipulation.
- Justice: High cost may lead to genetic inequity, creating a "genetically privileged" class.
- "Slippery Slope": Transitioning from disease prevention to non-medical trait enhancement (e.g., intelligence, appearance).
⭐ The core ethical conflict lies in distinguishing between therapy (acceptable use to prevent disease) and enhancement (controversial use to select for desired traits), which raises fears of modern eugenics.
High‑Yield Points - ⚡ Biggest Takeaways
- Telemedicine requires strict HIPAA compliance for data security and physicians must be licensed in the patient's state.
- AI algorithms carry risks of inherent bias, "black box" opacity, and unclear accountability for errors.
- EHRs can compromise patient privacy and propagate errors through careless use of features like copy-paste.
- Genomic medicine requires clear informed consent regarding incidental findings and protection from genetic discrimination (GINA).
- Determining liability for errors in robotic surgery or with AI-assisted diagnosis is a major ethical and legal challenge.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

