Informed Consent - The Starting Line
- Foundation: An ethical and legal mandate for physician-patient communication before any medical intervention. Ensures patient autonomy.
- Core Components:
- Disclosure: Patient receives all necessary information (diagnosis, prognosis, risks, benefits, alternatives, and nature of the intervention).
- Capacity: Patient demonstrates the ability to comprehend information and rationally use it to make a decision.
- Voluntariness: The decision is made freely, without coercion or manipulation.
⭐ In a true emergency where the patient lacks capacity and no surrogate is available, consent is implied to prevent imminent harm, loss of life, or limb.
Cultural Beliefs - Culture Clash
-
Individualism vs. Collectivism:
- Western medicine emphasizes patient autonomy.
- Many cultures prioritize family-centered or community decision-making; patients may defer to family elders or a spokesperson.
- Action: Identify the key decision-maker(s) with the patient's consent.
-
Communication & Trust:
- Language barriers are a major obstacle. Avoid using family members as interpreters.
- Historical events (e.g., Tuskegee) may fuel distrust in the healthcare system among minority groups.
- Address concerns with empathy and transparency to build rapport.
⭐ High-Yield Fact: When a patient refuses information, citing cultural norms ("My family will decide"), it is crucial to first offer to share information directly with them before involving the family. This respects their right to know, even if they choose to waive it.
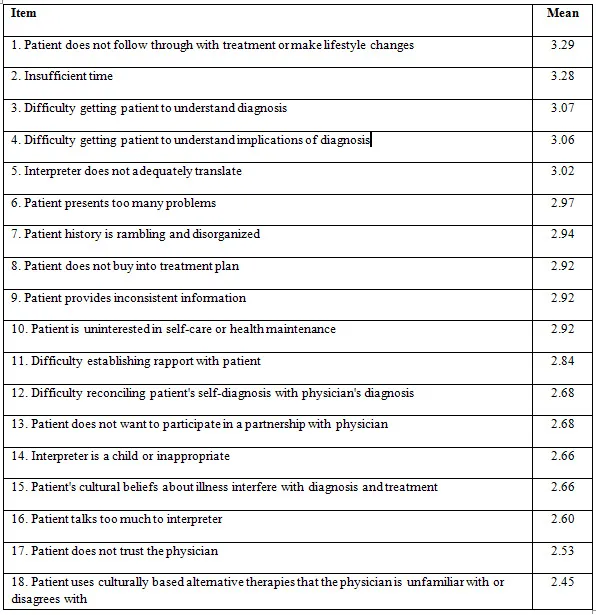
- Differing Health Beliefs:
- Patients may have alternative explanatory models for illness (e.g., spiritual, humoral).
- Explore these beliefs respectfully to find common ground for the treatment plan.
Communication Tools - Talk the Talk
- Cultural Humility: Approach each patient with a willingness to learn about their beliefs and values without making assumptions. Acknowledge and respect differences.
- Qualified Medical Interpreters:
- Legally required for patients with limited English proficiency (LEP).
- Use professional interpreters, not family or friends, to ensure accuracy and confidentiality.
- Teach-Back Method:
- Ask the patient to explain the information back in their own words.
- "Can you tell me what you understand about the procedure?"
- Shared Decision-Making:
- Collaborate with the patient (and family, if appropriate) to make healthcare choices that align with their values.
⭐ Always use a qualified medical interpreter for patients with Limited English Proficiency (LEP). Using family members (especially children) is a common pitfall; it can lead to errors, confidentiality breaches, and compromised consent.
High‑Yield Points - ⚡ Biggest Takeaways
- In some cultures, family or community involvement in decision-making may be prioritized over individual autonomy.
- Always use qualified medical interpreters; avoid using family members to prevent misinterpretation, breaches of confidentiality, or coercion.
- Acknowledge and respect diverse cultural beliefs about illness, healing, and the role of traditional medicine.
- Historical context can create distrust in the healthcare system; build rapport patiently.
- Directly ask the patient about their preferred decision-making process.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

