ADPKD - Adult Polycystic Mayhem
- Genetics: Autosomal dominant. Mutation in PKD1 (chromosome 16, ~85%) or PKD2 (chromosome 4, ~15%), coding for polycystin-1 or -2.
- Pathophysiology: Numerous cysts in all parts of the nephron cause bilateral, massive kidney enlargement.
- Clinical Triad: Presents in adulthood (40s-50s) with flank pain, hematuria, and hypertension (early, due to RAAS activation), leading to progressive renal failure.
- Extra-renal Manifestations:
- Hepatic cysts (most common)
- Berry aneurysms (Circle of Willis)
- Mitral valve prolapse
- Colonic diverticula
⭐ Exam Favorite: Rupture of a berry aneurysm is a major cause of death, leading to subarachnoid hemorrhage. Screen symptomatic patients or those with a family history of aneurysms.
📌 Mnemonic: Pain, Kidneys massive, Diverticula/aneurysms.

ARPKD - Recessive Renal Rumpus
- Genetics: Autosomal recessive mutation in the PKHD1 gene (chromosome 6), affecting the fibrocystin protein.
- Pathology:
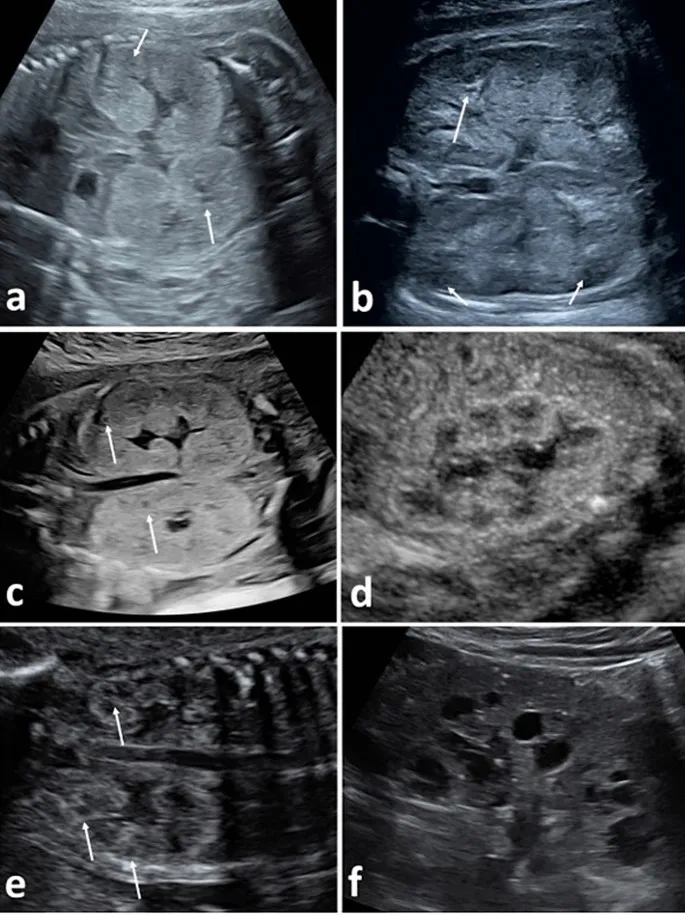
- Bilaterally enlarged, echogenic kidneys with a smooth surface.
- Cysts are elongated, arising from collecting ducts and arranged radially.
- Clinical Presentation:
- Presents in infancy or in utero.
- Severe cases may show Potter sequence (oligohydramnios, pulmonary hypoplasia).
- Systemic hypertension and progressive renal insufficiency.
⭐ High-Yield: ARPKD is invariably associated with congenital hepatic fibrosis, which can lead to portal hypertension.
📌 Mnemonic: Autosomal Recessive Potter Kidney Disease (links inheritance, common severe outcome, and organ).
Medullary Mix-up - Spongy vs. Cystic
| Feature | Medullary Sponge Kidney (MSK) | Medullary Cystic Kidney Disease (MCKD) |
|---|---|---|
| Etiology | Sporadic, developmental anomaly | Autosomal Dominant (AD) |
| Pathology | Dilated papillary collecting ducts | Cysts at corticomedullary junction, fibrosis |
| Kidney Size | Normal or enlarged | Shrunken kidneys |
| Key Finding | Incidental; recurrent kidney stones | Salt wasting, progressive renal failure |
| Prognosis | Benign | Leads to end-stage renal disease (ESRD) |
⭐ Key Distinction: MCKD is a progressive disease causing tubulointerstitial fibrosis, leading to shrunken kidneys and significant salt wasting, unlike the benign, normal-sized kidneys in MSK.
Acquired Cysts - Dialysis & Danger
- Develops in patients with end-stage renal disease, strongly associated with long-term dialysis (especially >3-5 years).
- Native kidneys are often shrunken/atrophic but develop multiple bilateral cortical and medullary cysts.
- ⚠️ High risk of malignant transformation. The primary danger is a significantly increased incidence of renal cell carcinoma (RCC), which can be bilateral and multifocal.
⭐ The risk of developing RCC in dialysis patients with acquired cystic disease is up to 7% over 10 years, a substantial increase over the general population.
- Autosomal Dominant Polycystic Kidney Disease (ADPKD) results from PKD1/PKD2 mutations, causing bilaterally enlarged kidneys, hypertension, and pain in adults.
- Key ADPKD extrarenal findings include berry aneurysms, hepatic cysts, and mitral valve prolapse.
- Autosomal Recessive (ARPKD) presents in infancy, often with Potter sequence, and is linked to congenital hepatic fibrosis.
- Medullary Cystic Kidney Disease causes tubulointerstitial fibrosis, leading to shrunken kidneys and eventual renal failure.
- Acquired cystic disease occurs in chronic dialysis patients, increasing their risk for renal cell carcinoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

