Neutrophils - First Responder Firefight
-
Primary Role: Acute inflammation's first responders, arriving in 6-24 hours.
-
Key Features: Multi-lobed nucleus, granular cytoplasm. Phagocytose, degranulate, and release Neutrophil Extracellular Traps (NETs).
-
Recruitment: Follows a specific sequence:
-
Chemotaxis: Migrate toward specific signals. 📌 Mnemonic: CILK - C5a, IL-8, LTB4, Kallikrein.
-
Killing: Use phagocytosis and respiratory burst ($O_2 ightarrow O_2^{\cdot-}$ via NADPH oxidase).
⭐ Leukocyte Adhesion Deficiency (LAD): Defect in integrins (CD18) impairs adhesion. Presents with delayed umbilical cord separation, recurrent bacterial infections, and neutrophilia without pus formation.
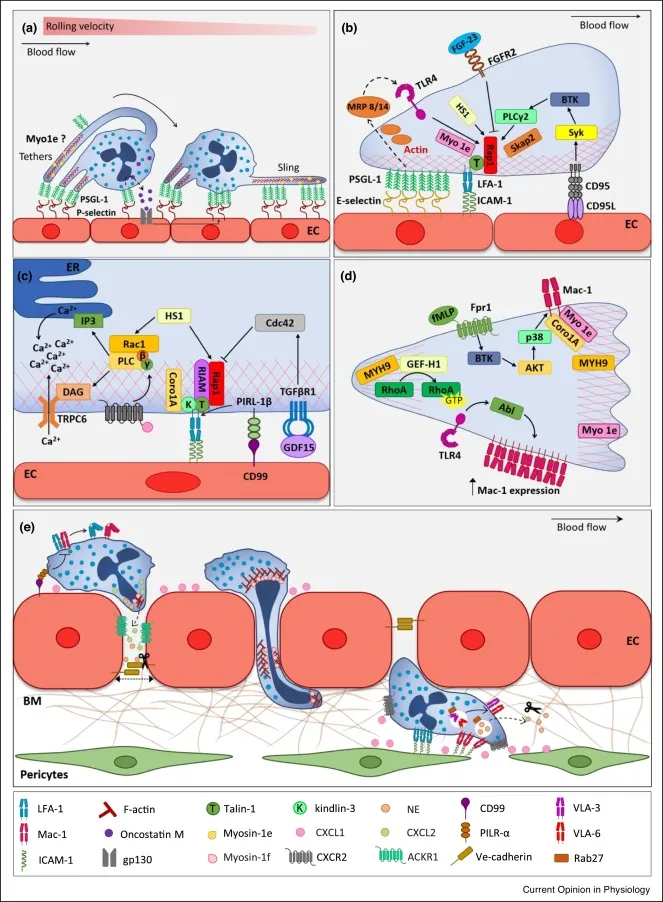
Macrophages - Clean-up & Command
- Arrival: Monocytes migrate from blood, becoming macrophages in tissue 24-48 hours post-injury, succeeding neutrophils.
- Core Functions:
- Phagocytosis: Engulf cellular debris, pathogens, and dead neutrophils.
- Antigen Presentation: Process and present antigens to helper T-cells, linking innate and adaptive immunity.
- Orchestration: Secrete cytokines (TNF, IL-1, IL-6) to manage inflammation and initiate healing.
- Activation Pathways:
- M1 (Classical): Pro-inflammatory; activated by IFN-γ. Destroys microbes.
- M2 (Alternative): Anti-inflammatory; activated by IL-4, IL-13. Drives tissue repair and fibrosis.
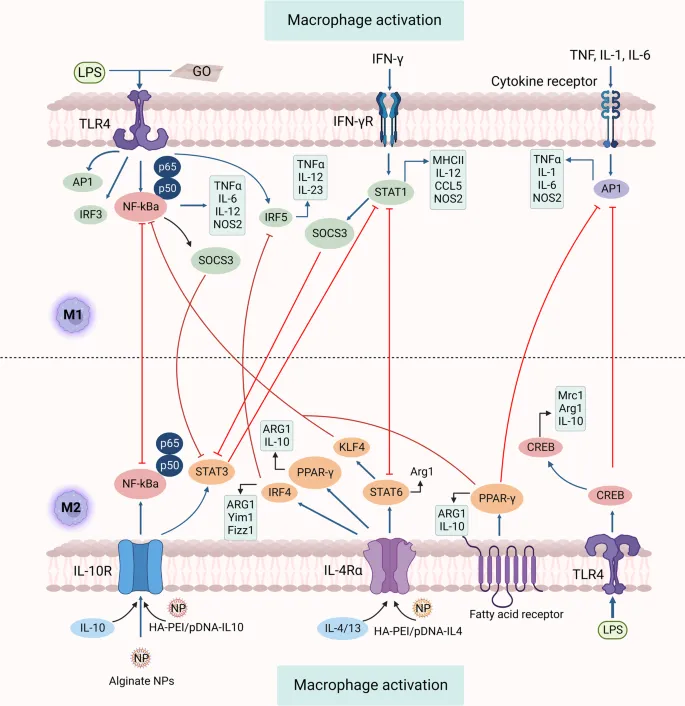
⭐ In granulomatous inflammation (e.g., Tuberculosis), macrophages transform into epithelioid cells and can fuse to form multinucleated giant cells.
Leukocyte Extravasation - The Great Escape
The sequential process of leukocytes exiting the vasculature to reach tissues. It's a critical component of acute inflammation, guided by specific adhesion molecules and chemokines.
📌 Mnemonic: "Rolling, Adhesion, Diapedesis, Migration"
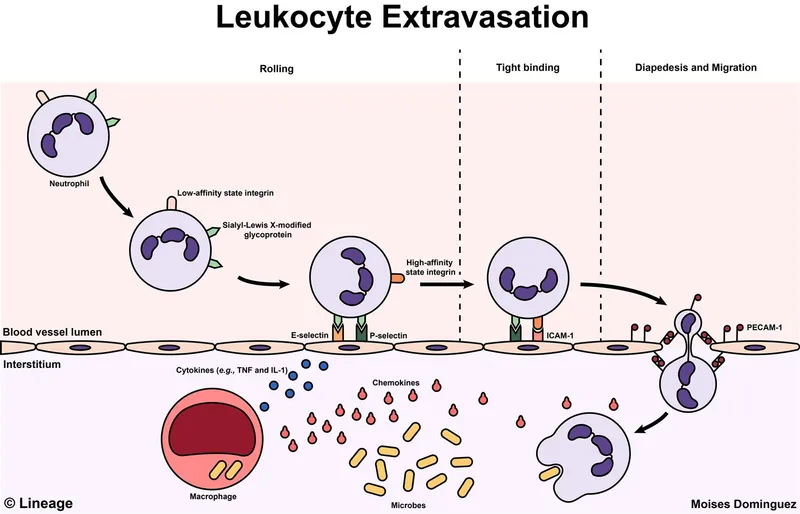
- Rolling: Mediated by low-affinity selectin binding.
- Adhesion: Firm attachment via high-affinity integrins.
- Transmigration: Squeezing between endothelial cells.
- Migration: Movement along a chemotactic gradient.
⭐ Leukocyte Adhesion Deficiency (LAD-1): An autosomal recessive defect in the CD18 subunit of integrins. Presents with recurrent bacterial infections without pus, poor wound healing, delayed umbilical cord separation, and marked neutrophilia.
Other Cells - Specialized Forces
-
Mast Cells & Basophils:
- Sentinel cells in connective tissue; activated by IgE, C3a/C5a, trauma.
- Release preformed histamine granules → vasodilation & ↑ vascular permeability.
- Central to Type I hypersensitivity reactions.
-
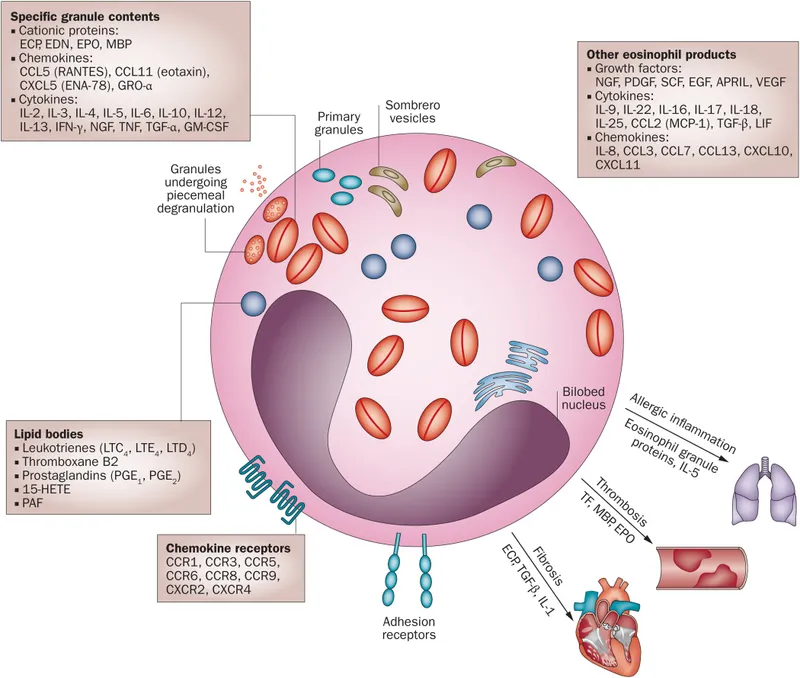
Eosinophils:
- Combat helminthic parasites and modulate allergic reactions.
- Granules contain Major Basic Protein (MBP), toxic to parasites.
-
Lymphocytes & Plasma Cells:
- Key drivers of chronic inflammation and the adaptive immune response.
⭐ Eosinophil granules contain crystalloid bodies, which can form Charcot-Leyden crystals, a classic finding in asthmatic sputum.
High‑Yield Points - ⚡ Biggest Takeaways
- Neutrophils are the first responders in acute inflammation, phagocytosing bacteria.
- Macrophages arrive in 24-48 hours, driving chronic inflammation and presenting antigens.
- Lymphocytes (T & B cells) are hallmarks of chronic inflammation and adaptive immunity.
- Eosinophils are characteristic of allergic reactions and parasitic infections.
- Mast cells and basophils release histamine, mediating vasodilation and increased permeability.
- Giant cells are fused macrophages, pathognomonic for granulomatous inflammation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

