IHC Principles - Staining the Unseen
- A technique to visualize specific antigens (proteins) in tissue sections by binding them to highly specific antibodies.
- The core principle is an antigen-antibody (Ag-Ab) reaction.
- An enzyme (e.g., peroxidase) is linked to the antibody.
- When a substrate (chromogen) is added, the enzyme creates a colored precipitate at the antigen's site.
- This allows for the precise localization and identification of cellular components.
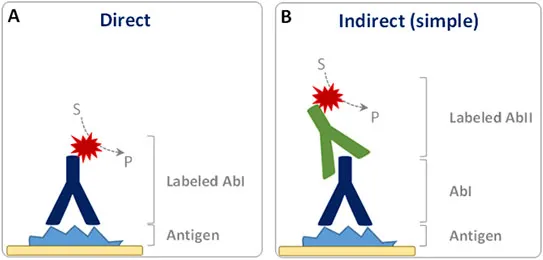
⭐ The most common chromogen used is Diaminobenzidine (DAB), which produces a characteristic brown stain, indicating the presence of the target antigen.
IHC Technique - A Staining Story
- Antigen Retrieval: Unmasks antigen epitopes hidden by formalin fixation. Methods: Heat-Induced (HIER) or Proteolytic-Induced (PIER).
- Blocking: Prevents non-specific background staining from endogenous enzymes or proteins.
- Primary Antibody: Monoclonal or polyclonal antibody that binds specifically to the target antigen.
- Secondary Antibody: Binds to the primary antibody. Conjugated to an enzyme (e.g., Horseradish Peroxidase - HRP).
- Chromogen & Counterstain: Substrate (e.g., DAB) forms a colored precipitate at the antigen site. Hematoxylin counterstain provides context.
⭐ The detection system often uses the high-affinity bond between biotin and avidin/streptavidin to amplify the signal, which dramatically increases the sensitivity of the assay.
Key Markers - The Cellular Lineup
| Marker | Cell / Tumor Type | Notes |
|---|---|---|
| Cytokeratin | Epithelial cells (Carcinomas) | Distinguishes carcinoma from sarcoma. |
| Vimentin | Mesenchymal cells (Sarcomas) | Connective tissue, muscle, endothelium. |
| Desmin | Muscle (Myosarcomas) | Rhabdomyosarcoma, Leiomyosarcoma. |
| GFAP | Neuroglia (Astrocytoma, Glioblastoma) | Glial Fibrillary Acidic Protein. |
| Neurofilament | Neurons (Neuroblastoma) | Differentiates from other small round blue cell tumors. |
| S-100 | Neural crest cells | Melanoma, Schwannoma, Langerhans cell histiocytosis. |
| CD45 | All Leukocytes (Lymphoma, Leukemia) | Also known as Leukocyte Common Antigen (LCA). |
| CD20, CD19 | B-cells (B-cell lymphomas) | CD20 is a target for Rituximab. |
| CD3, CD4, CD8 | T-cells (T-cell lymphomas) | Coreceptors for T-cell recognition. |
Clinical Use - Decoding the Colors
-
Diagnosis & Differentiation
- Distinguishes broad tumor types: Cytokeratin (Carcinoma), Vimentin (Sarcoma), LCA (Lymphoma).
- Identifies cell lineage in poorly differentiated neoplasms.
- Pinpoints origin of metastatic tumors (e.g., PSA for prostate, TTF-1 for lung).
-
Prognosis
- Gauges tumor aggressiveness.
- Ki-67: Measures proliferation rate (↑ Ki-67 = poorer prognosis).
- HER2/neu overexpression indicates aggressive disease.
-
Predictive Markers (Therapy Guidance)
- Guides targeted treatment selection.
- ER/PR status in breast cancer predicts response to hormone therapy.
- HER2 positivity predicts response to Trastuzumab.
⭐ IHC is crucial for evaluating a "Carcinoma of Unknown Primary" (CUP). A tumor positive for TTF-1 and Napsin-A strongly suggests a lung adenocarcinoma primary, guiding focused treatment.
High‑Yield Points - ⚡ Biggest Takeaways
- IHC is a cornerstone technique using antibodies to detect specific antigens (proteins) in tissue, primarily for tumor diagnosis and classification.
- Cytokeratin is the classic marker for carcinomas (epithelial tumors), while vimentin is characteristic of sarcomas (mesenchymal tumors).
- S-100 is a key marker for melanoma, schwannomas, and other neural crest-derived tumors.
- CD markers (e.g., CD20 for B-cells, CD3 for T-cells) are essential for subtyping lymphomas and leukemias.
- IHC identifies prognostic and predictive markers, such as ER/PR and HER2 in breast cancer, to guide targeted therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

