GI Uprisings - Tummy Troubles Takedown
-
Nausea & Vomiting (NVP) / "Morning Sickness"
- Initial: Lifestyle changes (small, frequent meals; avoid triggers like spicy/fatty foods), ginger, acupressure.
- First-line pharmacotherapy: Pyridoxine (Vitamin B6) +/- Doxylamine.
- Second-line: Antihistamines (Dimenhydrinate, Diphenhydramine).
- Refractory: Dopamine antagonists (Metoclopramide) or Serotonin antagonists (Ondansetron).
- ⚠️ Ondansetron: Use with caution in 1st trimester; small ↑ risk of cardiac malformations & orofacial clefts.
-
Gastroesophageal Reflux Disease (GERD)
- Initial: Lifestyle (elevate head of bed, avoid eating 2-3 hrs before sleep).
- Pharmacotherapy: Antacids (Calcium Carbonate) → H2-receptor blockers (Famotidine) → Proton Pump Inhibitors (Omeprazole) for severe/refractory cases.
⭐ Hyperemesis Gravidarum: Suspect if patient has persistent vomiting, weight loss >5% of pre-pregnancy body weight, ketonuria, and electrolyte abnormalities. Requires IV hydration and antiemetics.
Musculoskeletal Malaise - Aches, Pains & Strains
-
Low Back Pain: Exaggerated lumbar lordosis & hormonal joint laxity (↑ relaxin, progesterone).
- Management: Pelvic tilt exercises, proper posture, supportive shoes, maternity support belt.
- Avoid NSAIDs, especially in the 3rd trimester. Acetaminophen is preferred.
-
Round Ligament Pain: Sharp, stabbing pain in the lower abdomen or groin, often with sudden movements (e.g., rolling in bed). Usually occurs in the 2nd trimester.
- Management: Reassurance, positional changes, local heat.
-
Symphysis Pubis Dysfunction (SPD): Severe pelvic girdle pain, waddling gait. Worsened by weight-bearing activities.
- Management: Pelvic support garments, physical therapy, activity modification.
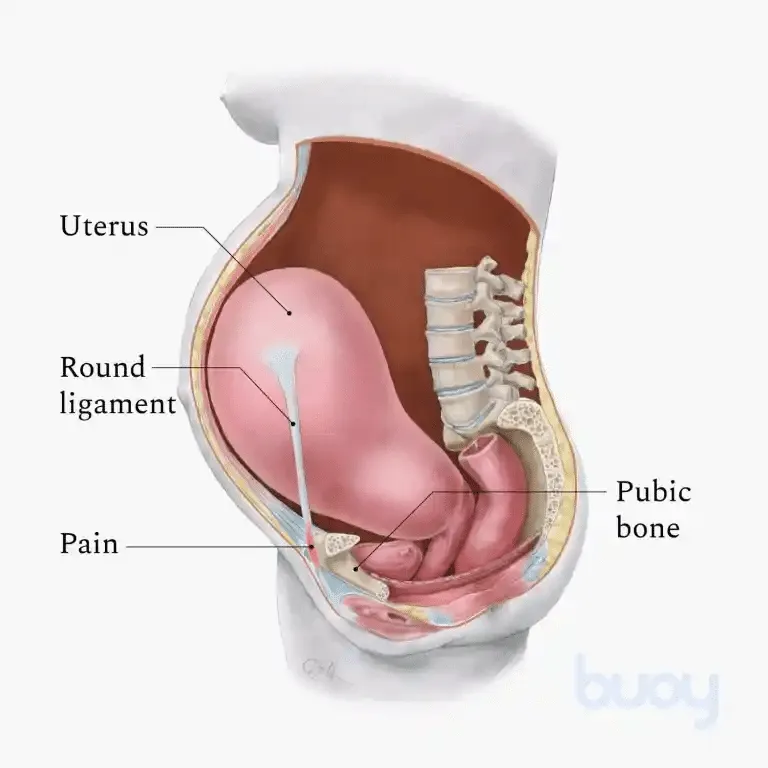
⭐ Exam Favorite: Round ligament pain is a diagnosis of exclusion. Always rule out more serious causes like appendicitis, placental abruption, or preterm labor if pain is severe, rhythmic, or associated with other systemic symptoms.
Systemic Stresses - Plumbing & Pressure
-
Edema & Varicosities
- Pathophysiology: Progesterone → venous dilation; Uterine growth → IVC & pelvic vein compression → ↑ hydrostatic pressure.
- Presentation: Swelling in legs, ankles, feet. Vulvar varicosities & hemorrhoids are common.
- Management:
- Leg elevation, compression stockings.
- Sleep in left lateral decubitus position to relieve IVC compression.
- For hemorrhoids: sitz baths, topical anesthetics, stool softeners.
- ⚠️ Red Flag: Sudden, unilateral, or painful swelling may indicate DVT. Facial/hand edema can signal preeclampsia.
-
Gastroesophageal Reflux (GERD)
- Pathophysiology: Progesterone relaxes the lower esophageal sphincter (LES).
- Management: Lifestyle (small meals, avoid triggers) → Antacids (calcium carbonate) → H2 blockers or PPIs.
-
Constipation
- Pathophysiology: Progesterone ↓ gut motility; iron supplementation exacerbates.
- Management: ↑ Fiber & fluid intake, exercise. Stool softeners (docusate) are first-line.
⭐ Supine Hypotensive Syndrome: In late pregnancy, the gravid uterus compresses the IVC when supine, reducing venous return & cardiac output, causing hypotension and dizziness. Management is immediate repositioning to the left lateral decubitus position.
High‑Yield Points - ⚡ Biggest Takeaways
- Nausea/vomiting: First-line is vitamin B6 ± doxylamine. For severe cases (hyperemesis gravidarum), use IV fluids and antiemetics.
- GERD: Start with lifestyle modifications. If persistent, use calcium carbonate.
- Constipation: Managed with increased fiber, fluids, and exercise. Docusate is a safe stool softener.
- Asymptomatic bacteriuria: Always treat in pregnancy to prevent pyelonephritis. Common antibiotics include nitrofurantoin and cephalexin.
- Low back pain: Treat with acetaminophen, proper posture, and pelvic tilt exercises.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

