Fetal Movement - Feeling the Kicks
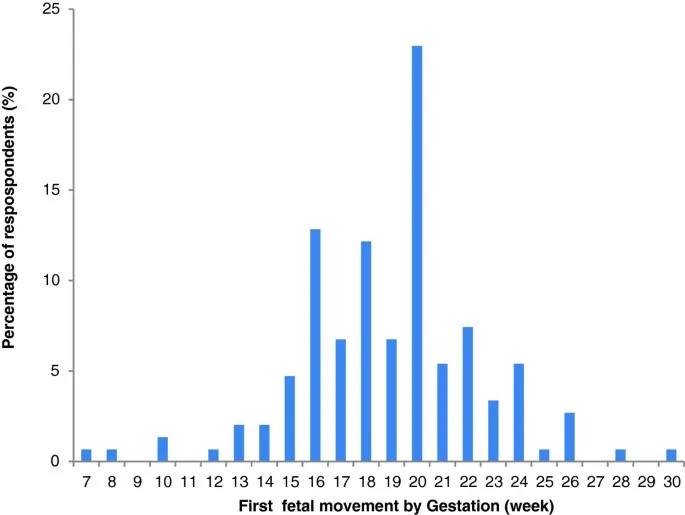
- Quickening: First maternal perception of fetal movement.
- Primigravida: 18-20 weeks
- Multigravida: 16-18 weeks
- Perception is subjective and can be affected by anterior placenta, amniotic fluid index (AFI), and maternal BMI.
- Decreased Fetal Movement (DFM): Subjective reduction in activity from the fetus's established baseline.
⭐ A key screening approach is the "count to 10" (Cardiff method): feeling 10 distinct movements within 2 hours is considered reassuring.
Kick Count Methods - Counting the Wiggles
Formal fetal movement assessment, or 'kick counts,' is a key method for monitoring fetal well-being, typically initiated around 28 weeks of gestation. The mother quantifies fetal movements to detect potential hypoxia early.
| Method | Procedure | Alarm Threshold |
|---|---|---|
| Cardiff ("Count to 10") | Time how long it takes to feel 10 distinct fetal movements. | > 2 hours to feel 10 movements. |
| Sadovsky | Count movements for 1 hour, three times per day, usually after meals. | < 4 movements per hour. |
* Perform counts at the same time each day, when the baby is typically active.
* Lie on the left side to enhance uterine perfusion.
⭐ A maternal report of Decreased Fetal Movement (DFM) always warrants further investigation, starting with a Non-Stress Test (NST).
DFM Workup - When Kicks Quiet Down
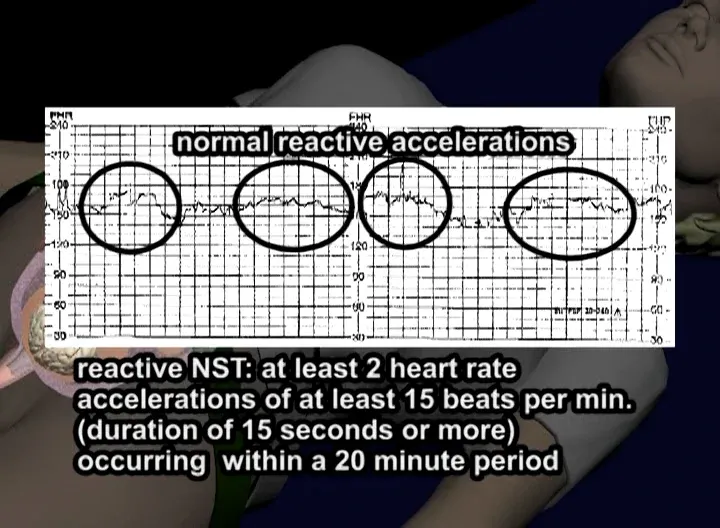
Initial management for decreased fetal movement (DFM) is a stepwise process to assess for fetal hypoxia and prevent stillbirth. The primary goal is to rule out acidosis.
- Umbilical Artery (UA) Doppler: Crucial in fetal growth restriction (IUGR) cases to assess placental perfusion. Absent or reversed end-diastolic flow is an ominous sign.
⭐ The Biophysical Profile (BPP) is an "ultrasound Apgar." It assesses 5 components, each getting a score of 0 or 2: Fetal breathing, Gross body movements, Fetal tone, Amniotic fluid index (AFI), and the NST itself.
Etiology of DFM - The Silent Culprits
- Fetal
- Benign: Normal sleep-wake cycles (most common, up to 40 min).
- Pathologic: CNS depression (hypoxia, acidosis), congenital anomalies, infection, demise.
- Placental
- Insufficiency (leading to IUGR), abruption.
- Maternal
- Medications: CNS depressants like sedatives, opioids.
- Substances: Smoking, alcohol.
- Conditions: Obesity, dehydration.
⭐ An anterior placenta can mask fetal movements, making it a frequent cause for benign maternal concern.
High‑Yield Points - ⚡ Biggest Takeaways
- Decreased fetal movement (DFM) is a critical sign requiring immediate evaluation to rule out fetal compromise.
- Maternal monitoring ("kick counts") typically starts at 28 weeks; a normal count is ≥10 movements in 2 hours.
- The first step for reported DFM is a Nonstress Test (NST).
- A non-reassuring NST prompts a Biophysical Profile (BPP) or Contraction Stress Test (CST).
- Underlying causes often relate to uteroplacental insufficiency, leading to fetal hypoxia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

