MTP Activation - Sounding the Alarm
- Trigger: Activate for persistent hemodynamic instability despite initial resuscitation, or when blood loss is massive and ongoing (e.g., >1500 mL or requiring >4 units PRBCs rapidly).
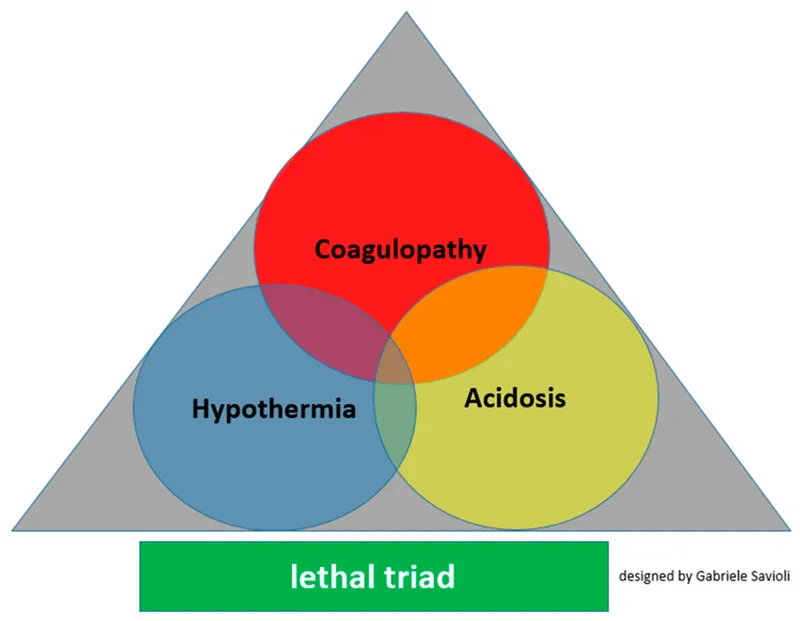
- Goal: Prevent the lethal triad of acidosis, hypothermia, and coagulopathy.
- Protocol: Transfuse packed red blood cells (PRBCs), fresh frozen plasma (FFP), and platelets in a balanced 1:1:1 ratio to mimic whole blood and prevent dilutional coagulopathy.
⭐ For every 1-minute delay in MTP initiation after its criteria are met, the relative risk of mortality increases significantly.
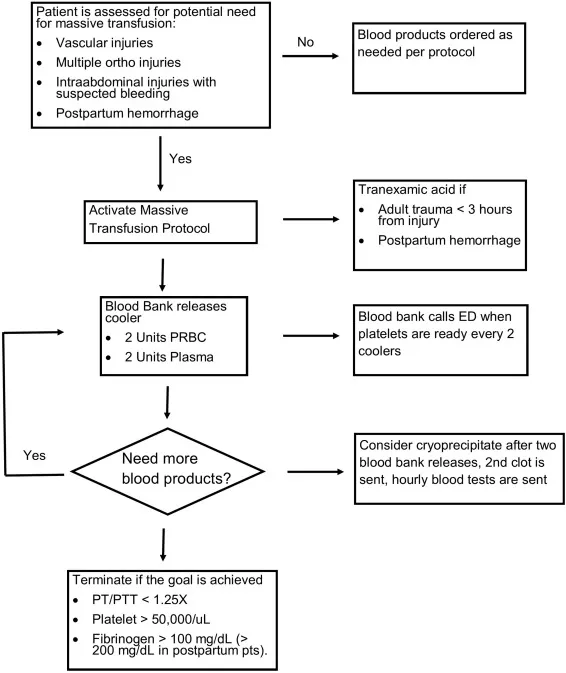
Blood Products - The Rescue Ratio
- Massive Transfusion Protocol (MTP): Activated in severe, ongoing PPH to combat coagulopathy, acidosis, and hypothermia.
- Core Strategy: Balanced resuscitation mimicking whole blood. The goal is a 1:1:1 ratio of:
- Packed Red Blood Cells (PRBCs)
- Fresh Frozen Plasma (FFP)
- Platelets
- Tranexamic Acid (TXA): An antifibrinolytic crucial for stabilizing clots.
- Administer 1 g IV slowly within 3 hours of bleeding onset.
- Cryoprecipitate: Consider if fibrinogen remains low (< 200 mg/dL) despite FFP.
⭐ The WOMAN trial showed that early TXA administration reduces mortality due to bleeding in PPH without increasing the risk of thromboembolic events.
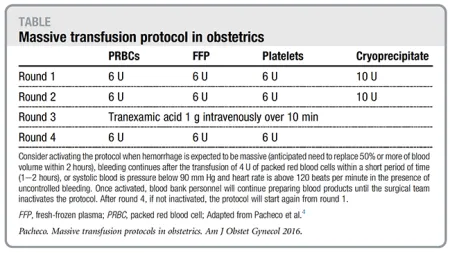
Adjuncts & Monitoring - The Supporting Cast
- Tranexamic Acid (TXA):
- Give 1g IV within 3 hours of delivery.
- Antifibrinolytic; reduces bleeding-related mortality.
- Correct Hypocalcemia:
- Citrate in blood products chelates Ca²⁺ → myocardial depression.
- Give 1g calcium gluconate IV for every 4 units PRBCs.
- Lab-Guided Resuscitation:
- Monitor: CBC, PT/INR, fibrinogen, ABG (lactate, pH), electrolytes.
- Goals:
- Fibrinogen >200 mg/dL
- Platelets >50,000/μL
- INR <1.5
- pH >7.2
- Maintain normothermia (>35°C).
⭐ The Lethal Triad: Be vigilant for the vicious cycle of acidosis, hypothermia, and coagulopathy. Actively warming the patient and correcting metabolic derangements is as critical as transfusion itself.
Transfusion Risks - Dodging Complications
- Acute Hemolytic: ABO incompatibility (clerical error). Fever, flank pain, hemoglobinuria.
- Febrile Non-Hemolytic (FNHTR): Most common reaction. Due to cytokines from donor leukocytes. Prevent with leukoreduction.
- Allergic/Anaphylactic: Ranges from urticaria to shock. Check for IgA deficiency in severe cases.
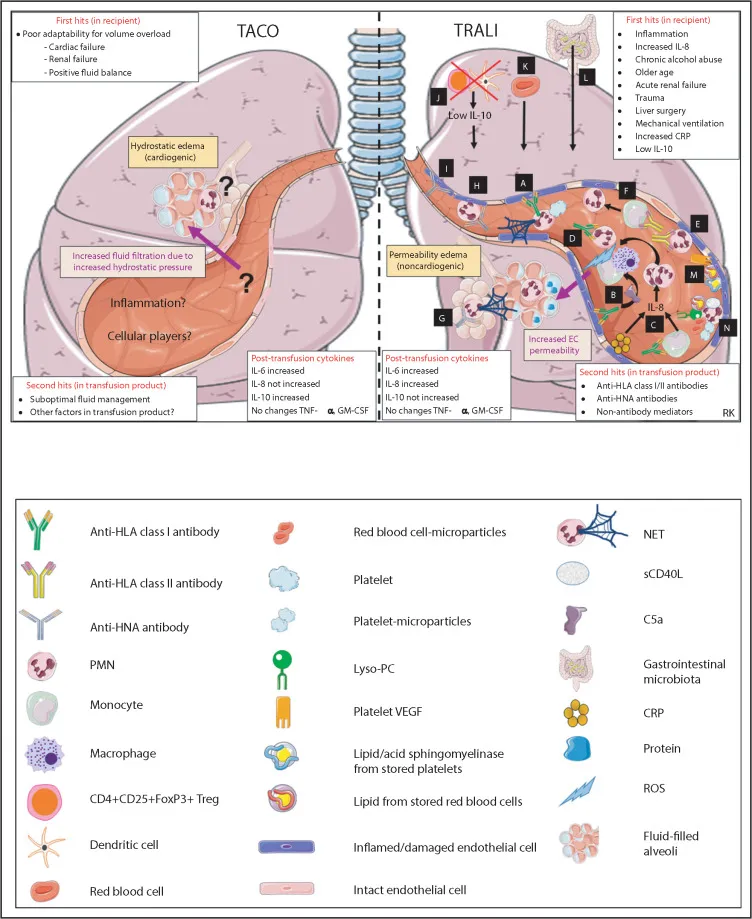
- TRALI (Transfusion-Related Acute Lung Injury): Donor antibodies vs. recipient neutrophils. Hypoxemia & non-cardiogenic pulmonary edema within 6 hours.
- TACO (Transfusion-Associated Circulatory Overload): Volume overload. Presents like heart failure (↑ JVP, pulmonary edema); improves with diuretics.
⭐ TRALI is a leading cause of transfusion-related mortality. Differentiate from TACO by lack of circulatory overload signs (e.g., normal BNP, no response to diuretics).
High‑Yield Points - ⚡ Biggest Takeaways
- Activate Massive Transfusion Protocol (MTP) for severe hemorrhage, using a balanced 1:1:1 ratio of Packed RBCs:FFP:Platelets.
- The primary goal is maintaining hemodynamic stability and tissue oxygenation, not chasing specific lab targets.
- Administer tranexamic acid (TXA) as early as possible (ideally within 3 hours) to reduce bleeding through antifibrinolytic action.
- Replace fibrinogen with cryoprecipitate if levels fall below 150-200 mg/dL.
- Monitor closely for transfusion complications like TACO, TRALI, and hypocalcemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

