Diagnosis - Water Break Whodunit
- Initial Steps:
- Sterile Speculum Exam: Visualize for pooling of fluid.
- Nitrazine Test: Amniotic fluid is alkaline (pH > 6.5), turning paper blue. ⚠️ False positives: blood, semen, BV.
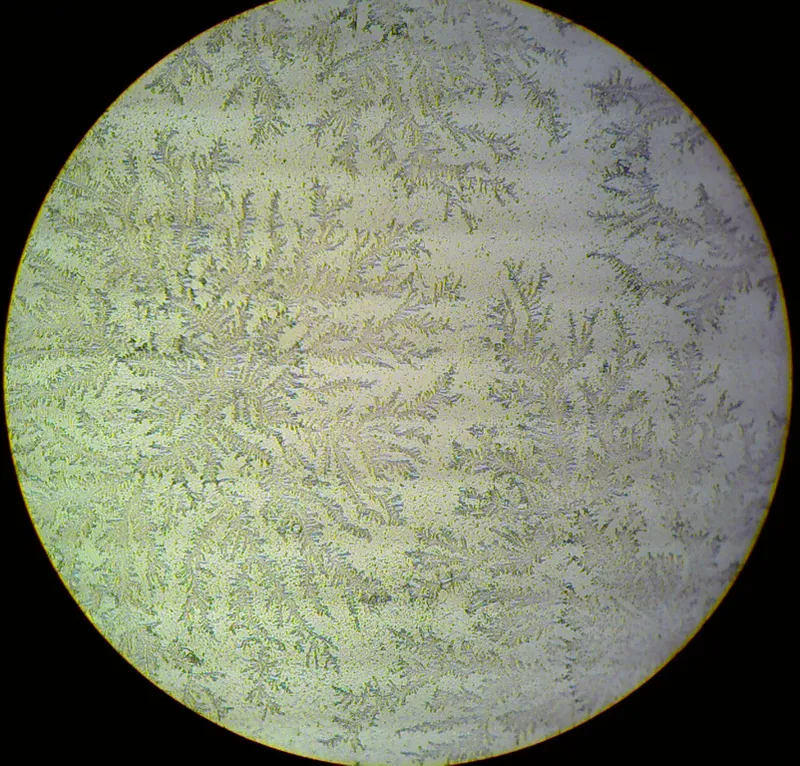
- Fern Test: Fluid air-dries on a slide, showing a crystallization pattern (arborization). Most specific office test.
- If Diagnosis Unclear:
- Ultrasound: Assess for oligohydramnios (AFI < 5 cm).
⭐ The fern test is highly specific for amniotic fluid, as the characteristic arborization pattern is caused by the crystallization of amniotic salts and proteins when dried.
Etiology & Risks - The Weak Link
- Infection: The primary driver, weakening membranes.
- Ascending genital tract infections (e.g., bacterial vaginosis)
- UTIs, chorioamnionitis
- Uterine Overdistension / Stress:
- Polyhydramnios, multiple gestation
- Iatrogenic/Traumatic:
- Amniocentesis, cervical surgery (LEEP, conization)
- Intrinsic Membrane Weakness:
- Prior PPROM, smoking, nutritional deficiencies (Vit C, copper)
⭐ A history of PPROM in a prior pregnancy is the single strongest predictor for recurrence.
Complications - Danger Zone Delivery
- Maternal Risks:
- Chorioamnionitis: Most common; intra-amniotic infection.
- Placental abruption: Can cause severe hemorrhage.
- Endometritis & retained placenta post-delivery.
- Fetal/Neonatal Risks:
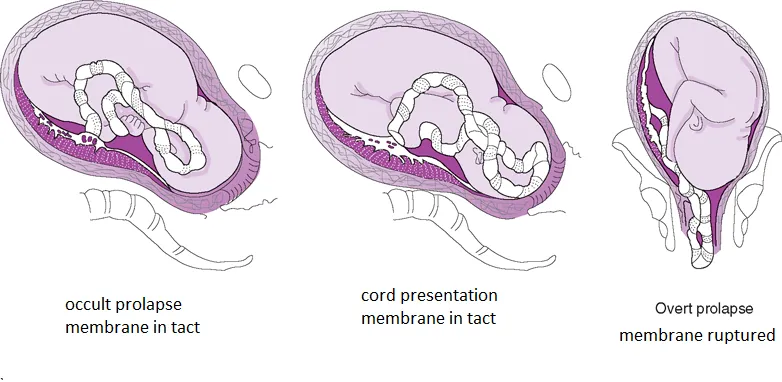
- Umbilical Cord Prolapse: EMERGENCY requiring immediate C-section.
- Pulmonary Hypoplasia: High risk if rupture <24 weeks.
- Prematurity: Major cause of RDS, IVH, NEC.
- Infection: Neonatal sepsis, pneumonia.
⭐ Chorioamnionitis is the most frequent major complication. Suspect with maternal fever, uterine tenderness, maternal or fetal tachycardia, and purulent amniotic fluid.
Management - The Ticking Clock
Management hinges on gestational age and presence of infection or fetal distress.
- Expectant Management (<34 wks):
- Corticosteroids (e.g., Betamethasone): For fetal lung maturity.
- Latency Antibiotics (e.g., Ampicillin + Azithromycin): To prolong pregnancy.
- Magnesium Sulfate: If <32 wks for fetal neuroprotection.
⭐ In PPROM, latency antibiotics are given to prolong the interval to delivery and reduce neonatal infectious morbidity, not primarily to treat maternal infection.
High-Yield Points - ⚡ Biggest Takeaways
- Rupture of membranes before labor onset is the defining feature.
- Diagnose with a sterile speculum exam showing amniotic fluid pooling, a positive nitrazine test (turns blue), and microscopic ferning.
- The greatest risks are intra-amniotic infection (chorioamnionitis) and preterm labor.
- At term (≥37 weeks), proceed to delivery and induce labor.
- For PPROM <34 weeks, manage expectantly with latency antibiotics (e.g., ampicillin, azithromycin) and corticosteroids for fetal lung maturity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

