Vaccine Types - The Immunity Arsenal
-
Live-Attenuated Vaccines
- Mechanism: Weakened pathogen that replicates in the host.
- Immunity: Strong, lifelong; humoral (IgA/IgG) & cell-mediated.
- Cons: Risk of disease in immunocompromised; reversion to virulence.
- 📌 "LIVE! See SMALL YELLOW CHICKENS get vaccinated with SABIN and MMR!" (Smallpox, Yellow Fever, Chickenpox, Sabin Polio, MMR). Also: Rotavirus, Influenza (intranasal).
-
Killed-Inactivated Vaccines
- Mechanism: Pathogen is killed/inactivated; cannot replicate.
- Immunity: Mainly humoral (IgG); less robust, requires boosters.
- Pros: Safer, no reversion risk.
- Examples: Rabies, Influenza (shot), Polio (Salk), Hepatitis A (RIP-A).
-
Subunit/Recombinant Vaccines
- Mechanism: Includes only specific antigenic components (e.g., surface protein).
- Immunity: Good humoral response; requires adjuvants.
- Pros: Very safe, minimal side effects.
- Examples: Hepatitis B, HPV, Pertussis (acellular).
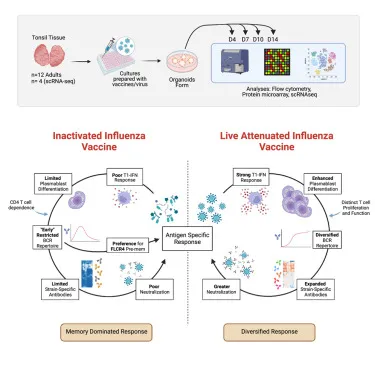
⭐ Live attenuated vaccines induce both humoral and cell-mediated immunity, mimicking natural infection. Inactivated vaccines primarily stimulate a humoral (antibody) response and may require boosters.
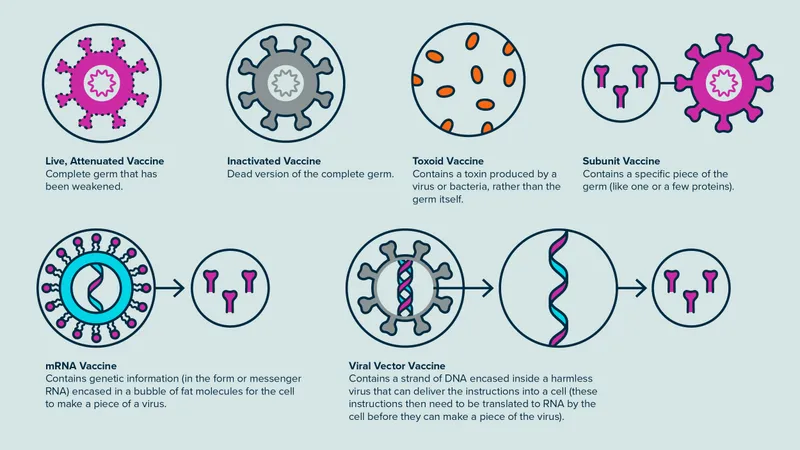
Live vs. Inactivated - A Tale of Two Titers
| Feature | Live Attenuated Vaccines | Inactivated (Killed) Vaccines |
|---|---|---|
| Organism | Weakened virus, can replicate | Killed virus, cannot replicate |
| Immunity | Strong, long-lasting; Humoral & Cellular (CD4+/CD8+) | Weaker, shorter; Mainly Humoral (IgG) |
| Boosters | Generally not required | Multiple boosters needed |
| Safety | ⚠️ Risk of reversion to virulence; Contraindicated in pregnancy & immunodeficiency | Safer, no risk of causing disease |
| IgA Response | Robust secretory IgA response | Poor IgA response |
| Examples | MMR, Varicella, Rotavirus, Sabin polio, Intranasal flu | Hepatitis A, Rabies, Salk polio, Injected flu |
📌 Mnemonic (Live): "RNA Virus Inside Me" (Rotavirus, Varicella, Influenza-intranasal, MMR)
Modern Vax - Subunit & Nucleic Acid
-
Subunit/Recombinant Polysaccharide/Conjugate
- Contain only specific purified macromolecules (e.g., proteins, polysaccharides) of a pathogen.
- Antigens are often produced via recombinant DNA technology.
- Examples: Hepatitis B (HBsAg), HPV (L1 protein), acellular Pertussis, N. meningitidis, S. pneumoniae, H. influenzae type b.
- Safe for immunocompromised patients; require adjuvants and boosters.
-
Nucleic Acid Vaccines
- mRNA Vaccines:
- Formulation: mRNA encoding a viral antigen within a lipid nanoparticle (LNP).
- Mechanism: Host cells translate mRNA → produce viral protein → presented on MHC class I & II.
- Examples: COVID-19 (Pfizer, Moderna).
- Viral Vector Vaccines:
- Mechanism: A modified, non-replicating virus (e.g., adenovirus) delivers DNA encoding the antigen.
- Examples: COVID-19 (J&J, AstraZeneca), Ebola.
- mRNA Vaccines:
⭐ mRNA vaccines are potent because they generate both a strong humoral (B-cell) and cell-mediated (T-cell) immune response, as the host cell synthesizes the antigen endogenously.
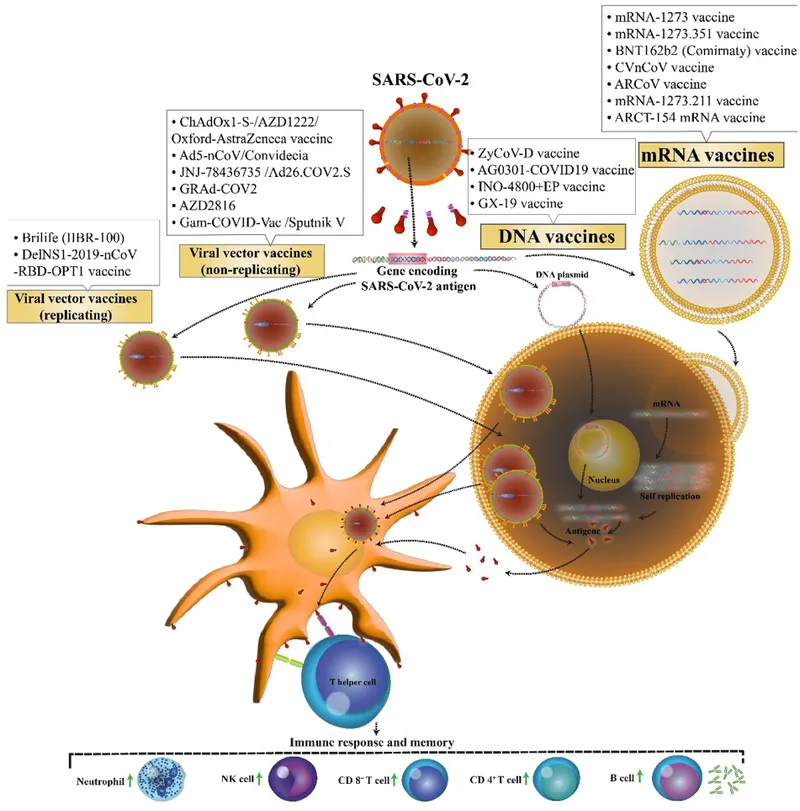
High‑Yield Points - ⚡ Biggest Takeaways
- Live attenuated vaccines (e.g., MMR, Sabin polio) induce potent humoral and cellular immunity but are contraindicated in immunocompromised patients and pregnancy.
- Killed/inactivated vaccines (e.g., Salk polio, Hepatitis A) are safer but less immunogenic, requiring boosters and inducing mainly humoral responses.
- Subunit (HBV, HPV) and mRNA (COVID-19) vaccines are non-infectious, presenting only specific viral antigens or their genetic code.
- The Sabin (live) polio vaccine provides stronger mucosal IgA immunity than the Salk (killed) version.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

