Vaccine Hesitancy - The Hesitation Spectrum
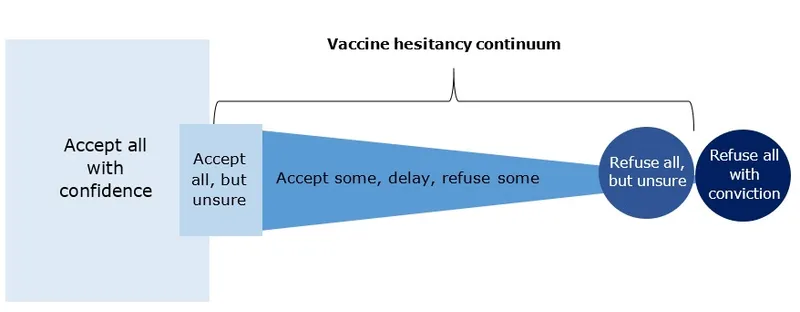
- Vaccine hesitancy exists on a continuum from complete acceptance to outright refusal, influenced by factors of confidence, convenience, and complacency (3 Cs).
- The Spectrum:
- Acceptance: Unquestioning acceptance of all vaccines.
- Hesitation/Caution: Voices concerns, seeks information, may delay or be selective about certain vaccines.
- Refusal: Rejects all vaccines, often termed "anti-vaccine."
⭐ A major historical driver of vaccine hesitancy was a fraudulent 1998 study linking the MMR vaccine to autism. This claim has been definitively debunked by numerous subsequent studies.
Hesitancy Drivers - Why People Pause
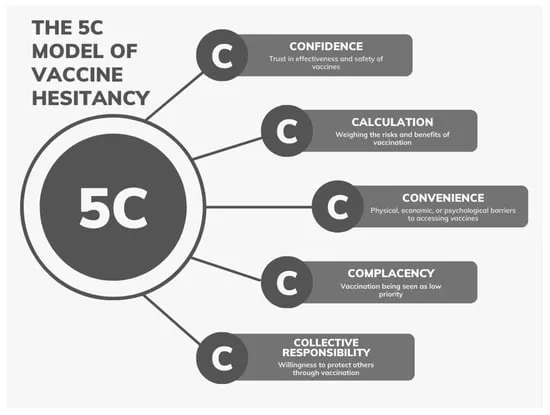
📌 The "5 Cs" Model provides a framework for understanding key drivers.
- Confidence: Lack of trust in vaccine safety, efficacy, or the healthcare system.
- Fears about side effects, long-term effects, and novel technologies (e.g., mRNA).
- Distrust in pharmaceutical companies or government agencies.
- Complacency: Low perceived risk of acquiring a vaccine-preventable disease (VPD).
- Belief that VPDs are not serious or that "natural" immunity is superior.
- Calculation: Individual assessment of risks vs. benefits, often influenced by misinformation.
- Emphasis on personal freedom and autonomy.
⭐ The fraudulent 1998 Lancet paper by Andrew Wakefield linking the MMR vaccine to autism remains a major source of hesitancy, despite being retracted and thoroughly discredited.
Public Health Impact - The Ripple Effect
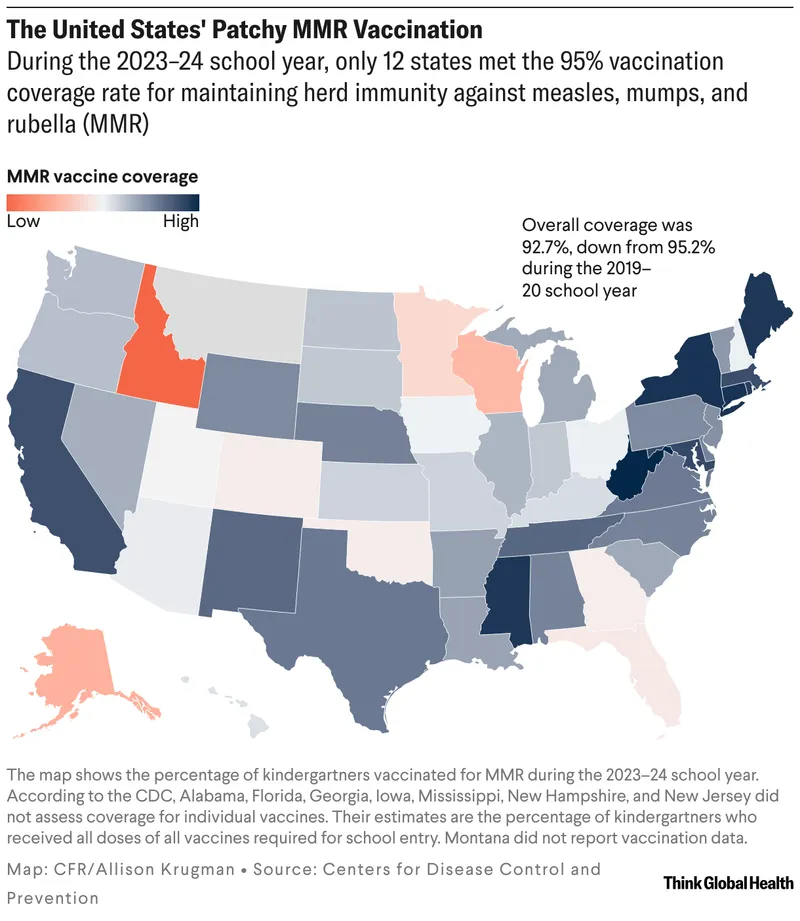
- Resurgence of Vaccine-Preventable Diseases (VPDs):
- Localized outbreaks of measles, mumps, and pertussis are increasingly common in communities with low vaccination rates.
- Erosion of Herd Immunity:
- When vaccination coverage drops below a critical threshold, the collective immunity that protects an entire population is compromised.
- This puts vulnerable individuals at high risk:
- Infants too young to be vaccinated.
- Immunocompromised patients (e.g., chemotherapy, HIV).
- Elderly individuals.
- Economic Burden:
- Significant costs from outbreak investigation, control measures, and treating the sick.
⭐ Measles has an R₀ of 12-18, requiring a herd immunity threshold of ~95% to prevent outbreaks. Even small drops in vaccination rates can lead to rapid community transmission.
Clinician Strategies - Trust & Talk Tactics
- Build Trust: Use empathetic, non-judgmental, patient-centered language. Validate concerns before offering facts.
- Motivational Interviewing (MI): Guide patients to their own conclusions about vaccination benefits. Ask open-ended questions to explore their reasoning.
- Use the C.A.S.E. Method:
- Corroborate: Acknowledge their concerns are valid.
- About Me: Note your role as a trusted expert.
- Science: Briefly explain the data.
- Explain/Advise: Give a clear, strong recommendation.
⭐ A presumptive recommendation (e.g., "Your child is due for vaccines today") is significantly more effective at increasing acceptance than a participatory approach (e.g., "What do you want to do about shots?").
High‑Yield Points - ⚡ Biggest Takeaways
- Vaccine hesitancy, a major public health threat, is driven by misinformation (e.g., debunked MMR-autism link), personal beliefs, and distrust.
- It undermines herd immunity, increasing the risk of outbreaks of diseases like measles and pertussis.
- This disproportionately affects vulnerable populations, including infants and the immunocompromised.
- Effective physician response involves empathetic listening and addressing concerns with evidence-based information.
- Motivational interviewing is a key strategy to build trust and encourage vaccination.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

