Diphtheria - The Strangling Angel
- Organism: Corynebacterium diphtheriae (Gram-positive, club-shaped rod).
- Pathophysiology: Exotoxin encoded by a β-prophage inhibits protein synthesis.
- Clinical Features:
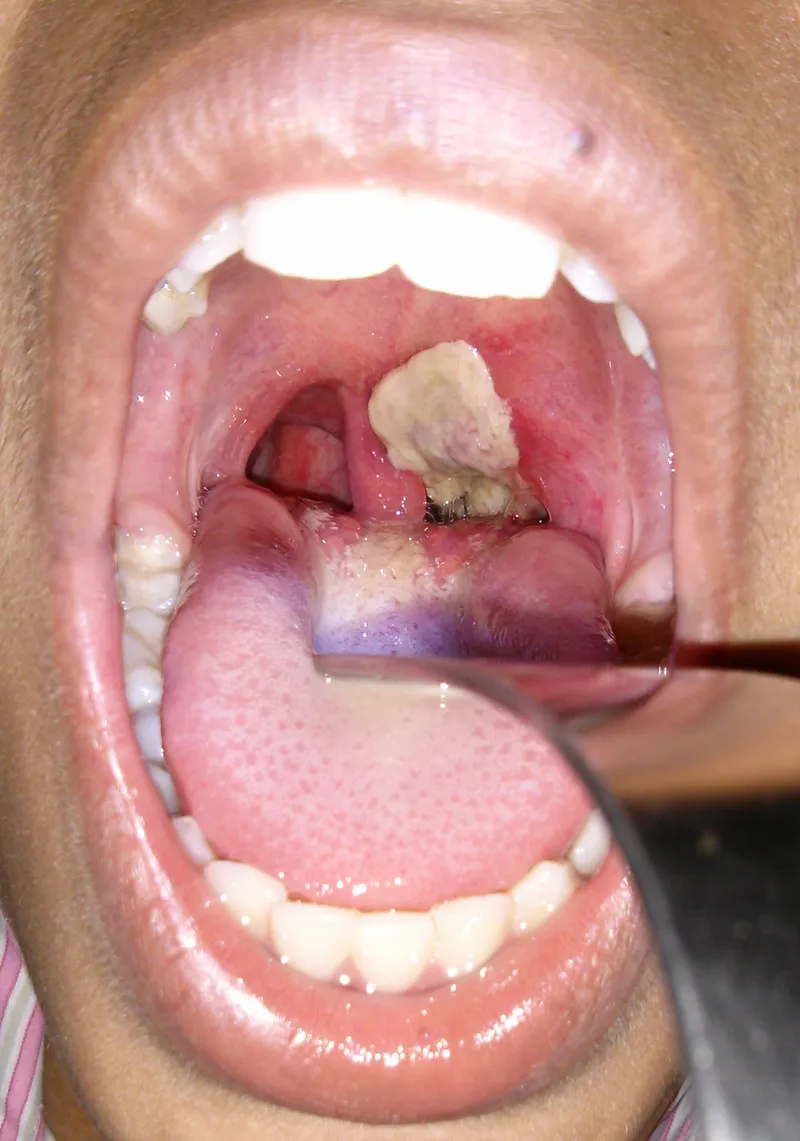
- Local: Sore throat, fever, and a thick, gray, adherent pseudomembrane on the tonsils/pharynx that bleeds when scraped.
- Systemic: "Bull neck" from cervical adenopathy, myocarditis, and neuropathies.
- Diagnosis: Culture on Tellurite or Loeffler's agar; Elek's test for toxin production.
- Treatment: Urgent administration of diphtheria antitoxin plus antibiotics (e.g., erythromycin or penicillin).
⭐ The exotoxin inactivates Elongation Factor-2 (EF-2) via ADP-ribosylation, halting protein synthesis.
Tetanus - The Rigid Smile
- Organism: Clostridium tetani - Gram-positive, spore-forming rod (tennis racket appearance), obligate anaerobe found in soil.
- Toxin: Tetanospasmin, a protease that travels via retrograde axonal transport to the spinal cord.
⭐ Mechanism: Tetanospasmin cleaves synaptobrevin (a SNARE protein), irreversibly blocking the release of inhibitory neurotransmitters (GABA and glycine) from Renshaw cells.
- Clinical: Presents with spastic paralysis.
- Trismus (lockjaw) is a common early sign.
- Risus sardonicus (rigid, grinning smile).
- Opisthotonus (arched back).
Pertussis - The 100-Day Cough
- Organism: Bordetella pertussis, a gram-negative coccobacillus.
- Transmission: Respiratory droplets; highly contagious.
- Clinical Stages:
- Catarrhal (1-2 wks): Nonspecific symptoms, highest infectivity.
- Paroxysmal (2-8 wks): Inspiratory "whoop," post-tussive emesis.
- Convalescent (1-3 mos): Gradual symptom resolution.
- Diagnosis: PCR or culture (nasopharyngeal swab).
- Treatment: Macrolides (e.g., Azithromycin).
⭐ Exam Favorite: Pertussis toxin ADP-ribosylates and inactivates Gi proteins, preventing them from inhibiting adenylate cyclase. The resulting surge in cAMP causes massive lymphocytosis by preventing lymphocyte entry into lymph nodes.
DTPH Vaccines - Acellular Shield
- DTaP (Diphtheria, Tetanus, acellular Pertussis): Primary series for children <7 years.
- Tdap (Tetanus, diphtheria, acellular Pertussis): Booster for adolescents & adults; features lower diphtheria/pertussis antigen dose.
- Administer one dose, then Td booster every 10 years.
- Mechanism: Toxoid-based vaccines that stimulate humoral immunity against bacterial toxins.
⭐ Tdap is recommended during each pregnancy (27-36 weeks) to confer passive immunity to the neonate.

High‑Yield Points - ⚡ Biggest Takeaways
- Diphtheria toxin inactivates Elongation Factor-2 (EF-2) via ADP-ribosylation, halting protein synthesis.
- Tetanus toxin cleaves SNARE proteins, blocking the release of inhibitory neurotransmitters GABA and glycine, causing spastic paralysis.
- Pertussis toxin ADP-ribosylates Gi, leading to increased cAMP levels and the characteristic "whooping cough".
- Key presentations: Diphtheria's pharyngeal pseudomembrane and myocarditis; Tetanus's trismus (lockjaw).
- The DTaP/Tdap vaccine uses toxoids for diphtheria/tetanus and acellular pertussis antigens.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

