Microbiology - The Stealthy Yeast
- Organism: Heavily encapsulated yeast (C. neoformans, C. gattii), found in soil and pigeon droppings.
- Virulence: Antiphagocytic polysaccharide capsule is the major virulence factor.
- Clinical: Primary lung infection can disseminate. Meningoencephalitis is the most common manifestation in immunocompromised patients (HIV, CD4 < 100).
- Diagnosis: India ink stain of CSF reveals halos. Cryptococcal antigen (CrAg) test is highly sensitive and specific.

⭐ Brain imaging may show characteristic gelatinous pseudocysts or "soap bubble" lesions, typically in the basal ganglia.
Pathogenesis - Cloak of Invisibility
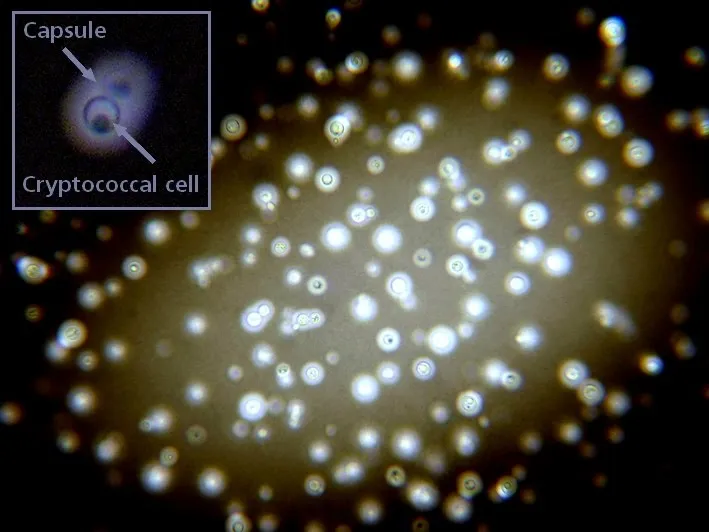
-
Primary Virulence Factor: Polysaccharide Capsule
- Antiphagocytic shield, physically blocking immune cells.
- Masks pathogen-associated molecular patterns (PAMPs) like β-glucan, preventing recognition.
- Sheds capsular antigen (GXM), which acts as a decoy and induces immune tolerance.
-
Other Key Factors:
- Melanin Production: Scavenges free radicals, protecting the yeast from oxidative damage inside phagocytes.
- Urease & Phospholipase: Enzymes that facilitate tissue damage and CNS invasion.
⭐ The massive polysaccharide capsule is not just a physical barrier; its shed antigens (GXM) can be detected in serum and CSF for rapid diagnosis.
Clinical Features - Brain & Lung Invader

- Primary Site: Lungs, often asymptomatic or causing mild pneumonia/nodules.
- Major Manifestation: Meningoencephalitis, the hallmark, especially in immunocompromised (e.g., HIV with CD4 < 100 cells/μL).
- Insidious Onset: Headache, fever, lethargy, confusion.
- ↑ ICP: Key feature causing nausea/vomiting, vision changes, & cranial nerve palsies.
- ⚠️ Meningeal signs (nuchal rigidity) often absent in severe immunosuppression.
- Disseminated Disease: Skin lesions resembling molluscum contagiosum are common.
⭐ In HIV patients, cryptococcal meningitis is the most common cause of meningitis.
Diagnosis - Unmasking the Fungus
- Lumbar Puncture (LP): Essential for suspected CNS disease.
- Often shows markedly ↑ opening pressure (>20 cm H₂O).
- CSF: ↑ protein, ↓ glucose, pleocytosis with lymphocytic predominance.
- Microscopy & Stains:
- India Ink Stain: Reveals encapsulated, budding yeast with characteristic halos.
- Mucicarmine or GMS stains are positive on tissue samples.
- Antigen & Culture:
- Cryptococcal Antigen (CrAg) Test: Rapid, highly sensitive/specific test on CSF & serum.
- Culture: Gold standard. Use Sabouraud agar.
⭐ The CrAg latex agglutination test is the most crucial diagnostic tool, detecting polysaccharide capsule antigens. It can be positive weeks before symptoms manifest.

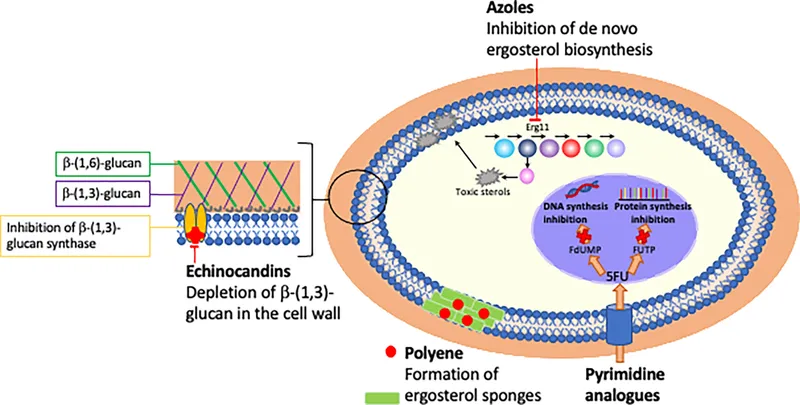
Treatment - Fungal Fatality Fighters
📌 Amphotericin + Flucytosine to Attack, Fluconazole for Follow-up.
Treatment varies by disease severity and immune status. For severe CNS or disseminated disease:
⭐ For meningitis, aggressive management of ↑ Intracranial Pressure (ICP) via serial lumbar punctures is as critical as antifungal therapy for preventing mortality and blindness.
High‑Yield Points - ⚡ Biggest Takeaways
- Encapsulated yeast found in pigeon droppings (C. neoformans) or eucalyptus trees (C. gattii).
- Major virulence factor is its thick polysaccharide capsule, visualized as halos on India ink stain.
- Causes meningoencephalitis in immunocompromised patients, particularly AIDS with CD4 < 100.
- Pulmonary cryptococcosis can present as pneumonia or asymptomatic nodules.
- Diagnosis via Cryptococcal antigen (CrAg) test in serum or CSF is rapid and sensitive.
- Treatment involves Amphotericin B + flucytosine, followed by long-term fluconazole.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

