Hepatitis C Virus - The Stealthy Instigator
- Virus: Enveloped, (+)ssRNA Flavivirus; high genetic variability due to error-prone RNA polymerase.
- Pathogenesis: Chronic inflammation and direct viral protein actions are the key drivers.
- Inflammation: Persistent immune response → cycles of necrosis & regeneration → fibrosis → cirrhosis.
- Viral Proteins: Core, NS3, and NS5A interfere with tumor suppressors like p53 and Rb.
- 📌 C for Chronic, Cirrhosis, Carcinoma.
⭐ Unlike Hepatitis B, the HCV genome does not integrate into the host genome; oncogenesis is driven by chronic inflammation and viral protein interference.
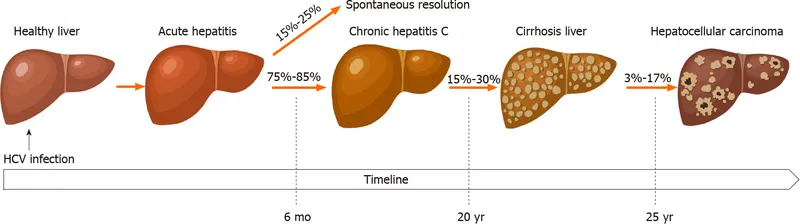
Pathogenesis - From Hepatitis to Hepatoma
- Inflammation-Driven Carcinogenesis: Unlike DNA viruses, HCV (an RNA virus) does not integrate into the host genome. The primary driver is chronic inflammation and subsequent hepatocyte turnover.
- Cycle of Damage & Repair: Persistent infection leads to a vicious cycle:
- Chronic hepatitis → hepatocyte necrosis → compensatory regeneration.
- This high-turnover state, amidst oxidative stress, fosters mutations.
- Leads to progressive liver fibrosis and, ultimately, cirrhosis in most cases.
- Key Viral Proteins: HCV Core, NS3, and NS5A proteins interfere with host pathways, inhibiting tumor suppressors like p53 and promoting cell proliferation.
⭐ High-Yield: While cirrhosis is the strongest risk factor, HCV can induce HCC without it. Viral proteins (e.g., NS5A) can directly activate pro-oncogenic pathways like Wnt/β-catenin, promoting carcinogenesis even in a non-cirrhotic liver.
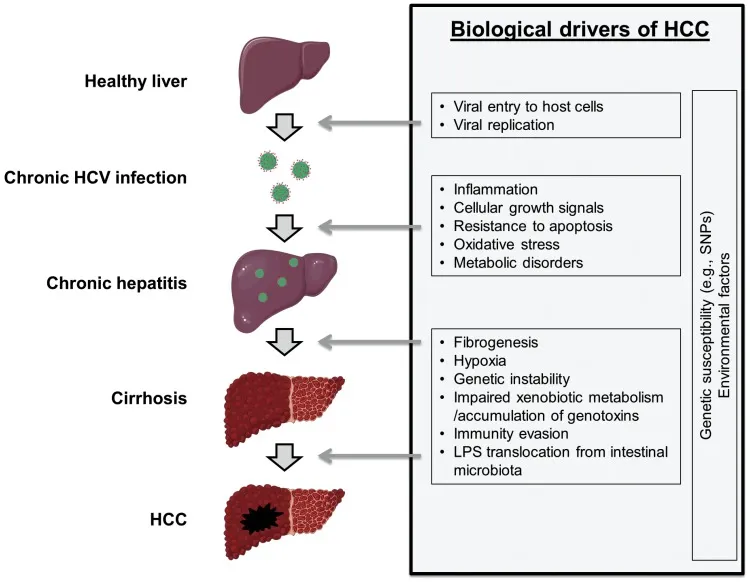
Clinical & Diagnosis - Unmasking the Culprit
-
Clinical Course:
- Acute infection is often asymptomatic; chronic infection is a "silent" disease for decades.
- Progresses insidiously to fatigue, nausea, and eventually signs of cirrhosis (jaundice, ascites, encephalopathy).
-
Diagnostic Workup:
- Screening: Immunoassay for anti-HCV antibodies. A positive result indicates exposure, not necessarily active infection.
- Confirmation: HCV RNA testing (PCR) to confirm active viremia.
- Staging: Liver biopsy or non-invasive elastography to assess fibrosis/cirrhosis.
-
HCC Surveillance:
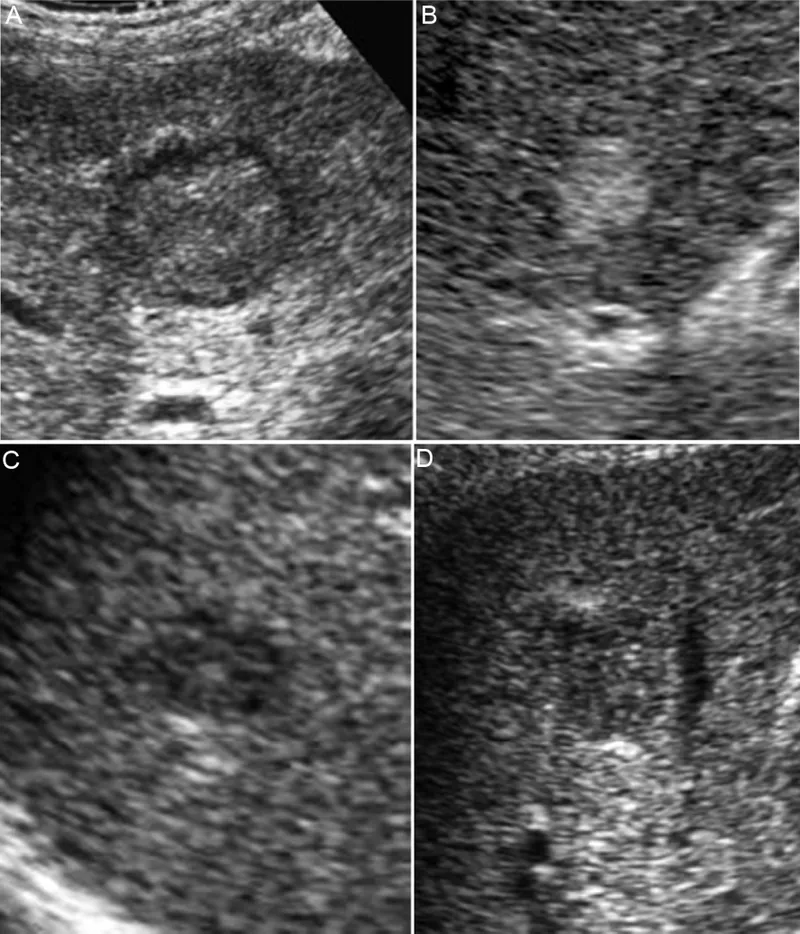
- For all cirrhotic patients: abdominal ultrasound ± AFP every 6 months.
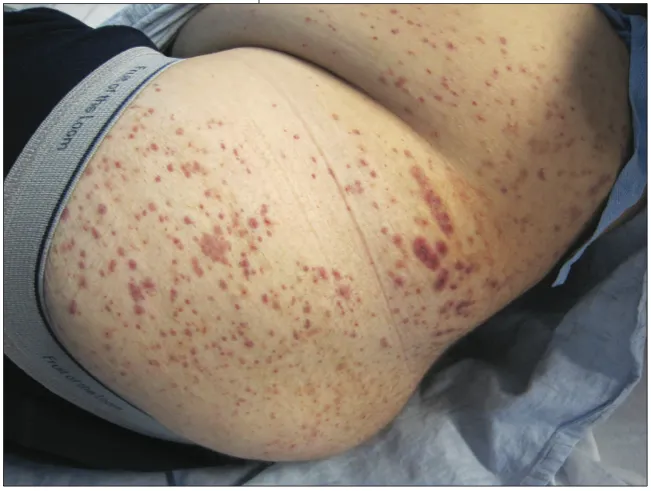
⭐ Mixed cryoglobulinemia is a classic extrahepatic manifestation, presenting with palpable purpura, weakness, and arthralgias (Meltzer's triad).
Screening & Management - The Vigilant Response
- Universal Screening: All adults aged 18-79 once. Test for anti-HCV antibodies; confirm active infection with HCV RNA PCR.
- HCC Surveillance: For patients with cirrhosis, ultrasound (US) with or without alpha-fetoprotein (AFP) every 6 months.
- Management Goal: Achieve Sustained Virologic Response (SVR) with Direct-Acting Antivirals (DAAs).
- Regimens like Sofosbuvir/Ledipasvir offer >95% cure rates.
- HCC Treatment: Staged approach.
- Early: Resection, transplant, local ablation.
- Advanced: Systemic therapy (e.g., Sorafenib).
⭐ Achieving SVR with DAAs significantly reduces, but does not eliminate, the risk of developing HCC, especially in patients with pre-existing cirrhosis. Surveillance must continue.
High‑Yield Points - ⚡ Biggest Takeaways
- Hepatitis C (HCV) is a major cause of hepatocellular carcinoma (HCC), typically developing over 20-30 years.
- The primary mechanism is chronic inflammation and liver cirrhosis, not direct viral oncogene action.
- Viral proteins like the HCV core protein and NS5A/NS5B disrupt host cell cycle control and apoptosis.
- Unlike HBV, HCV is an RNA virus and does not integrate into the host genome.
- Regular ultrasound screening for HCC is crucial for patients with HCV-induced cirrhosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

