VAP Defined - The Unwanted Guest
- Ventilator-Associated Pneumonia (VAP): A subtype of hospital-acquired pneumonia (HAP) developing in a patient on mechanical ventilation.
- Key Criterion: Pneumonia that arises >48 hours after endotracheal intubation and the start of mechanical ventilation.
- Mechanism: Caused by microaspiration of colonized secretions from the oropharynx or upper GI tract around the endotracheal tube cuff.
⭐ The 48-hour rule is a critical diagnostic cutoff to distinguish VAP from community-acquired or other aspiration pneumonias present at admission.
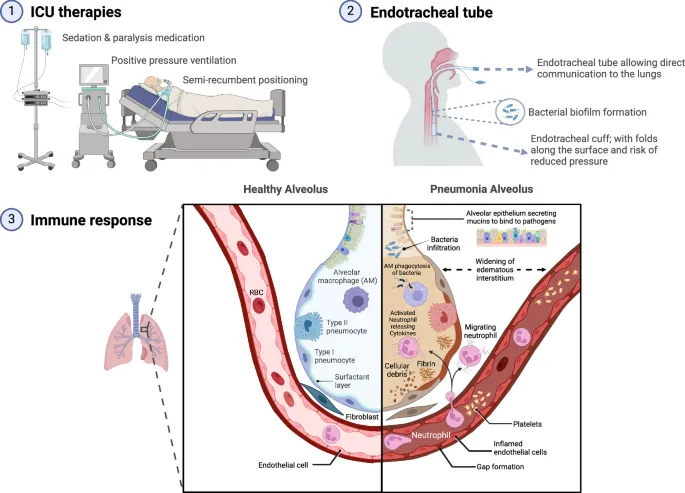
Etiology & Pathogenesis - The Usual Suspects
Ventilator-associated pneumonia (VAP) is a lung infection developing >48 hours after endotracheal intubation.
-
Primary Mechanism: Microaspiration of contaminated secretions from the oropharynx or stomach around the endotracheal tube cuff. This bypasses host defenses, leading to bacterial colonization and infection of the lower airways.
-
Common Pathogens:
- Early-onset (<5 days): Often antibiotic-sensitive organisms.
- Streptococcus pneumoniae
- Haemophilus influenzae
- Methicillin-sensitive Staphylococcus aureus (MSSA)
- Late-onset (≥5 days): Frequently multidrug-resistant (MDR) pathogens.
- Pseudomonas aeruginosa
- Methicillin-resistant S. aureus (MRSA)
- Acinetobacter species
- Early-onset (<5 days): Often antibiotic-sensitive organisms.
⭐ Pseudomonas aeruginosa is the most common causative agent of VAP, particularly in late-onset cases, and is notorious for biofilm formation on endotracheal tubes, contributing to antibiotic resistance and treatment failure.
Diagnosis & Workup - Catching the Culprit
- Primary Mechanism: Microaspiration of colonized oropharyngeal or gastric bacteria around the endotracheal tube (ETT) cuff, gaining direct access to the lower airways.
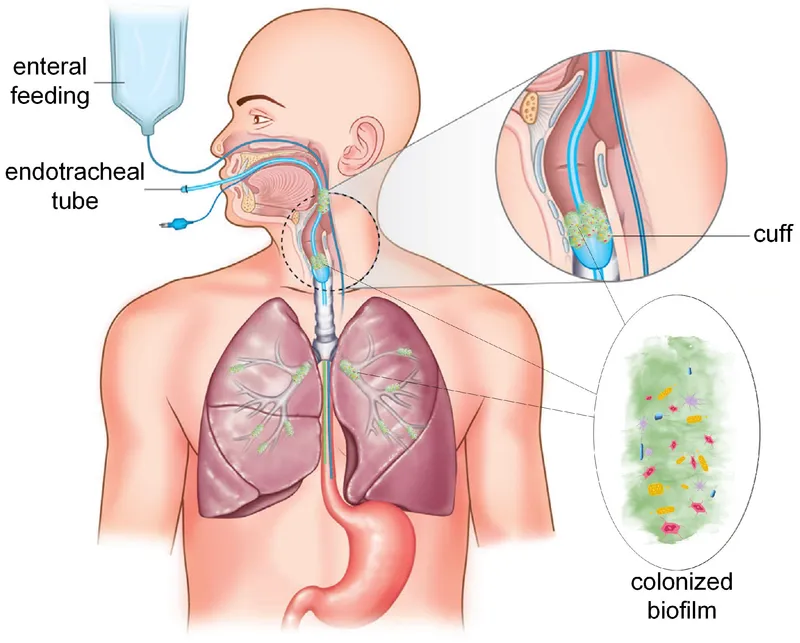
- Diagnostic Criteria: Suspect in any ventilated patient with signs of infection.
- Radiographic: New, persistent, or progressive infiltrate on chest X-ray.
- Clinical (≥2 required):
- Fever >38°C or hypothermia <36°C
- Leukocytosis (>12,000) or leukopenia (<4,000)
- New onset of purulent sputum.
⭐ The Clinical Pulmonary Infection Score (CPIS) can aid diagnosis, but lower respiratory tract sampling (e.g., endotracheal aspirate, BAL) with quantitative cultures is key to confirm the pathogen and guide targeted antibiotic therapy.
- Common Culprits:
| Onset | Typical Pathogens |
|---|---|
| Early-Onset (<5 days) | Antibiotic-sensitive bacteria: S. pneumoniae, H. influenzae, MSSA. |
| Late-Onset (≥5 days) | Multidrug-resistant (MDR) organisms: Pseudomonas, Acinetobacter, MRSA, ESBL-producers. |
Management & Prevention - The VAP Vanquishers

- Diagnosis: A combination of clinical, radiological, and microbiological findings.
- Clinical Pulmonary Infection Score (CPIS): Can guide suspicion; low specificity.
- Definitive Diagnosis: Quantitative cultures from lower respiratory tract samples.
- Endotracheal Aspirate: >10^5-10^6 CFU/mL
- Bronchoalveolar Lavage (BAL): >10^4 CFU/mL
- Protected Specimen Brush (PSB): >10^3 CFU/mL
⭐ Empiric, broad-spectrum antibiotic therapy should be started promptly, covering Pseudomonas and MRSA, tailored to local antibiograms. De-escalate therapy once culture results are available.
- 📌 VAP Prevention Bundle:
- Elevate head of bed to 30-45°.
- Daily "sedation vacations" & readiness-to-extubate assessments.
- Oral hygiene with chlorhexidine.
- Subglottic secretion drainage.
High-Yield Points - ⚡ Biggest Takeaways
-
VAP Bundle for prevention is key:
- Head of bed elevation 30-45°
- Daily sedation vacations
- Prophylaxis for peptic ulcer disease (PUD) & DVT
- Oral care with chlorhexidine
-
Empiric Antibiotics depend on MDR risk factors (e.g., prior IV antibiotic use).
| Risk Category | Empiric Therapy |
|---|---|
| Low Risk | Ceftriaxone or Piperacillin-tazobactam |
| High Risk (MDR) | Anti-pseudomonal β-lactam + Anti-MRSA agent |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

