SSI Basics - The Unwanted Souvenir
- Infection occurring at or near a surgical incision within 30 days of the procedure, or within 90 days if prosthetic material is implanted.
- Top Pathogens: Staphylococcus aureus (most common), coagulase-negative staphylococci, Enterococcus spp., and E. coli.
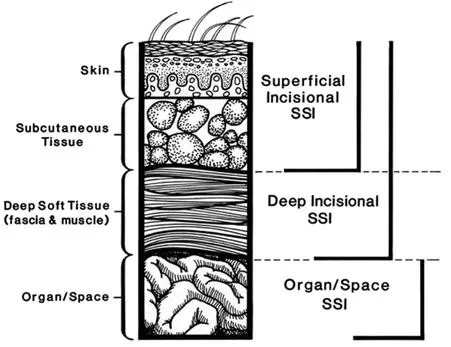
- Classification by Depth:
- Superficial Incisional (skin, subcutaneous tissue)
- Deep Incisional (fascia, muscle)
- Organ/Space
⭐ Most SSIs become clinically apparent between postoperative day 5 and 10.
Causative Organisms - The Usual Suspects
- Staphylococcus aureus: The most frequent cause (~30%), typically originating from the patient's skin or nasal flora.
- Other Gram-Positives:
- Coagulase-negative staphylococci (e.g., S. epidermidis), common in procedures involving prosthetic implants.
- Enterococcus spp., often seen after abdominal or pelvic surgeries.
- Gram-Negatives:
- Escherichia coli, Klebsiella spp., and Enterobacter spp. are common after GI/GU surgeries.
- Pseudomonas aeruginosa.
- Anaerobes:
- Bacteroides fragilis is a key pathogen in colorectal surgery.
⭐ In clean surgeries (e.g., cardiac, neuro), skin flora like S. aureus and S. epidermidis are the predominant pathogens. In contrast, contaminated surgeries (e.g., bowel resection) have a higher incidence of polymicrobial infections with Gram-negative rods and anaerobes.
Risk & Prevention - Dodging the Infection
-
Patient Risk Factors:
- Smoking, obesity (BMI > 30), malnutrition
- Comorbidities: Diabetes (HbA1c > 7%)
- Nasal carriage of S. aureus
-
Procedural Risk Factors:
- Emergency surgery, prolonged duration
- Contaminated wound class
- Improper skin prep, intra-op hypothermia
-
Core Prevention Steps:
- Pre-op: Antiseptic shower, glucose control <180 mg/dL
- Intra-op: Hair clipping (no razors), chlorhexidine prep, maintain normothermia
⭐ Most SSIs are caused by Staphylococcus aureus, originating from the patient's own skin flora. This makes pre-operative screening and decolonization a key preventive strategy in high-risk surgeries like cardiac or orthopedic procedures.
Diagnosis & Management - The Aftermath Plan
-
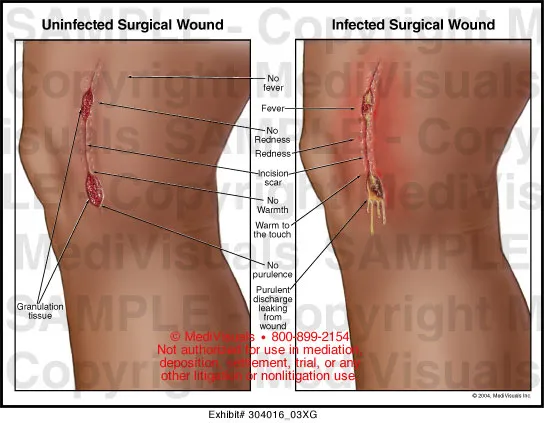
Diagnosis: Primarily clinical (erythema, pain, purulent drainage).
- Obtain deep wound cultures before starting antibiotics.
- Imaging (CT/ultrasound) to detect deeper collections/abscesses.
-
Management:
- Source Control: Open the wound, explore, debride necrotic tissue, and drain purulent material. Leave wound open to heal by secondary intention.
- Antibiotics: Empiric therapy targeting common pathogens (S. aureus, streptococci), then tailor based on culture results.
⭐ Most SSIs manifest 5-7 days post-op. Early onset (<48 hrs) suggests Group A Strep or Clostridium perfringens.
High‑Yield Points - ⚡ Biggest Takeaways
- S. aureus is the most common cause of SSIs; consider MRSA.
- SSIs typically appear within 30 days of surgery, or up to 1 year with prosthetic material.
- Prophylaxis with Cefazolin (1st-gen cephalosporin) is standard, given <60 minutes before incision.
- Colorectal surgery requires anaerobic coverage (e.g., cefoxitin, metronidazole).
- Major risk factors include diabetes, obesity, smoking, and prolonged surgery.
- Diagnosis is clinical: erythema, warmth, pain, and purulent drainage.
- Treatment involves incision and drainage plus systemic antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

