Pathophysiology - The Gut Wrecker
- Causative Agent: Gram-positive, spore-forming, obligate anaerobic rod.
- Transmission: Fecal-oral route. Spores are highly resilient, resisting heat, acid, and alcohol-based sanitizers.
- Mechanism of Injury:
- Toxin A (Enterotoxin): Targets the brush border, causing inflammation, fluid secretion, and watery diarrhea.
- Toxin B (Cytotoxin): More potent; causes actin depolymerization, leading to mucosal cell apoptosis and necrosis.
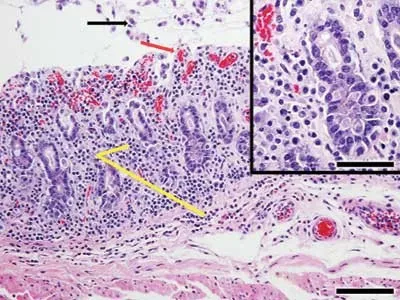
⭐ The toxins' destruction of the colonic epithelium leads to the formation of characteristic pseudomembranes-yellow-white plaques composed of fibrin, mucus, and inflammatory cells.
Risk & Presentation - Antibiotic's Revenge
-
Risk Factors:
- Recent antibiotic use (📌 Clindamycin, Fluoroquinolones, Cephalosporins)
- Advanced age (>65 years)
- Recent hospitalization or long-term care residency
- Proton Pump Inhibitor (PPI) use
-
Classic Presentation:
- Profuse, watery, foul-smelling diarrhea (>3 loose stools in 24h)
- Lower abdominal pain & cramping
- Low-grade fever, leukocytosis
-
Severe Disease Hallmark:
- Pseudomembranous colitis (yellowish-white plaques on colonoscopy)
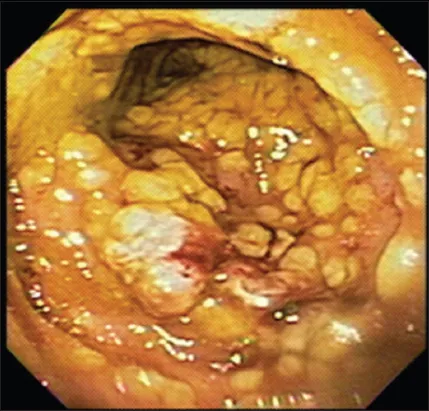
⭐ While Clindamycin is classically cited, third-generation cephalosporins are a very common cause of hospital-acquired C. difficile.
Diagnosis - The Toxin Trackdown
- Best Initial Test: Stool testing. Options include:
- Nucleic Acid Amplification Test (NAAT) for C. diff toxin genes.
- Glutamate Dehydrogenase (GDH) antigen + toxin EIA combo.
- Severity Markers: Suggest severe disease.
- WBC > 15,000 cells/mL
- Creatinine ≥ 1.5x baseline
- Imaging: Abdominal X-ray or CT for complications like toxic megacolon (colonic diameter > 6 cm).
⭐ NAAT is highly sensitive but doesn't distinguish between active infection and colonization. A positive toxin EIA confirms active toxin production, indicating true disease.
Management - The Flora Force
- Primary Goal: Discontinue the inciting antibiotic as soon as possible.
- Prevention: Strict contact precautions (gown, gloves).
⭐ Alcohol-based hand sanitizers do NOT kill C. difficile spores; vigorous hand washing with soap and water is required to physically remove them.
High‑Yield Points - ⚡ Biggest Takeaways
- C. difficile is a Gram-positive, spore-forming anaerobe transmitted via spores, often following antibiotic use.
- Key risk factors include clindamycin, fluoroquinolones, cephalosporins, and proton pump inhibitors.
- Pathogenesis is mediated by Toxin A (enterotoxin) and Toxin B (cytotoxin), causing diarrhea and colonic damage.
- Clinical presentation ranges from mild diarrhea to life-threatening pseudomembranous colitis and toxic megacolon.
- Diagnosis relies on stool NAAT/PCR for toxin genes.
- First-line treatment is oral fidaxomicin or oral vancomycin.
- High recurrence rates are managed with fidaxomicin or a vancomycin taper.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

