EPS Composition - The Biofilm's Glue
- Major Components: A hydrated matrix (~97% water) primarily composed of:
- Polysaccharides: The main structural scaffold. Key examples include Alginate (Pseudomonas aeruginosa), Cellulose (E. coli, Salmonella), and Glucans (Streptococcus mutans).
- Proteins: Functional (e.g., enzymes like hydrolases, nucleases) and structural (e.g., amyloid fibers like curli, fimbriae).
- eDNA (extracellular DNA): Released via cell lysis; critical for initial adhesion, structural stability, and horizontal gene transfer.
- Lipids & Surfactants: Contribute to biofilm structure and facilitate motility.
⭐ Alginate, an exopolysaccharide from Pseudomonas aeruginosa in Cystic Fibrosis patients, is a key virulence factor that confers significant antibiotic resistance.
EPS Functions - Slime Shield Activated
- Structural Scaffold: Provides the 3D architecture for the biofilm community.
- Adhesion & Cohesion: Mediates initial attachment to surfaces (e.g., catheters, teeth) and cements bacteria together.
- Protective Barrier:
- Shields from host immunity (phagocytes, antibodies, complement).
- Limits penetration of antimicrobial agents, often ↑ MIC by 100-1000x.
- Prevents desiccation by retaining water.
- Nutrient Reservoir: Sequesters ions and can be degraded for use as a carbon source during starvation.
- Genetic Exchange Hub: Creates a stable environment facilitating horizontal gene transfer.
⭐ High-Yield: The EPS matrix is a primary reason for the profound antibiotic resistance of biofilms. It acts as a diffusion barrier, slowing drug penetration and allowing bacteria time to activate stress responses.
📌 Mnemonic: "SHIELD"
- Structural support
- Hydration
- Immune evasion
- Environment for exchange
- Location (adhesion)
- Diet (nutrients)
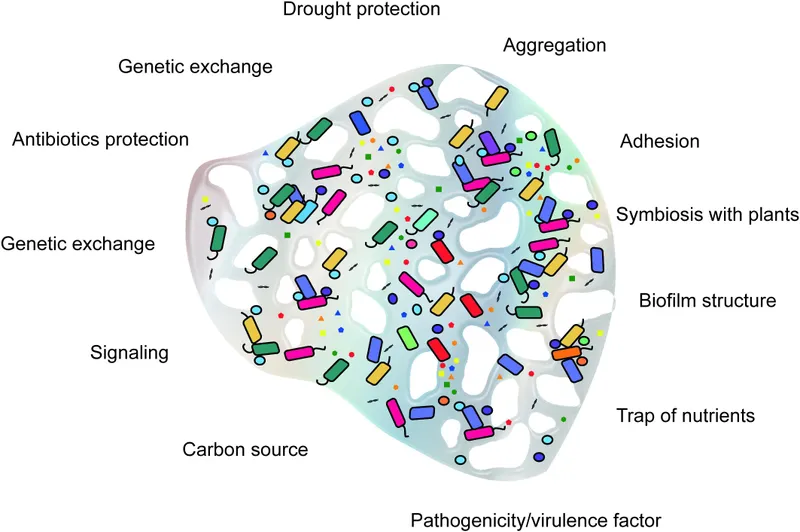 matrix protecting bacteria from antibiotics and immune cells)
matrix protecting bacteria from antibiotics and immune cells)
Clinical Relevance - Resistance & Virulence
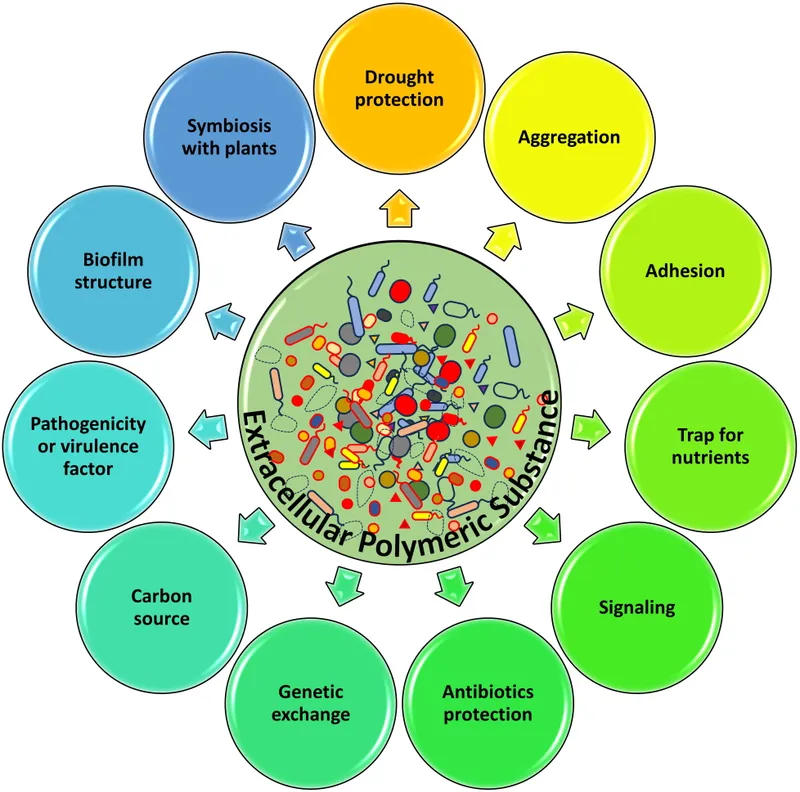
-
Antibiotic Resistance: Biofilms create a formidable barrier against antimicrobial agents.
- Physical Barrier: The dense EPS matrix physically blocks or slows the diffusion of antibiotics.
- Chemical Inactivation: Enzymes trapped within the EPS (e.g., β-lactamases) can degrade antibiotics like penicillin.
- Altered Metabolism: Bacteria in deeper layers are often in a slow-growing or dormant state (persister cells), making them less susceptible to antibiotics that target active cell processes.
-
Host Immune Evasion:
- The EPS matrix shields bacteria from phagocytosis and antibodies.
- Contributes to chronic infections by frustrating immune clearance (e.g., Pseudomonas aeruginosa in cystic fibrosis).
⭐ Biofilm-associated bacteria can be up to 1000-fold more resistant to antibiotics than their free-floating (planktonic) counterparts.
High‑Yield Points - ⚡ Biggest Takeaways
- The Extracellular Polymeric Substance (EPS) is the structural "slime" matrix of biofilms, providing protection and adhesion.
- It's a complex mixture of polysaccharides, proteins, lipids, and extracellular DNA (eDNA).
- EPS is critical for adhesion to surfaces, especially medical devices like catheters and implants.
- It acts as a physical barrier, shielding microbes from antibiotics and host immune responses.
- eDNA in the matrix facilitates horizontal gene transfer, promoting the spread of resistance.
- Directly contributes to the persistence and chronic nature of biofilm-associated infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

