Biofilm Formation - The Slime Shield
- Foundation: Begins with planktonic (free-floating) bacteria attaching to a surface (e.g., catheters, implants).
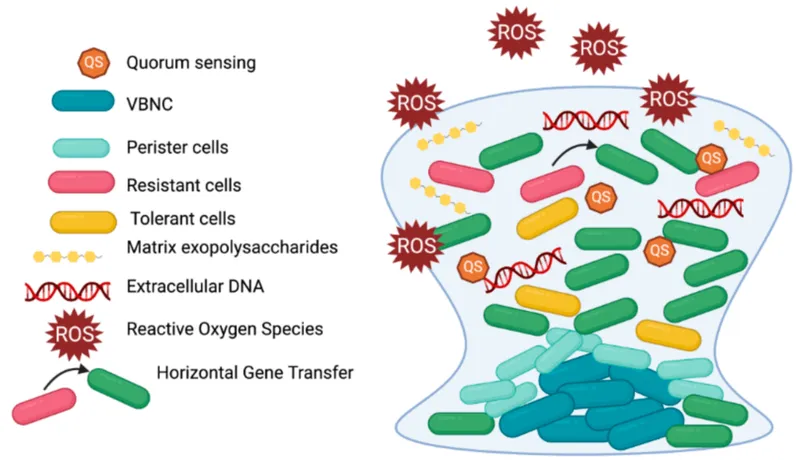
- The Matrix: Bacteria secrete Extracellular Polymeric Substance (EPS), a slimy mix of polysaccharides, proteins, lipids, and eDNA.
- This EPS encases the colony, providing structural support and protection.
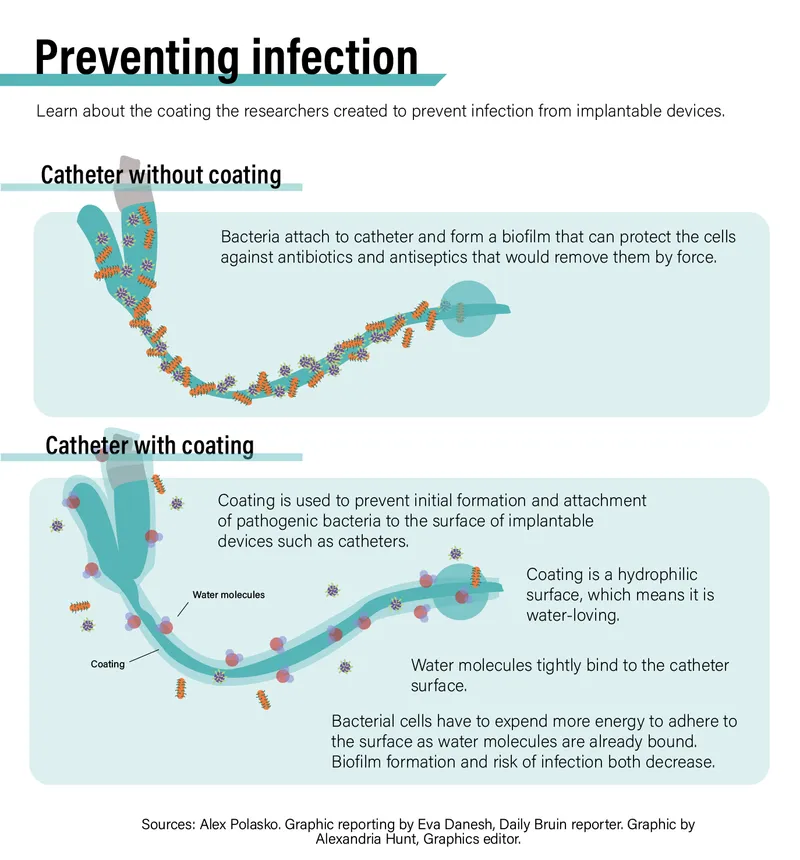
⭐ Quorum Sensing: Bacteria communicate via autoinducers (e.g., acyl-homoserine lactones in Gram-negatives) to coordinate gene expression, initiating EPS production once a critical population density is reached.
Resistance Mechanisms - Fort Biofilm's Defenses
-
Physical Barrier: Extracellular Polymeric Substance (EPS) matrix physically blocks or slows antibiotic penetration.
- Certain antibiotics may be inactivated by binding to EPS components.
-
Altered Microenvironment: Creation of chemical gradients within the biofilm.
- ↓ O₂ and nutrient availability leads to slow-growing or dormant cells in deeper layers.
- These metabolically inactive cells are less susceptible to antibiotics targeting active processes (e.g., β-lactams).
-
Persister Cells: A subpopulation of dormant, highly tolerant cells that survive antibiotic assault and can repopulate the biofilm post-treatment.
-
Efflux Pumps & Enzyme-Mediated Resistance: Overexpression of efflux pumps to expel antibiotics from the cell.
- Concentrated neutralizing enzymes (e.g., β-lactamases) are trapped within the EPS matrix, protecting the entire community.
⭐ Horizontal Gene Transfer (HGT): High cell density promotes the exchange of genetic material, such as plasmids and transposons carrying resistance genes, accelerating the spread of resistance.
Clinical Correlates - High-Risk Havens
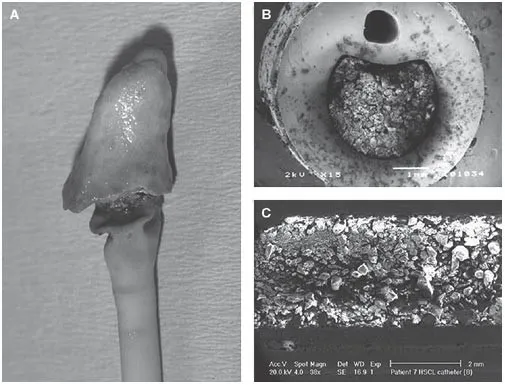
- Prosthetic Devices: Hotbeds for biofilm formation.
- Joints & Heart Valves: Staphylococcus epidermidis & S. aureus are primary culprits. Viridans streptococci on native/prosthetic valves.
- Catheters (Venous/Urinary): S. epidermidis, S. aureus, Candida, E. coli, Proteus.
- Chronic Infections:
- Cystic Fibrosis Pneumonia: Mucoid Pseudomonas aeruginosa creates stubborn lung biofilms.
- Dental Plaque & Caries: Streptococcus mutans.
- Chronic Otitis Media: Non-typeable Haemophilus influenzae.
- Prostatitis: E. coli.
⭐ Exam Favorite: The mucoid phenotype of Pseudomonas aeruginosa in cystic fibrosis is due to alginate overproduction, a key component of its protective biofilm matrix, leading to persistent infections and antibiotic failure.
High‑Yield Points - ⚡ Biggest Takeaways
- The extracellular polymeric substance (EPS) matrix is a physical barrier that blocks or slows antibiotic penetration.
- Slow bacterial growth within the biofilm reduces the efficacy of antibiotics targeting active cell division, like β-lactams.
- An altered chemical microenvironment (e.g., ↓O₂, ↓pH) can directly inactivate certain antimicrobial drugs.
- Biofilms harbor persister cells, dormant variants that survive high-dose antibiotic therapy and can repopulate the community.
- Close proximity facilitates horizontal gene transfer, accelerating the spread of resistance genes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

