Overview - The Wall-less Wonder
- Smallest free-living bacteria; famously lacks a peptidoglycan cell wall, rendering beta-lactam antibiotics ineffective.
- Consequently pleomorphic (variable shape).
- Cell membrane uniquely contains sterols (cholesterol), acquired from the host, for structural integrity.
- Known as an "atypical" pathogen because it doesn't gram stain and has a milder presentation.
- Transmitted via respiratory droplets, with a long incubation period.
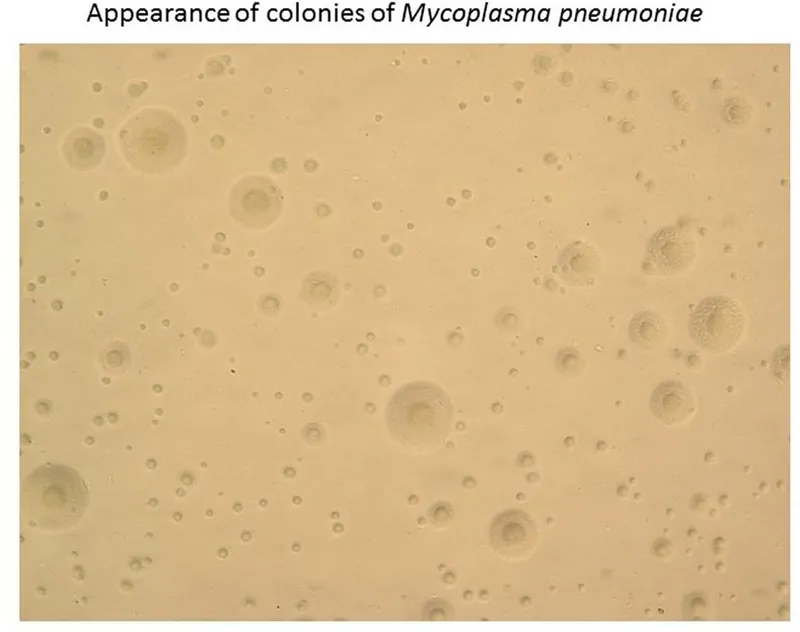
⭐ A primary cause of community-acquired atypical pneumonia ("walking pneumonia"), particularly in school-aged children, military recruits, and college students.
Pathophysiology - The Great Adherer
- Extracellular pathogen attaching to respiratory epithelium via the P1 adhesin protein.
- This binding to sialic acid receptors causes ciliostasis, inhibiting mucous clearance.
- Secretes CARDS (Community-Acquired Respiratory Distress Syndrome) toxin, an ADP-ribosylating toxin that damages host cells and incites inflammation.
⭐ The P1 adhesin is located on a specialized tip structure, allowing M. pneumoniae to glide along and bind tightly to respiratory mucosa, which is key to its pathogenesis.
Clinical Features - The Walking Pneumonia
- Insidious Onset: Low-grade fever, malaise, and a persistent, hacking, non-productive cough.
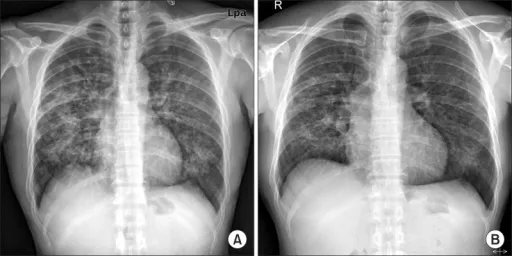
- Auscultation: Often unremarkable, despite significant X-ray findings (wheezes, rhonchi).
- "Walking Pneumonia": Patients often remain ambulatory and appear less ill than their chest X-ray suggests.
- Extrapulmonary Manifestations: Common and high-yield.
- Dermatologic: Erythema multiforme (target lesions), Stevens-Johnson syndrome (SJS).
- Hematologic: Cold agglutinin (IgM) disease → autoimmune hemolytic anemia.
- ENT: Bullous myringitis (painful vesicles on the tympanic membrane).
⭐ High-Yield: Mycoplasma can trigger cold agglutination. IgM antibodies bind to I antigen on RBCs in colder temperatures, leading to complement-mediated hemolysis and anemia.
Diagnosis - The Cold Agglutinin
- Mechanism:
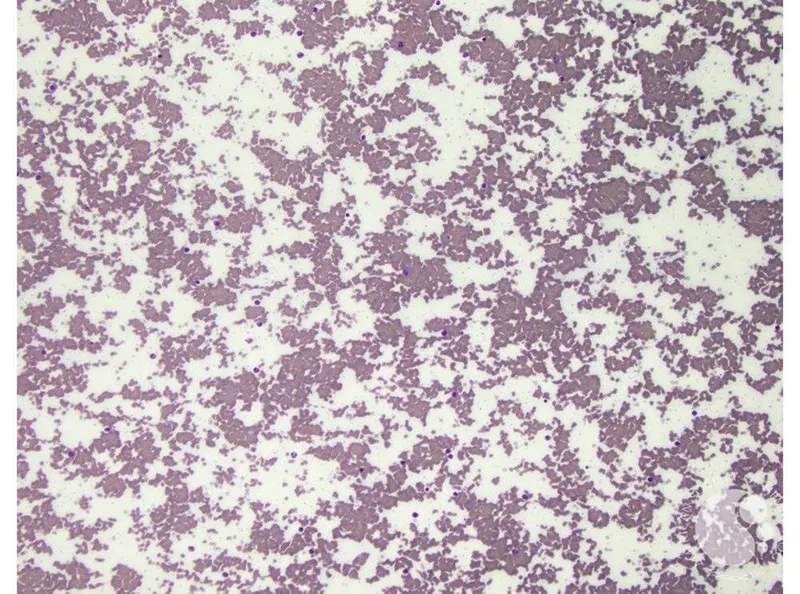
- Mycoplasma induces autoantibodies (IgM) that bind to the I antigen on RBCs.
- These "cold agglutinins" cause RBC clumping at cooler temperatures (<37°C), potentially leading to mild, self-limited extravascular hemolysis.
- Testing:
- Cold agglutinin test shows a titer ≥ 1:32.
- Found in ~50% of cases, peaking 2-4 weeks after infection.
- 📌 Mycoplasma Causes Cold agglutinins.
⭐ High-Yield: The test is non-specific. Cold agglutinins can also be seen in infectious mononucleosis (EBV), influenza, and certain lymphomas.
Treatment - No Wall, No Problem
- Primary Agents: Target protein synthesis or DNA replication, bypassing the need to attack a cell wall.
- Macrolides: Azithromycin, clarithromycin. Often first-line, especially in children.
- Tetracyclines: Doxycycline. Effective, but avoided in children <8 years.
- Fluoroquinolones: Levofloxacin. Reserved for adults or resistant cases.
- Ineffective: All β-lactam antibiotics (e.g., penicillins, cephalosporins).
⭐ Macrolide resistance is a growing concern, particularly in Asia, often requiring a switch to tetracyclines or fluoroquinolones.
- Lacks a cell wall, making it resistant to penicillins and other beta-lactam antibiotics.
- The classic cause of atypical or "walking" pneumonia, particularly in adolescents and military recruits.
- Unique among prokaryotes for requiring cholesterol for its cell membrane integrity.
- Strongly associated with cold agglutinins (IgM), which can lead to autoimmune hemolytic anemia.
- Common extrapulmonary manifestations include rashes (like erythema multiforme/SJS) and neurologic issues.
- Macrolides or tetracyclines are the treatments of choice.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

