M. tuberculosis - The Great White Plague
- Characteristics: Acid-fast bacillus (Ziehl-Neelsen stain), obligate aerobe, facultative intracellular in macrophages.
- Virulence Factors: Mycolic acid (waxy lipid cell wall), Cord factor (serpentine growth, inhibits neutrophil migration).
- Culture: Slow-growing on Lowenstein-Jensen (LJ) medium.
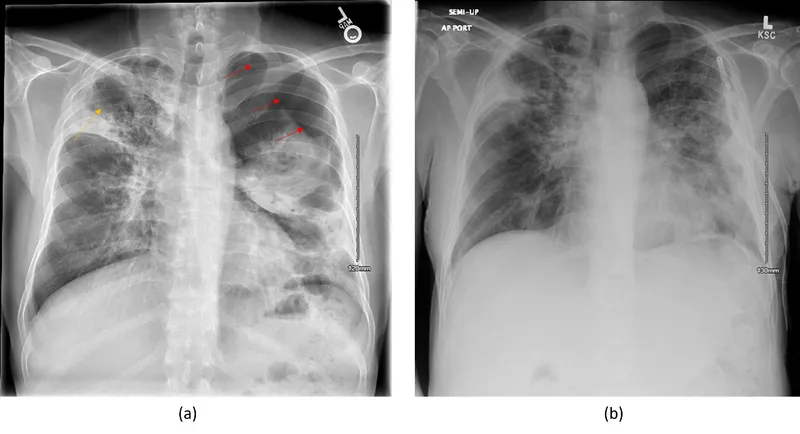
- Pathogenesis:
- Diagnosis:
- PPD/TST Induration: >5 mm (immunocompromised, close contacts), >10 mm (high-risk), >15 mm (no risk factors).
- IGRAs: QuantiFERON-TB Gold, T-SPOT.TB.
- AFB smear, culture (gold standard), NAAT.
⭐ M. tuberculosis is an obligate aerobe, explaining its predilection for the well-ventilated lung apices during reactivation.
Non-Tuberculous Mycobacteria - The Atypical Cousins
| Organism | Source/Transmission | Classic Presentation | Buzzwords |
|---|---|---|---|
| M. avium complex (MAC) | Ubiquitous (water, soil) | Disseminated disease in AIDS (CD4 < 50); prophylaxis with azithromycin. Pulmonary disease in COPD. | - |
| M. kansasii | Tap water | TB-like pulmonary disease, often in patients with underlying lung conditions. | - |
| M. scrofulaceum | Environmental sources | Scrofula: painless cervical lymphadenitis, typically seen in children. | - |
| M. marinum | Aquariums, saltwater | Papule on hand/arm that ulcerates and spreads along lymphatics after minor trauma. | 'Fish tank granuloma' |
| M. leprae (Hansen's Dis.) | Armadillos, resp. droplets | Spectrum: Tuberculoid (strong Th1, few lesions) to Lepromatous (weak Th2, many lesions). | 'Leonine facies' |
⭐ Mycobacterium avium complex (MAC) is the most common NTM causing human disease, typically presenting as a disseminated infection in severely immunocompromised patients (CD4 < 50).
Anti-Mycobacterial Drugs - RIPE for Action
| Drug | Mechanism of Action | Key Adverse Effect(s) |
|---|---|---|
| Rifampin | Inhibits DNA-dependent RNA polymerase | Red-orange body fluids |
| Isoniazid (INH) | Inhibits mycolic acid synthesis | Hepatotoxicity, peripheral neuropathy |
| Pyrazinamide | Active in acidic pH of phagolysosomes | Hyperuricemia, gout |
| Ethambutol | Inhibits arabinosyltransferase (cell wall) | Optic neuropathy (red-green color blindness) |
⭐ Co-administration of pyridoxine (Vitamin B6) with Isoniazid is standard practice to prevent peripheral neuropathy.
High‑Yield Points - ⚡ Biggest Takeaways
- M. tuberculosis is an acid-fast bacillus requiring an aerobic environment, explaining its predilection for lung apices.
- Primary infection is marked by a Ghon complex; reactivation leads to caseating granulomas with central necrosis.
- Diagnosis relies on acid-fast staining, culture on Löwenstein-Jensen medium, and interferon-gamma release assays (IGRAs).
- Standard treatment is multi-drug RIPE therapy (Rifampin, Isoniazid, Pyrazinamide, Ethambutol).
- M. avium complex (MAC) causes disseminated disease in AIDS patients (CD4 < 50); prophylaxis with azithromycin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

