Initial Assessment - The First 10 Minutes
- ABCs & Vitals: Immediate stabilization, focused history, and physical exam.
- Initial Setup: IV access (2 large-bore), cardiac monitor, pulse oximetry.
- Oxygen: Only if O₂ saturation < 90% or in respiratory distress.
- Medications (Concurrent):
- Aspirin: 325 mg (chewed) immediately.
- Nitroglycerin (sublingual): For active pain. ⚠️ Caution with hypotension, bradycardia, or recent PDE-5 inhibitor use.
- Morphine: For pain refractory to nitroglycerin.
⭐ A 12-lead ECG must be obtained and interpreted within 10 minutes of arrival. If initial ECG is non-diagnostic but suspicion is high, consider posterior leads (V7-V9).
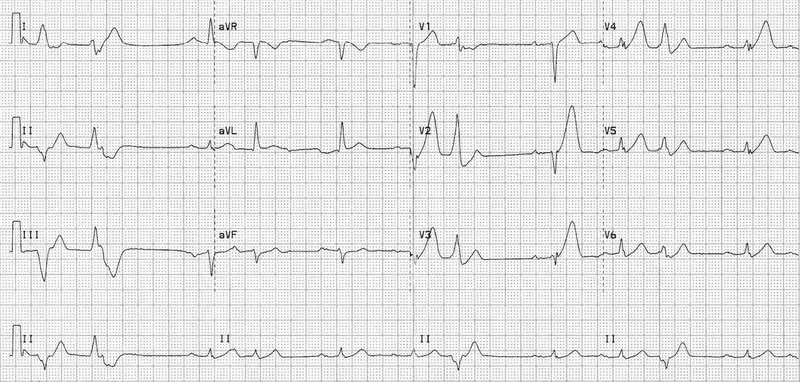
ECG Interpretation - Reading the Lines
- Primary Goal: Identify ST-elevation MI (STEMI) for emergent reperfusion.
- STEMI Criteria: New ST elevation at the J-point in ≥2 contiguous leads.
- ≥1 mm in most leads.
- In leads V2-V3: ≥2 mm in men ≥40y, ≥2.5 mm in men <40y, or ≥1.5 mm in women.
- NSTEMI/Ischemia: New horizontal or downsloping ST depression ≥0.5 mm or T-wave inversion ≥1 mm.
- Pathologic Q-waves: Indicate prior MI; >0.04s wide & >25% of R-wave height.
⭐ A new or presumed new Left Bundle Branch Block (LBBB) in a patient with ischemic chest pain is considered a STEMI equivalent.
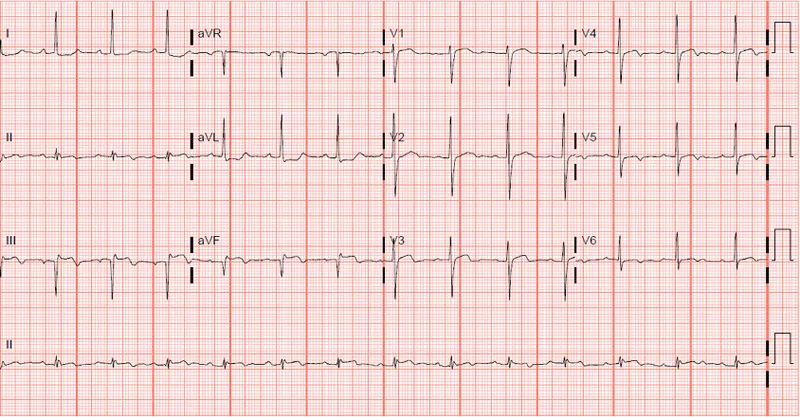
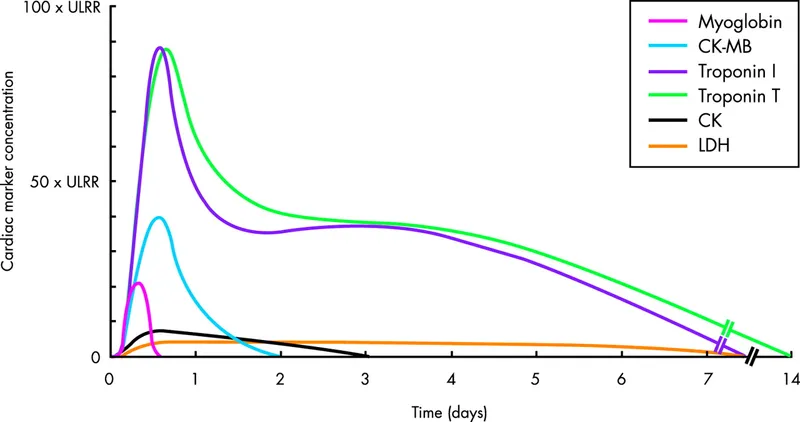
Cardiac Biomarkers - Chemical Footprints
- Troponins (cTnI, cTnT): The gold standard for MI diagnosis due to high sensitivity and specificity.
- Rise: 2-4 hrs
- Peak: 24-48 hrs
- Duration: 7-10 days
- 📌 Troponin lasts up to Ten days.
- Creatine Kinase-MB (CK-MB):
- Rise: 4-6 hrs
- Peak: 12-24 hrs
- Baseline: 48-72 hrs
- Useful for detecting reinfarction.
⭐ High-sensitivity troponin (hs-cTn) can rule out MI faster (e.g., in a 0/1-hour algorithm).
Immediate Triage - The MONA-BASH Protocol
📌 MONA-BASH is a classic mnemonic, though treatment order varies. Aspirin first!
- Aspirin: 162-325 mg chewed immediately to inhibit platelet aggregation. Reduces mortality.
- Oxygen: Supplemental O₂ only if saturation is <90% or in respiratory distress.
- Nitroglycerin: Sublingual/IV. Vasodilator; reduces preload and pain.
- Contraindicated in hypotension (SBP <90 mmHg), recent PDE-5 inhibitor use, or right ventricular infarction.
- Morphine: IV for refractory chest pain despite nitrates. Also reduces preload.
- Beta-Blockers: e.g., Metoprolol. Reduces O₂ demand and arrhythmias. Start within 24h if no signs of heart failure/shock.
- ACE Inhibitors: Start within 24h, especially in patients with anterior MI, heart failure, or EF <40%.
- Statin: High-intensity (e.g., Atorvastatin 80 mg) initiated ASAP, regardless of baseline cholesterol.
- Heparin (UFH or LMWH): Anticoagulation to prevent further thrombus formation.
⭐ Beta-blockers are one of the few initial therapies (along with Aspirin and reperfusion) that have a proven mortality benefit in acute MI.
- Initial management includes ABCs, IV access, cardiac monitoring, and a 12-lead ECG within 10 minutes.
- Administer chewable aspirin (162-325 mg) immediately to all patients without contraindications.
- Supplemental O₂ is only for hypoxemia (SaO₂ <90%) or respiratory distress.
- Nitroglycerin for chest pain is contraindicated in right ventricular infarction, severe aortic stenosis, or recent PDE-5 inhibitor use.
- Morphine is a second-line analgesic for pain refractory to nitrates.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

