Arrhythmia Overview - The Heart's Glitches
- Timing is key: Risk is highest in the first 48 hours post-MI.
- Acute Phase (< 48 hrs): Due to ischemia, electrolyte shifts, and reperfusion injury.
- Late Phase (> 48 hrs): Arises from scar tissue formation and ventricular remodeling, creating re-entrant circuits.
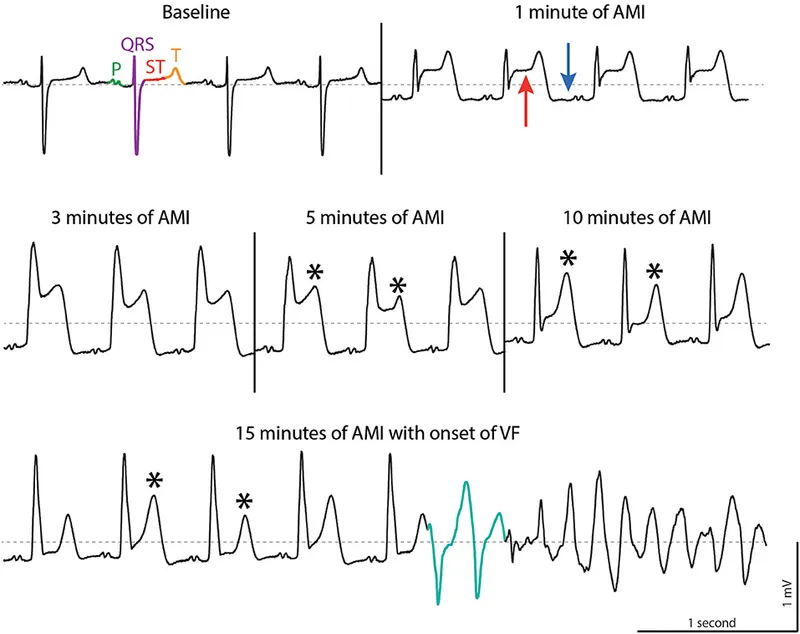
⭐ Ventricular fibrillation (V-fib) is the most common cause of sudden cardiac death in the immediate hours following an acute MI.
Bradyarrhythmias & AV Blocks - The Slowdown
- Sinus Bradycardia: Rate < 60 bpm. Often benign (athletes) or drug-induced (β-blockers, CCBs).
- AV Blocks: Delay or interruption of atrial impulse to ventricles.
- 1st Degree: Fixed, prolonged PR interval (> 0.20s).
- 2nd Degree, Mobitz I (Wenckebach): Progressively lengthening PR until a beat is dropped. 📌 "Longer, longer, longer, DROP!"
- 2nd Degree, Mobitz II: Constant PR interval with randomly dropped beats. High risk of progressing to 3rd degree.
- 3rd Degree (Complete): Complete dissociation of P waves and QRS complexes. Requires urgent pacing.
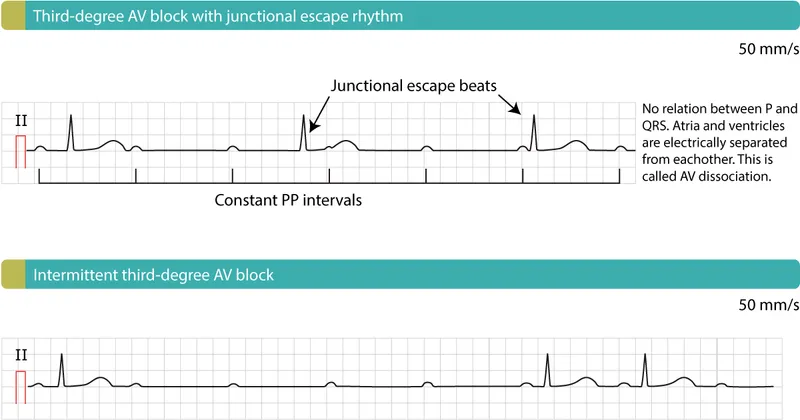
⭐ In inferior MIs, AV blocks (especially 1st-degree and Mobitz I) are common due to RCA ischemia affecting the AV node. These often resolve with reperfusion.
Ventricular Arrhythmias - Dangerously Fast Beats
- Core Principle: Assess for a pulse and hemodynamic stability to guide management. Wide QRS complex tachycardia is treated as VT until proven otherwise.
- Types & ECG:
- Ventricular Tachycardia (VT): Organized, wide QRS (>0.12s). Can be monomorphic or polymorphic.
- Ventricular Fibrillation (VF): Disorganized, chaotic rhythm with no identifiable QRS. No cardiac output.
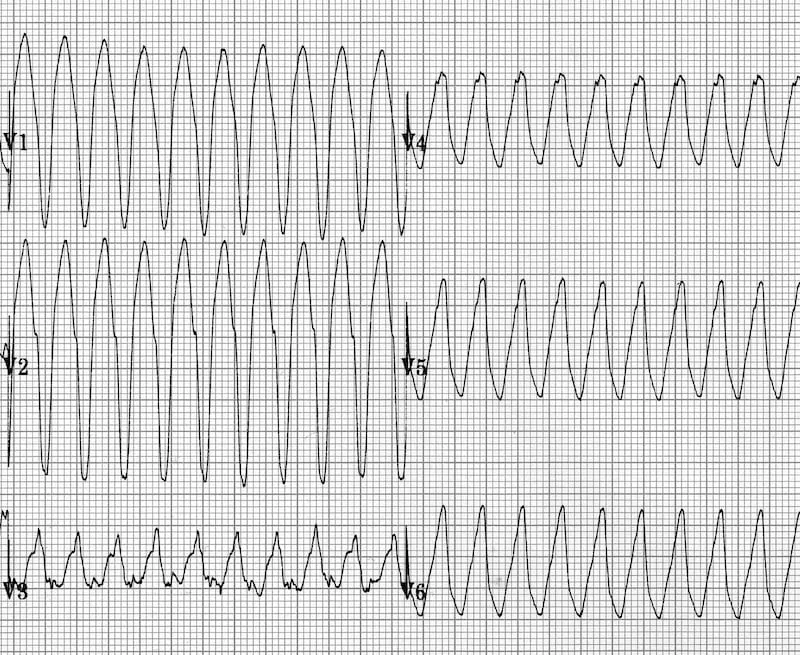
⭐ For Torsades de Pointes (polymorphic VT with a long QT interval), the first-line treatment is IV Magnesium Sulfate, not standard VT antiarrhythmics.
Atrial Fibrillation - Irregularly Irregular
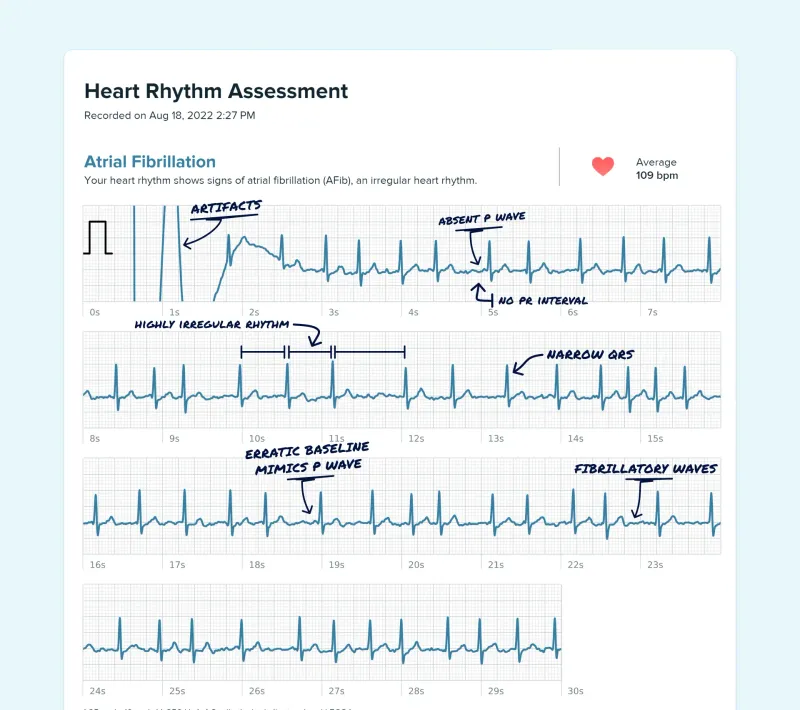
- Hallmark: Irregularly irregular rhythm with absent P waves & variable ventricular rate.
- Acute Management (Unstable): Immediate synchronized cardioversion.
- Stable Management: Focus on rate control & anticoagulation.
- Rate Control: β-blockers (metoprolol) or non-DHP CCBs (diltiazem). Goal HR < 110 bpm.
- Anticoagulation: Guided by CHA₂DS₂-VASc score for stroke prevention.
- Score ≥ 2 (men) or ≥ 3 (women) → DOACs (e.g., apixaban) > warfarin.
⭐ The CHA₂DS₂-VASc score, not the presence of symptoms, dictates the need for chronic anticoagulation to prevent ischemic stroke.
High‑Yield Points - ⚡ Biggest Takeaways
- Sinus bradycardia is treated with atropine only if it causes hypotension or altered mental status.
- Atrial fibrillation requires rate control (beta-blockers) and risk-stratified anticoagulation.
- Ventricular fibrillation and pulseless VT are shockable rhythms requiring immediate defibrillation.
- For stable VT, use antiarrhythmics like amiodarone; for unstable VT with a pulse, use synchronized cardioversion.
- High-degree AV blocks (Mobitz II, third-degree) demand transcutaneous pacing, likely followed by a permanent pacemaker.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

