Sodium Disorders - Salty Situations
-
Hyponatremia (<135 mEq/L): Check serum osmolality (Osm).
- Hypotonic (<280 mOsm): True hyponatremia. Assess volume status.
Volume Status Urine Na+ Causes Hypovolemic >20 Renal loss (diuretics) <10 Extra-renal loss (GI, skin) Euvolemic >20 SIADH, Hypothyroidism, Adrenal Insuff. Hypervolemic >20 CHF, Cirrhosis, Nephrotic Syndrome - Isotonic (280-295): Pseudohyponatremia (↑lipids/protein).
- Hypertonic (>295): Hyperglycemia, mannitol. $Na_{corr} = Na_{meas} + 2.4 \times \frac{Glucose-100}{100}$.
- Hypotonic (<280 mOsm): True hyponatremia. Assess volume status.
-
Hypernatremia (>145 mEq/L): Always hypertonic; net water loss.
- Causes: Dehydration, Diabetes Insipidus (Central vs. Nephrogenic).
-
⚠️ Correction Rate is Key
- Hyponatremia: Correct slowly to prevent Osmotic Demyelination Syndrome (ODS). Rate <8-10 mEq/L/24h.
- Hypernatremia: Correct slowly to prevent cerebral edema.
⭐ Central Pontine Myelinolysis (a type of ODS) from rapid correction of chronic hyponatremia presents with spastic quadriparesis, pseudobulbar palsy, and altered consciousness.

Potassium Disorders - K's Kardiac Karma
-
Hypokalemia (<3.5 mEq/L):
- Causes: Diuretics (loop/thiazide), RTA, GI loss (diarrhea, vomiting), hyperaldosteronism.
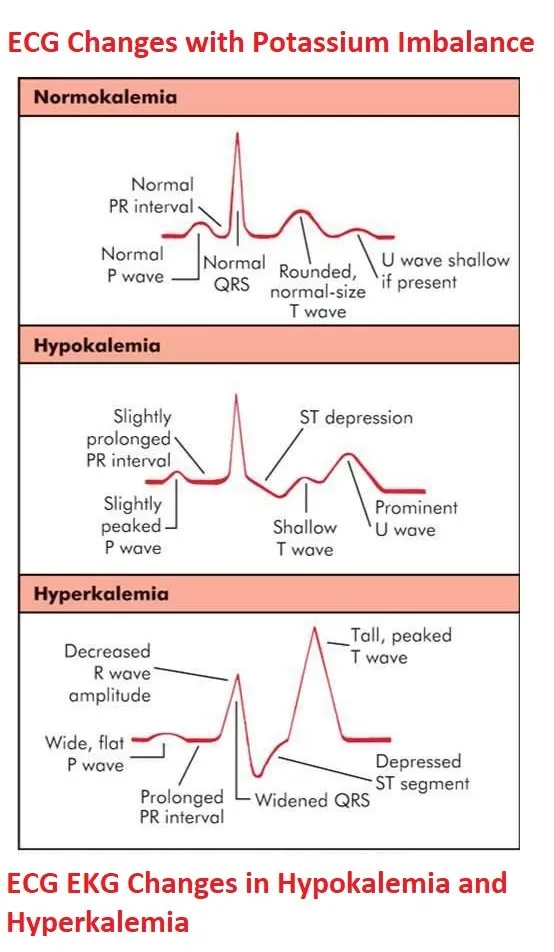
- ECG: Flattened T waves, prominent U waves, ST depression.
- Tx: Oral/IV KCl. Max IV rate: 10-20 mEq/hr. Always check & correct ↓Mg²⁺ first!
-
Hyperkalemia (>5.5 mEq/L):
- Causes: CKD, ACEi/ARBs, K⁺-sparing diuretics, crush injury/rhabdo, adrenal insufficiency.
- ECG: Peaked T waves, wide QRS, sine wave pattern → V-fib.
- 📌 Mnemonic (Tx): C BIG K Drop (Calcium, Bicarb/Beta-agonist, Insulin, Glucose, Kayexalate, Diuretics/Dialysis).
⭐ In hyperkalemia with ECG changes, give IV Calcium Gluconate first to stabilize the cardiac membrane before lowering potassium.
Calcium Disorders - A Bone to Pick
-
Hypercalcemia (>10.5 mg/dL)
- Causes: Primary Hyperparathyroidism (outpatient), Malignancy (inpatient), Thiazides.
- Symptoms: "Stones, bones, groans, psychiatric overtones."
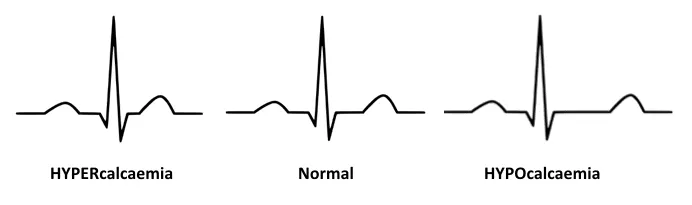
- EKG: Short QT interval.
- Tx: Aggressive IV fluids, calcitonin (rapid), bisphosphonates (slow onset, long duration).
-
Hypocalcemia (<8.5 mg/dL)
- Causes: Hypoparathyroidism (e.g., post-thyroidectomy), CKD, Vitamin D deficiency.
- Symptoms: Perioral numbness, tetany, seizures.
- Signs: 📌 Chvostek (facial tap), Trousseau (carpal spasm).
- EKG: Long QT interval.
- Tx: IV Calcium Gluconate.
⭐ Malignancy is the most common cause of hypercalcemia in hospitalized patients, often via PTHrP (e.g., Squamous Cell Lung Cancer).
Magnesium & Phosphate - The Understudies
- Hypomagnesemia (< 1.8 mg/dL)
- Causes: Diuretics (loops/thiazides), PPIs, diarrhea, alcohol abuse.
- Effects: Torsades de Pointes, tetany, prolonged PR/QT intervals.
- Hypophosphatemia (< 2.5 mg/dL)
- Causes: Refeeding syndrome, DKA, chronic antacid use.
- Effects: Acute muscle weakness (incl. diaphragm), rhabdomyolysis, cardiac dysfunction.

⭐ Refractory Hypokalemia? Always check magnesium levels. Hypomagnesemia prevents renal K⁺ reabsorption and intracellular correction.
High-Yield Points - ⚡ Biggest Takeaways
- Hyperkalemia with EKG changes (peaked T waves) requires immediate IV calcium gluconate for cardiac stabilization.
- Correcting chronic hyponatremia too quickly risks osmotic demyelination syndrome; correcting hypernatremia too quickly risks cerebral edema.
- Hypocalcemia presents with neuromuscular excitability (Chvostek/Trousseau signs) and QT prolongation.
- Severe hypercalcemia management starts with aggressive IV fluid hydration to enhance renal excretion.
- Refractory hypokalemia often indicates underlying hypomagnesemia; always replete magnesium first.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

