Initial Rx - Stabilize First!
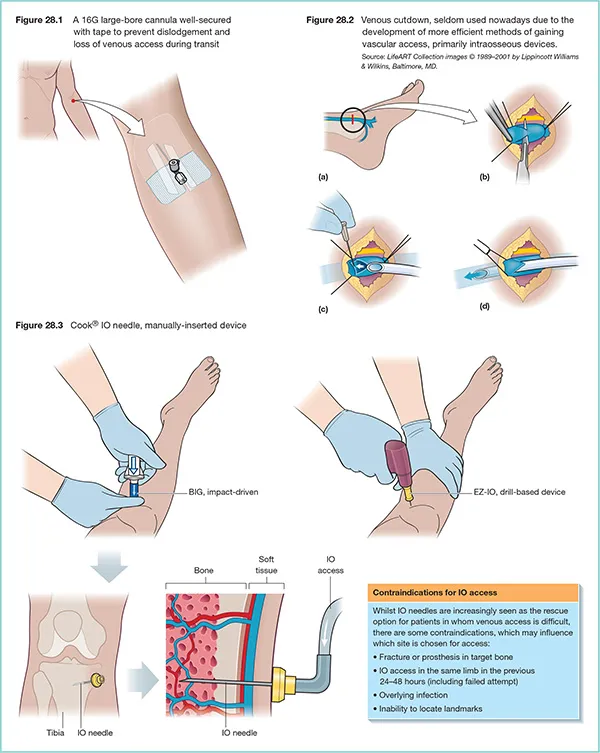
- ABCs: Assess & secure Airway, Breathing, Circulation. Intubate for altered mental status or hematemesis.
- IV Access: Place 2 large-bore (≥18G) peripheral IV catheters for rapid infusion.
- Resuscitation: Begin aggressive IV fluid resuscitation with crystalloids (NS or LR).
- Transfusion Trigger: Transfuse packed RBCs (pRBCs) for Hemoglobin <7 g/dL.
- Key Labs: Type & crossmatch, CBC, coagulation studies (PT/INR, PTT), LFTs, BUN/Cr.
- Medication: Start a high-dose IV Proton Pump Inhibitor (PPI) drip (e.g., pantoprazole).
⭐ In patients with known Coronary Artery Disease (CAD), the transfusion threshold is higher; maintain Hb >9 g/dL to ensure adequate myocardial oxygen delivery.
Localize the Bleed - Up or Down?
-
Upper GI Bleed (UGIB): Proximal to Ligament of Treitz.
- Presentation: Hematemesis (vomiting blood/coffee grounds), melena (black, tarry stool).
- Key Lab: ↑ BUN/Cr ratio > 20.
-
Lower GI Bleed (LGIB): Distal to Ligament of Treitz.
- Presentation: Hematochezia (bright red blood per rectum).
- Melena can indicate a slow-bleed, right-sided LGIB.
⭐ A BUN/Cr ratio > 20 strongly suggests an upper GI source. This is due to the digestion of blood proteins in the upper gut, leading to increased urea absorption.
Upper GI Bleed - Variceal vs. Ulcer
-
Initial Steps (All UGIB): Assess ABCs. Secure 2 large-bore IVs. Transfuse if Hb <7 g/dL (or <9 in CAD). Start high-dose IV PPI. Consult GI for urgent endoscopy (<24h).
-
Variceal Bleed (from Portal HTN):
- Acute Rx: Octreotide (reduces splanchnic flow), prophylactic ceftriaxone, and endoscopic variceal ligation (banding).
- Refractory: Balloon tamponade (Sengstaken-Blakemore) or TIPS for persistent bleeding.
-
Peptic Ulcer Bleed (H. pylori/NSAIDs):
- Acute Rx: Endoscopic therapy (clips, thermal coagulation, epinephrine injection) combined with high-dose IV PPI.
- Test and treat for H. pylori after the acute bleed resolves.
⭐ In cirrhotic patients with variceal bleeding, prophylactic antibiotics (e.g., ceftriaxone) are crucial as they significantly reduce the risk of bacterial infections like SBP and improve overall survival.
Lower GI Bleed - Colon Carnage
-
Etiology: Common causes include diverticulosis, angiodysplasia, ischemic colitis, and malignancy.
- Diverticulosis: Most common cause of massive LGIB. Abrupt, painless, large-volume hematochezia. Usually stops spontaneously (>80%).
- Angiodysplasia: Dilated, tortuous submucosal vessels. Painless, recurrent, low-grade bleeding. Associated with CKD and aortic stenosis.
- Ischemic Colitis: "Watershed" areas (splenic flexure). Abdominal pain followed by bloody diarrhea, often post-hypotension.
-
Diagnosis & Management:
- Initial step: Hemodynamic resuscitation (ABCs, 2 large-bore IVs).
- Colonoscopy is the primary diagnostic and therapeutic tool.
- If bleeding is massive/obscures view: CTA or tagged RBC scan.
- Treatment: Endoscopic therapy (clipping, cautery), angiography with embolization, or surgery for refractory cases.
⭐ Heyde's Syndrome: A classic association between aortic stenosis and bleeding from angiodysplasia due to acquired von Willebrand factor deficiency.
High‑Yield Points - ⚡ Biggest Takeaways
- Initial management requires two large-bore IV lines for resuscitation before any diagnostic steps.
- For suspected variceal bleeding, immediately administer octreotide and prophylactic ceftriaxone.
- All patients with upper GI bleeding should receive IV proton pump inhibitors (PPIs).
- Endoscopy (EGD) is the cornerstone for both diagnosis and therapy in upper GI bleeds.
- Transfuse packed RBCs for hemoglobin <7 g/dL in most patients (<9 g/dL in cardiovascular disease).
- Colonoscopy is the procedure of choice for evaluating hemodynamically stable lower GI bleeds.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

