Pain Principles - The Analgesic Ladder
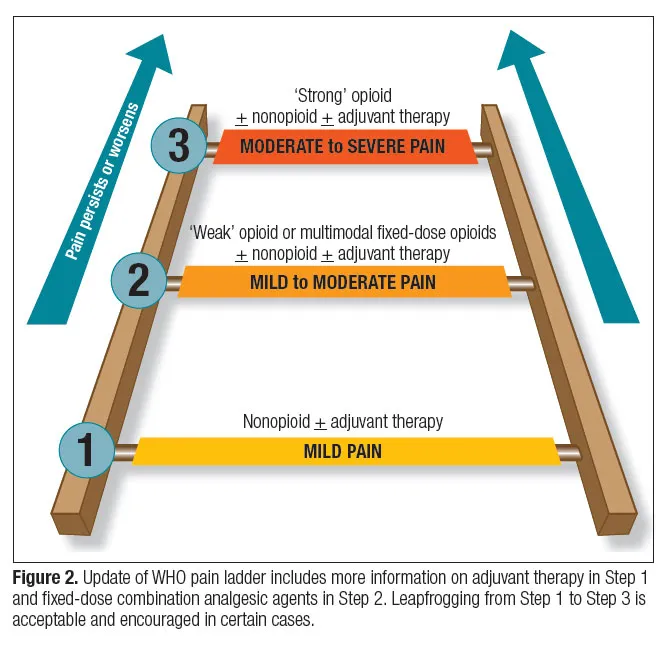
The WHO analgesic ladder provides a stepwise framework for managing pain, starting with the least potent drugs and escalating as needed. The goal is to stay ahead of the pain.
- Non-opioids: NSAIDs, Acetaminophen.
- Weak Opioids: Tramadol, Codeine.
- Strong Opioids: Morphine, Hydromorphone, Fentanyl.
- Adjuvants: Antidepressants (e.g., TCAs, SNRIs), Anticonvulsants (e.g., Gabapentin).
⭐ By the Clock Dosing: For persistent pain, analgesics should be given at regular intervals ("by the clock") rather than only when the patient requests them ("prn"). This maintains a therapeutic level and prevents breakthrough pain.
Non-Opioids - Foundation First
- Acetaminophen (APAP)
- Mechanism: Primarily central COX inhibition. First-line for mild-moderate pain.
- Dosing: Max daily dose 4g. Be aware of combination products (e.g., Percocet).
- Toxicity: Hepatotoxicity in overdose. Antidote: N-acetylcysteine (NAC).
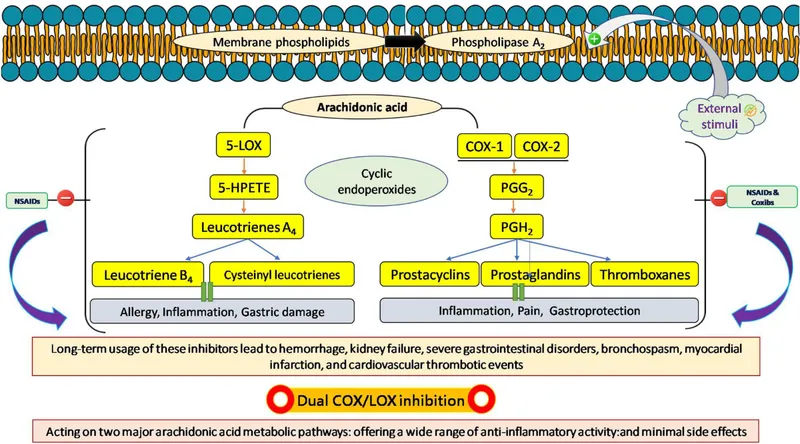
- NSAIDs
- Mechanism: Peripheral & central COX-1/2 inhibition, reducing prostaglandins.
- Types:
- Non-selective: Ibuprofen, Naproxen.
- Parenteral: Ketorolac (potent, for moderate-severe pain).
- COX-2 selective: Celecoxib (less GI risk, ↑ CV risk).
- ⚠️ Cautions: Renal insufficiency, peptic ulcer disease, cardiovascular disease, aspirin-exacerbated respiratory disease (AERD).
⭐ Ketorolac use is limited to a maximum of 5 days (cumulative duration for all routes) due to significant risk of GI bleeding and renal toxicity.
Opioids - The Heavy Hitters
- Mechanism: Full agonists at central μ-opioid receptors.
- Indications: Moderate to severe acute pain.
- Common Agents (IV):
- Morphine: The standard for comparison. Causes histamine release (itching, hypotension). Active metabolite (M6G) accumulates in renal failure.
- Hydromorphone (Dilaudid): 5-7x more potent than morphine. Less histamine release; better choice in hemodynamic instability or renal dysfunction.
- Fentanyl: 100x more potent than morphine. Fastest onset, shortest duration. Ideal for procedural pain and in renal/liver failure.
- Side Effects: Sedation, respiratory depression, constipation, nausea, miosis.
- Antidote: Naloxone.
⭐ Meperidine (Demerol) is generally avoided. Its metabolite, normeperidine, is neurotoxic, accumulates in renal failure, and lowers the seizure threshold.
Adjuncts & Blocks - Beyond the Pill
-
Systemic Adjuncts:
- Ketamine: Low-dose infusion for severe or opioid-tolerant pain (NMDA antagonist).
- IV Lidocaine: Systemic sodium channel blockade for visceral/neuropathic pain.
- Gabapentinoids: (Gabapentin/Pregabalin) Useful for neuropathic pain components.
- Corticosteroids: (Dexamethasone) Potent anti-inflammatory, reduces opioid needs.
-
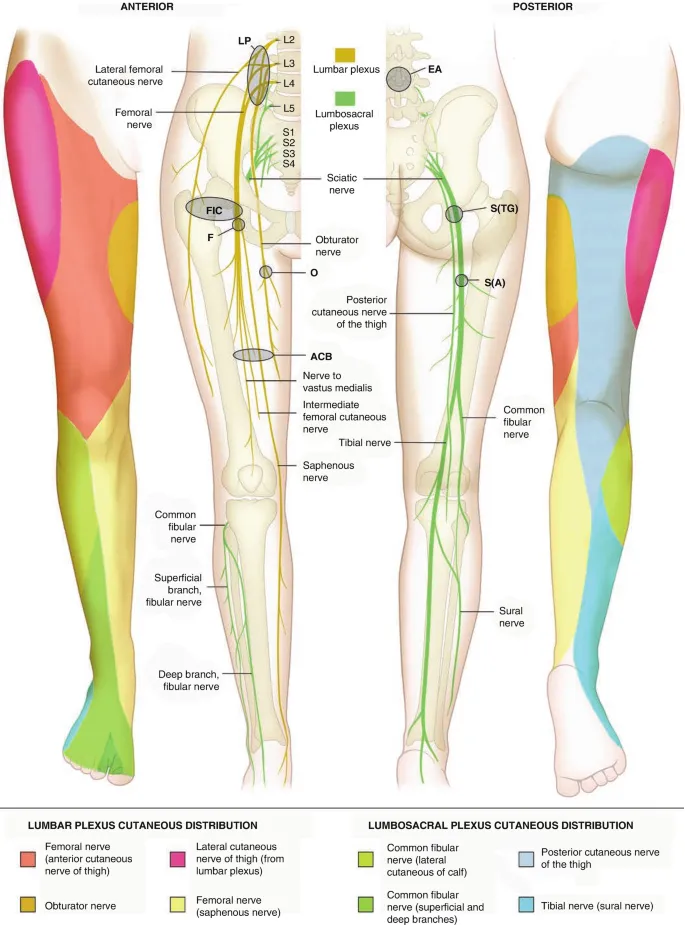
Regional Anesthesia & Nerve Blocks:
- Mechanism: Local anesthetic delivered near nerves to block nociception. Ultrasound guidance is standard of care.
- Benefits: Superior, site-specific analgesia; significant opioid-sparing effect, reduced side effects.
⭐ Local Anesthetic Systemic Toxicity (LAST): A rare but life-threatening complication of regional anesthesia. Presents with CNS (tinnitus, metallic taste, seizures) and cardiovascular (arrhythmias, collapse) symptoms. Treat immediately with 20% lipid emulsion therapy.
High-Yield Points - ⚡ Biggest Takeaways
- Pain is the fifth vital sign; always assess with a validated scale.
- Use multimodal analgesia (e.g., NSAIDs, acetaminophen, opioids) to maximize efficacy and minimize opioid side effects.
- NSAIDs and acetaminophen are first-line for mild-to-moderate pain; check contraindications like renal or liver disease.
- Reserve opioids for moderate-to-severe pain; monitor for respiratory depression, sedation, and constipation.
- Patient-Controlled Analgesia (PCA) offers excellent control for postoperative pain.
- Regional nerve blocks can significantly reduce systemic opioid needs for localized pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more