Pathophysiology - The Great Imitator
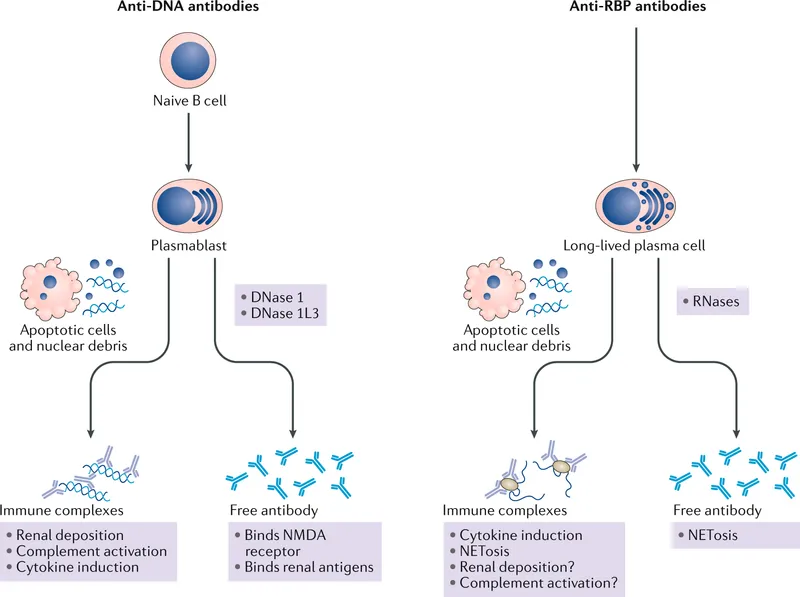
- Core Defect: Failure of self-tolerance, leading to autoantibody production against nuclear antigens (e.g., DNA, histones).
- Primary Mechanism: Type III hypersensitivity. Immune complexes (Ag-Ab) deposit in tissues (kidneys, skin, joints), activating complement (↓C3/C4) and causing inflammation.
- Also involves Type II hypersensitivity (cytotoxic antibodies against blood cells).
- Key Triggers: Genetic predisposition (HLA-DR2, HLA-DR3), UV light (induces keratinocyte apoptosis), infections, and drugs (hydralazine, procainamide).
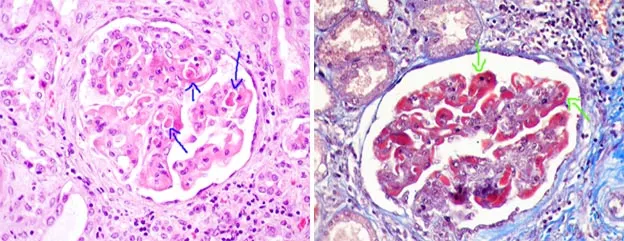
⭐ Anti-dsDNA antibodies are highly specific for SLE, and their titers often correlate with disease activity, especially lupus nephritis.
Clinical Presentation - Butterfly & Betrayal
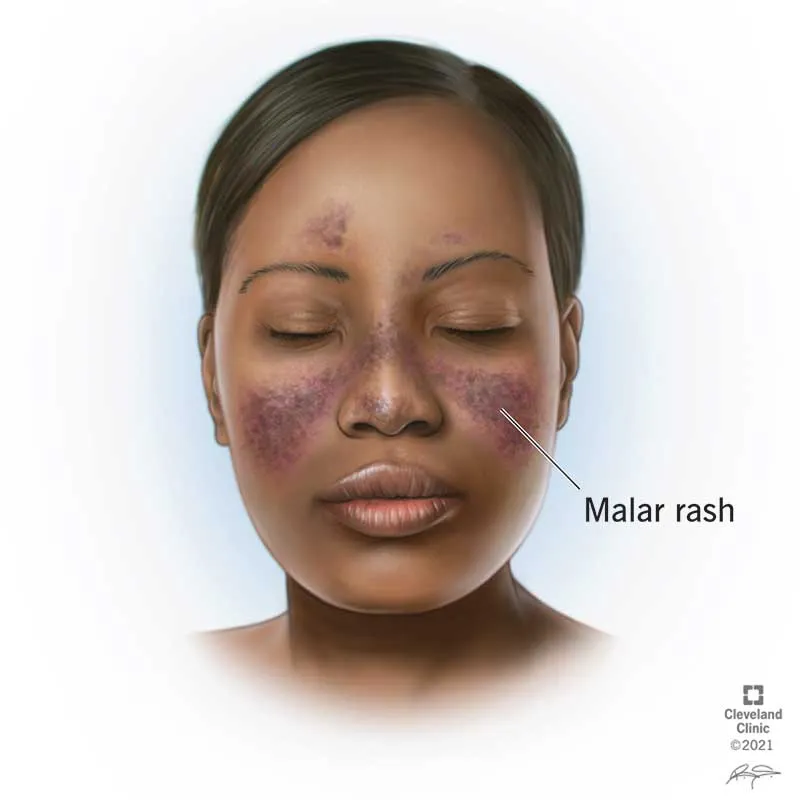
SLE is a quintessential multi-system autoimmune disease, presenting with a constellation of symptoms. The presentation is notoriously variable, ranging from indolent to fulminant.
📌 Mnemonic: SOAP BRAIN MD
- Serositis: Pleuritis or pericarditis.
- Oral ulcers: Typically painless.
- Arthritis: Non-erosive, involving ≥2 peripheral joints.
- Photosensitivity: Skin rash as an unusual reaction to sunlight.
- Blood disorders: Hemolytic anemia, leukopenia, lymphopenia, or thrombocytopenia.
- Renal disease: Proteinuria or cellular casts.
- ANA positive: The most sensitive test (>95%).
- Immunologic disorder: Anti-dsDNA, Anti-Sm, or antiphospholipid antibodies.
- Neurologic disorder: Seizures or psychosis.
- Malar rash: "Butterfly rash" over cheeks, sparing nasolabial folds.
- Discoid rash: Raised, scaly patches.
⭐ Drug-induced lupus (hydralazine, procainamide, isoniazid) is associated with anti-histone antibodies; renal and CNS involvement is rare.
Diagnosis & Labs - Cracking the Code
- Screening: Best initial test is Antinuclear Antibody (ANA); highly sensitive (>98%) but not specific. An ANA-negative result virtually excludes SLE.
- Confirmatory Antibodies:
- Anti-dsDNA: Highly specific, fluctuates with disease activity, strongly linked to lupus nephritis.
- Anti-Smith (Sm): The most specific antibody for SLE; part of diagnostic criteria.
- Other Key Labs:
- ↓ Low complement (C3, C4) indicates immune complex deposition and active disease.
- Pancytopenia (anemia of chronic disease, leukopenia, thrombocytopenia).
- Antiphospholipid antibodies (e.g., lupus anticoagulant, anti-cardiolipin).
⭐ High titers of anti-dsDNA antibodies and low complement levels are strong indicators of active lupus nephritis, a major cause of morbidity.
Management - Taming the Wolf
- Goal: Control flares, prevent organ damage, improve quality of life.
- Sun protection: Essential for all patients to prevent photosensitivity-induced flares.
- NSAIDs: For arthritis and serositis.
⭐ Hydroxychloroquine (HCQ) is foundational for ALL patients, regardless of severity. It reduces flares, organ damage, and mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- SLE is a chronic, multi-system autoimmune disease primarily affecting young women.
- Key autoantibodies include ANA (highly sensitive) and the more specific anti-dsDNA and anti-Sm.
- Drug-induced lupus is linked to anti-histone antibodies (e.g., hydralazine, procainamide).
- Classic features include malar rash, discoid rash, photosensitivity, and non-erosive arthritis.
- Lupus nephritis is a severe complication requiring renal biopsy for staging and management.
- Hydroxychloroquine is foundational therapy for all SLE patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

