Pathophysiology & Genetics - Salty Sweat & Sticky Stuff
- Genetics: Autosomal recessive mutation in the CFTR gene on chromosome 7.
- Most common mutation: ΔF508, a Class II mutation leading to misfolded protein.
- Pathophysiology: A defective CFTR protein creates a dysfunctional chloride channel, disrupting ion transport across epithelial cells.
- Mechanism & Effect:
- Sweat Ducts: Impaired NaCl reabsorption → high salt content in sweat (diagnostic).
- Airways/Pancreas: Decreased Cl⁻ secretion → thick, dehydrated mucus → obstruction, infection, and inflammation.
⭐ The "salty sweat" paradox: In sweat glands, CFTR reabsorbs chloride. In respiratory/GI epithelia, it secretes chloride. The channel's function is tissue-specific.
Clinical Manifestations - The Multi-System Mayhem
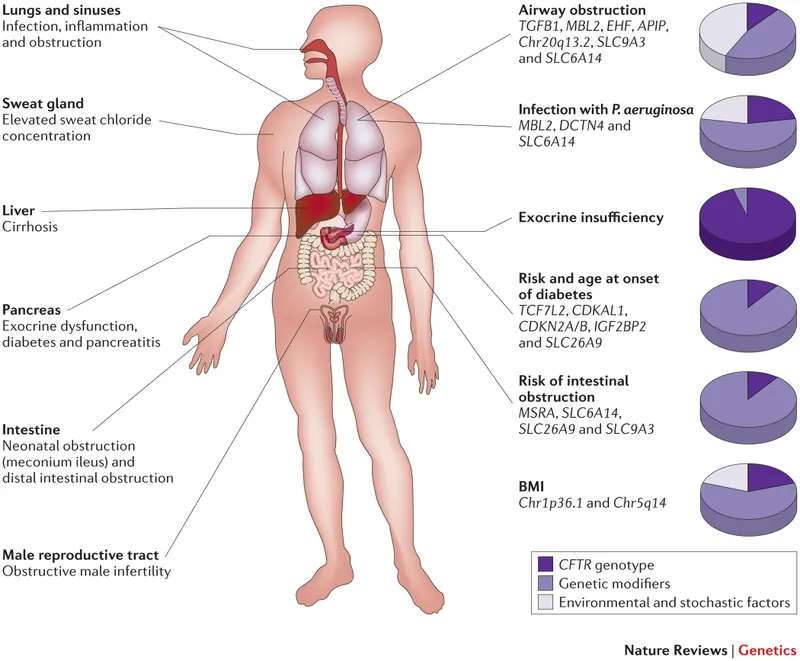
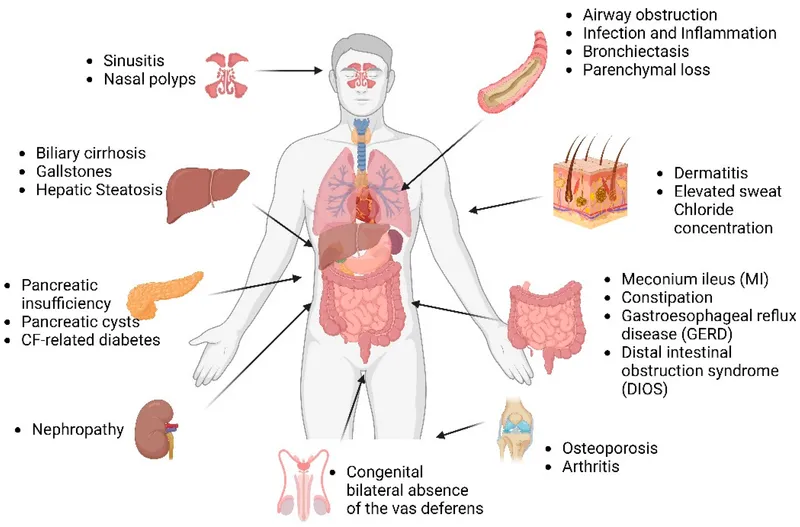
- Pulmonary: The dominant cause of morbidity/mortality.
- Persistent productive cough, wheezing, recurrent sinus/pulmonary infections (esp. Pseudomonas aeruginosa, S. aureus).
- Leads to bronchiectasis, hemoptysis, and eventual respiratory failure.
- Gastrointestinal:
- Exocrine pancreatic insufficiency (~85%): Steatorrhea, malabsorption of vitamins A, D, E, K.
- Distal Intestinal Obstruction Syndrome (DIOS).
- Hepatobiliary: Focal biliary cirrhosis, cholestasis, portal hypertension.
- Endocrine: CF-Related Diabetes (CFRD) due to progressive pancreatic islet destruction.
- Reproductive:
- Males: Infertility (>95%) from congenital bilateral absence of the vas deferens (CBAVD).
- Females: Reduced fertility (thick, tenacious cervical mucus).
- Other: Digital clubbing, hypertrophic osteoarthropathy, high sweat chloride.
⭐ Recurrent pulmonary exacerbations, often with mucoid Pseudomonas aeruginosa, are a hallmark of adult CF, strongly linked to accelerated decline in lung function.
Diagnosis - Catching the Chloride Culprit
- Primary Test: Quantitative pilocarpine iontophoresis (Sweat Chloride Test).
- Thresholds (mmol/L):
- < 30: CF unlikely.
- 30-59: Intermediate; requires further testing.
- ≥ 60: Diagnostic.
- Genetic Confirmation: CFTR gene analysis for inconclusive sweat tests or atypical presentations.
⭐ A diagnosis of CF generally requires clinical symptoms plus evidence of CFTR dysfunction (e.g., two positive sweat tests on different days, or identifying two CF-causing mutations).
Management & Treatment - The Modulator & Mop-Up Crew
- CFTR Modulators: Cornerstone therapy based on genotype.
- Potentiators (e.g., Ivacaftor): Increase channel opening for gating mutations (e.g., G551D).
- Correctors (e.g., Lumacaftor, Tezacaftor): Improve protein folding/trafficking for processing mutations (e.g., F508del).
- Combination (e.g., Elexacaftor/Tezacaftor/Ivacaftor - Trikafta): Highly effective for patients with at least one F508del mutation.
- Airway Clearance ("Mop-Up"):
- Dornase alfa (DNase) & hypertonic saline.
- Chest physiotherapy (vest, percussion).
- Chronic Therapies:
- Inhaled antibiotics for Pseudomonas (e.g., tobramycin, aztreonam).
⭐ Chronic azithromycin use is primarily for its anti-inflammatory and biofilm-disrupting effects, not its direct bactericidal action.
High‑Yield Points - ⚡ Biggest Takeaways
- Autosomal recessive CFTR gene mutation (ΔF508 is most common) causes defective chloride transport across epithelial cells.
- Suspect in adults with recurrent sinopulmonary infections (especially Pseudomonas), pancreatic insufficiency, and male infertility.
- Diagnosis is confirmed by an elevated sweat chloride test > 60 mEq/L.
- Pulmonary disease manifests as obstructive PFTs and bronchiectasis, the primary cause of mortality.
- Management includes airway clearance, pancreatic enzyme replacement, and antibiotics.
- CFTR modulators are a key emerging therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

