Asthma Diagnosis - The Wheezing Workup
- History & Physical: Look for classic triad: wheeze, cough (esp. nocturnal), dyspnea.
- Pulmonary Function Tests (PFTs) / Spirometry:
- ↓ FEV₁/FVC ratio (< 0.7)
- Reversibility post-bronchodilator: ↑ FEV₁ by ≥ 12% AND ≥ 200 mL.
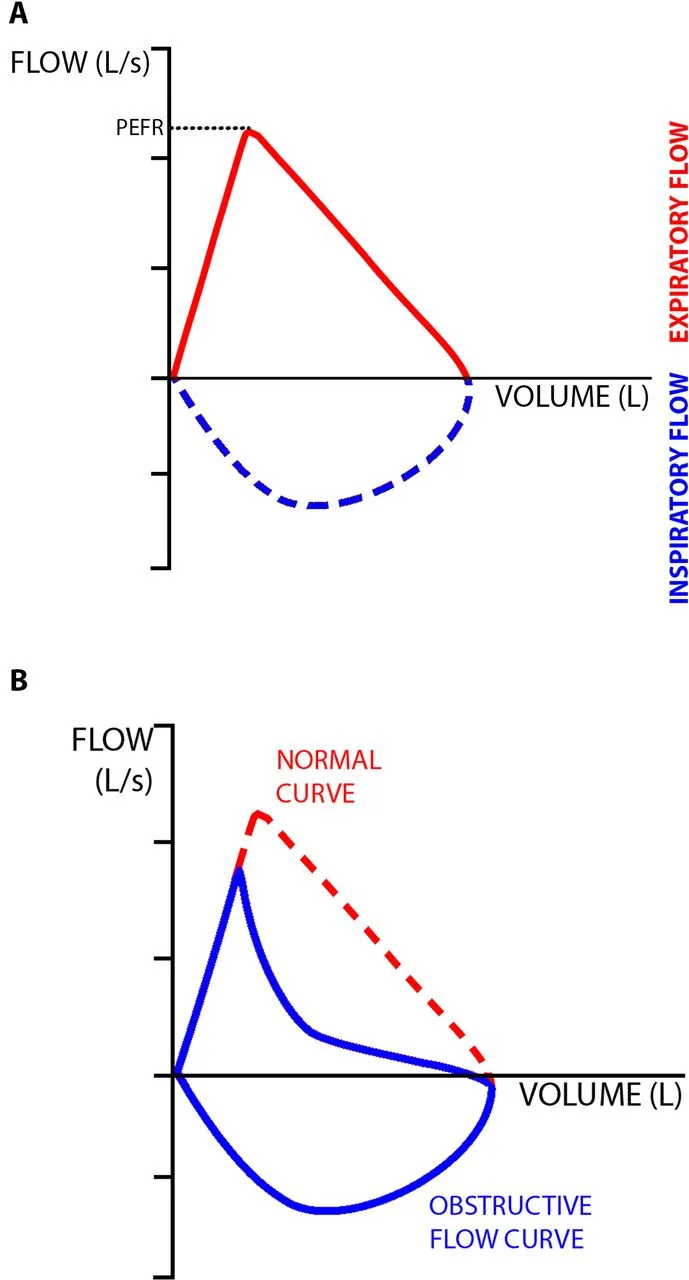
- Peak Expiratory Flow (PEF): Useful for home monitoring; diurnal variation > 20% is suggestive.
- Chest X-ray (CXR): Usually normal; rules out mimics.
⭐ Fractional Exhaled Nitric Oxide (FeNO): A high FeNO level (> 50 ppb) suggests eosinophilic airway inflammation, supporting an asthma diagnosis and predicting response to inhaled corticosteroids.
Stepwise Management - Climbing the Ladder
The goal is to use the minimum step required to maintain control. Treatment is escalated if symptoms persist and de-escalated if control is maintained for >3 months. The preferred approach (Track 1) uses ICS-formoterol as both controller and reliever.
- ICS: Inhaled Corticosteroid (e.g., Budesonide, Fluticasone)
- SABA: Short-Acting β2-Agonist (e.g., Albuterol)
- LABA: Long-Acting β2-Agonist (e.g., Formoterol, Salmeterol)
- LAMA: Long-Acting Muscarinic Antagonist (e.g., Tiotropium)
⭐ Exam Favorite: The biggest shift in recent GINA guidelines is the move away from SABA-only reliever therapy. As-needed low-dose ICS-formoterol is now the preferred reliever across all steps to reduce exacerbation risk.
Acute Exacerbation - Gasping for Air
- Triggers: Viral URI (most common), allergens, air pollution, exercise.
- Severity Assessment: Based on symptoms, PEF, and vitals.
- Mild-Moderate: PEF >40%, speaks in phrases.
- Severe: PEF <40%, speaks in words, accessory muscle use.
- Life-Threatening: Silent chest, confusion, cyanosis - impending respiratory failure.
⭐ A "normal" PaCO₂ in a tiring, tachypneic asthmatic is an ominous sign of impending hypercapnic respiratory failure. Prepare for intubation.
High‑Yield Points - ⚡ Biggest Takeaways
- Asthma diagnosis hinges on demonstrating reversible airway obstruction with spirometry (>12% and 200 mL increase in FEV1).
- Management is a stepwise approach: SABA PRN, then add a low-dose ICS, then a LABA.
- Viral URIs are the most common trigger for acute exacerbations.
- Treat exacerbations with systemic corticosteroids, high-dose SABA, and oxygen.
- Aspirin-exacerbated respiratory disease (AERD) presents with asthma, nasal polyps, and aspirin/NSAID sensitivity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

