Classification - The Fluid & Debris Spectrum
Based on the 2012 Revised Atlanta Classification, local complications are stratified by pancreatitis type and time. Interstitial edematous pancreatitis leads to fluid collections, while necrotizing pancreatitis results in collections containing necrotic debris. These collections mature and encapsulate after 4 weeks.
⭐ A key distinction: Pancreatic pseudocysts contain sterile fluid and lack a true epithelial lining. Walled-off necrosis (WON) is encapsulated and contains a mixture of liquid and solid necrotic material, with a higher risk of infection.
Fluid Collections - Just Fluid, Folks!
- Acute Peripancreatic Fluid Collection (APFC): Occurs <4 weeks post-pancreatitis. Homogenous fluid collection without a defined wall. Most resolve with expectant management.
- Pancreatic Pseudocyst: Develops >4 weeks later, forming a well-defined, encapsulated fibrous wall around the collection.
- Drainage Indications: Reserved for symptomatic patients (pain, obstruction), cysts >6 cm, or those that are enlarging.
⭐ A pseudocyst's wall is fibrous granulation tissue, NOT a true epithelial lining-a key distinction from cystic neoplasms.
Necrotic Collections - Walled-Off Trouble
- Develops from necrotizing pancreatitis. Initially an Acute Necrotic Collection (ANC) (<4 weeks), a heterogeneous mix of fluid and solid debris without a defined wall.
- Matures into Walled-Off Necrosis (WON) (≥4 weeks), an encapsulated collection with a thick, inflammatory wall.
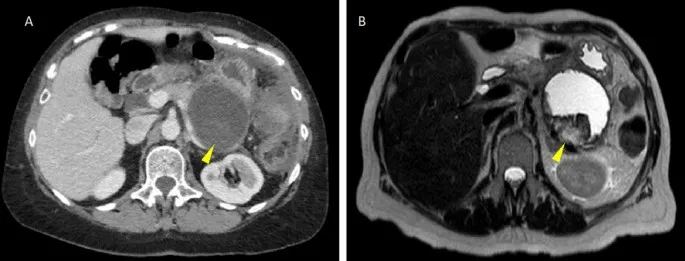
- Imaging (CECT): Shows non-enhancing pancreatic parenchyma with heterogeneous fluid/debris. Gas bubbles imply infection.
- Management:
- Sterile: Often managed supportively.
- Infected (suspected): Confirm with CT-guided Fine-Needle Aspiration (FNA). Treat with broad-spectrum antibiotics and drainage.
- Intervention: Endoscopic necrosectomy is preferred.
⭐ High-Yield: Delaying intervention for WON until at least 4 weeks allows the wall to mature, making endoscopic drainage safer and more effective.
Vascular Issues - Bleeding & Clotting Chaos
- Splenic Vein Thrombosis: Proximal inflammation can lead to thrombosis of the splenic vein, causing left-sided portal hypertension.
- Leads to isolated gastric varices (via short gastric veins) without esophageal varices.
- Pseudoaneurysm Formation: Enzymatic digestion weakens adjacent arteries (splenic, gastroduodenal, pancreaticoduodenal).
- Rupture can cause life-threatening hemorrhage into a pseudocyst, the GI tract, or peritoneum.
⭐ Splenic vein thrombosis is a classic cause of isolated gastric varices; suspect it in a patient with pancreatitis and upper GI bleeding.
- Management:
- Diagnosis: CT Angiography.
- Treatment: Angiographic embolization.
Organ Obstruction - Neighborhood Nuisances
- Gastric Outlet Obstruction: Duodenal inflammation or compression by a pseudocyst leads to early satiety and vomiting.
- Biliary Obstruction: Common bile duct compression from edema or a pseudocyst can cause jaundice.
- Colonic Inflammation: Most commonly affects the transverse colon and splenic flexure, risking ischemia.
- Pancreatic Ascites/Pleural Effusion: From a disrupted pancreatic duct leaking fluid.
⭐ A pleural effusion with markedly high amylase (>1000 IU/L) is pathognomonic for a pancreaticopleural fistula.
- Acute peripancreatic fluid collections (APFC) are the most common complication, seen <4 weeks after onset.
- Pancreatic pseudocysts are encapsulated fluid collections that mature at >4 weeks; they have high amylase content.
- Pancreatic necrosis is the most severe complication; infected necrosis carries the highest mortality risk.
- Walled-off necrosis (WON) is a mature, encapsulated area of necrosis, developing after >4 weeks.
- Contrast-enhanced CT (CECT) is the imaging modality of choice to differentiate fluid from necrosis.
- Vascular complications include splenic vein thrombosis and pseudoaneurysm formation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

