Initial Clues - The Grumbling Gland
-
Clinical Triad (often incomplete):
- Pain: Persistent, deep epigastric pain radiating to the back. Often postprandial, leading to food avoidance and weight loss.
- Malabsorption (Exocrine Insufficiency): Steatorrhea (bulky, foul-smelling, fatty stools), weight loss, and fat-soluble vitamin (A, D, E, K) deficiencies.
- Diabetes Mellitus (Endocrine Insufficiency): Late finding; often brittle and difficult to control.
-
Lab Findings:
- Serum amylase & lipase are typically normal or only mildly elevated, unlike in acute pancreatitis.
- ↓ Fecal elastase is a more sensitive indicator of exocrine dysfunction.
-
Etiology:
- 📌 TIGAR-O Mnemonic: Toxic-metabolic (alcohol, smoking), Idiopathic, Genetic, Autoimmune, Recurrent acute pancreatitis, Obstructive.
⭐ Amylase and lipase levels are often normal in chronic pancreatitis due to burnout of acinar cells, distinguishing it from acute pancreatitis where levels are significantly elevated.
Imaging Modalities - Pancreas Paparazzi
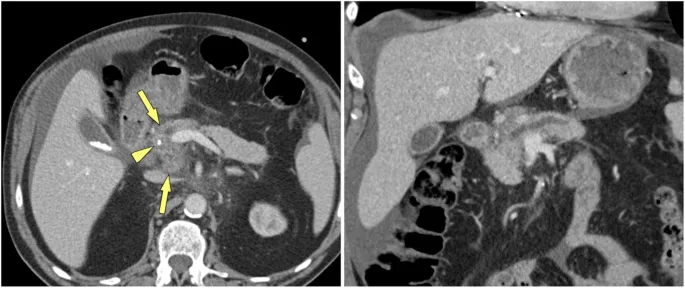
- CT Abdomen: Often the first-line imaging modality.
- Key findings: Pancreatic calcifications (pathognomonic), main pancreatic duct dilation (>3 mm), and parenchymal atrophy. Limited sensitivity for early disease.
- MRI / MRCP: Superior to CT for visualizing ductal anatomy, strictures, and pseudocysts without radiation.
- Secretin-stimulated MRCP (s-MRCP) dynamically assesses exocrine function by measuring duodenal filling.
- Endoscopic Ultrasound (EUS): Highly sensitive and specific for both early and late-stage disease.
- Detects subtle parenchymal (e.g., lobularity) and ductal changes.
- Guided by Rosemont criteria for diagnosis.
- ERCP: Historically the gold standard for visualizing ductal morphology (Cambridge classification).
- Invasive with significant risk of post-procedure pancreatitis; now reserved for therapeutic interventions.
⭐ Chain of Lakes: A classic, exam-favorite finding on MRCP or ERCP, representing alternating stenosis and dilation of the main pancreatic duct.
Function Tests - The Final Proof
-
Confirms exocrine insufficiency when imaging is inconclusive, especially in early disease.
-
Direct Test (Most Sensitive):
- Secretin Stimulation Test: Involves duodenal intubation to collect pancreatic fluid after IV secretin.
- Measures bicarbonate output; a concentration < 80 mEq/L is diagnostic.
- Highly sensitive and specific but invasive and rarely performed.
-
Indirect Tests (Non-Invasive):
- Fecal Elastase-1: Preferred initial test. Measures enzyme concentration in stool.
- Unaffected by pancreatic enzyme replacement therapy (PERT).
- Value < 200 µg/g suggests insufficiency.
- 72-hour Fecal Fat: Measures steatorrhea on a 100 g/day fat diet.
- Result > 7 g/day is abnormal.
- Fecal Elastase-1: Preferred initial test. Measures enzyme concentration in stool.
⭐ Fecal elastase is a practical, non-invasive first choice for suspected pancreatic exocrine insufficiency, though its sensitivity is lower in mild cases compared to the secretin test.
High‑Yield Points - ⚡ Biggest Takeaways
- Amylase/lipase are often normal, a key distinction from acute pancreatitis.
- The classic triad of pancreatic calcifications, steatorrhea, and diabetes mellitus indicates late-stage disease.
- CT abdomen is the best initial imaging to detect calcifications and ductal dilation.
- MRCP or EUS are the most sensitive imaging modalities for diagnosing early or mild chronic pancreatitis.
- The secretin stimulation test is the most specific test for pancreatic exocrine function, though rarely used.
- Fecal elastase is a reliable, non-invasive test for pancreatic exocrine insufficiency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

