Etiology & Triggers - The Usual Suspects
- Toxic-Metabolic (~70%):
- Alcohol abuse: The most common cause. Risk increases with duration and quantity.
- Smoking: Independent risk factor; potentiates alcohol damage.
- Chronic renal failure, hypercalcemia, hypertriglyceridemia.
- Idiopathic (~20%): No identifiable cause.
- Genetic: Mutations in PRSS1 (cationic trypsinogen), SPINK1, CFTR.
- Autoimmune: IgG4-related systemic disease.
- Recurrent and severe acute pancreatitis.
- Obstructive: Tumors, strictures, pancreas divisum.
⭐ Smoking is the single greatest risk factor that accelerates progression from alcoholic acute to chronic pancreatitis.
📌 Mnemonic: TIGAR-O
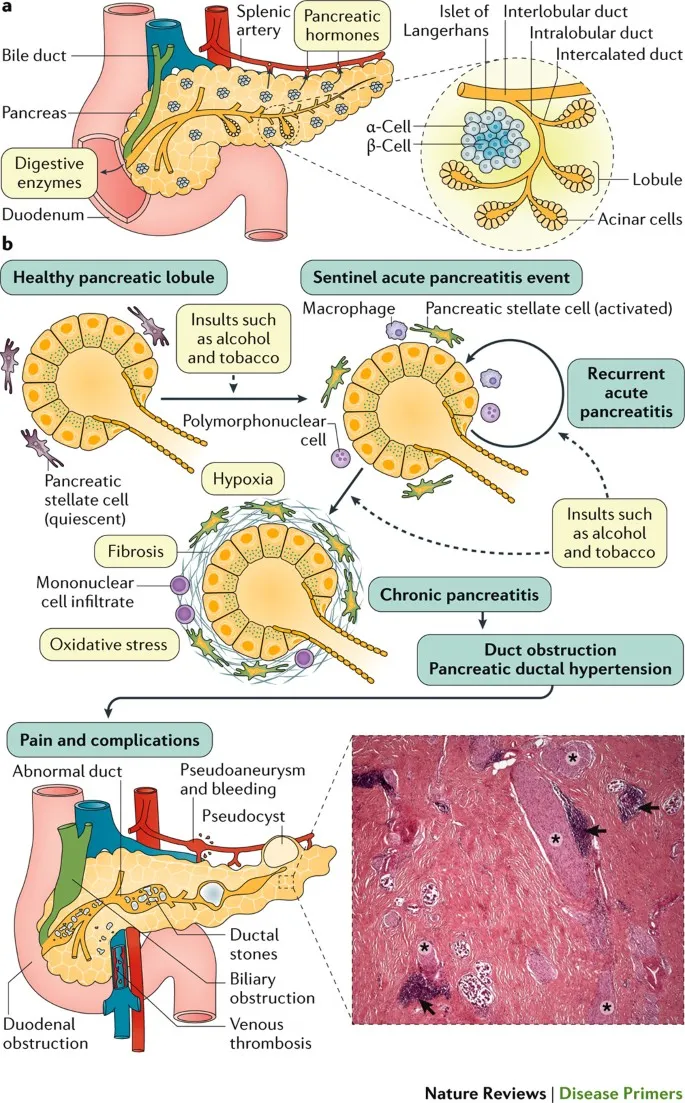
Pathophysiology Pathways - The Domino Effect

Multiple insults trigger a final common pathway: progressive, irreversible pancreatic fibrosis. The process is driven by the activation of pancreatic stellate cells.
- Core Mechanisms:
- Toxic-Metabolic: Direct acinar cell injury from toxins (e.g., alcohol) or metabolic stress.
- Ductal Obstruction: Blockage by protein plugs or stones leads to ↑ intraductal pressure, inflammation, and fibrosis.
- Necrosis-Fibrosis: Recurrent episodes of acute pancreatitis heal with scar tissue, gradually replacing healthy parenchyma (SAPE Hypothesis - Sentinel Acute Pancreatitis Event).
⭐ Pancreatic stellate cells (PSCs) are the key mediators of fibrosis, analogous to hepatic stellate cells in liver cirrhosis.
Fibrosis & Failure - The Scarring Cascade
-
Pancreatic Stellate Cell (PSC) Activation: The central event. Following injury (e.g., alcohol, oxidative stress), quiescent PSCs transform into myofibroblast-like cells, driven by cytokines like TGF-β and PDGF.
-
Irreversible Scarring: These activated PSCs deposit excess extracellular matrix (collagen, fibronectin), leading to dense parenchymal fibrosis, ductal distortion, and strictures.
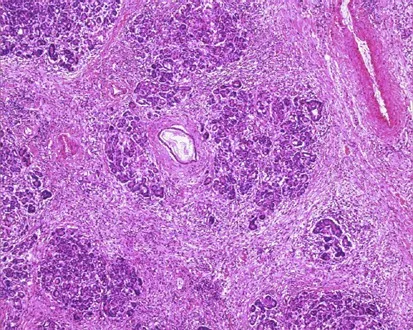
- Functional Loss: Progressive fibrosis destroys both acinar (exocrine) and islet (endocrine) cells, culminating in maldigestion and pancreatogenic diabetes (Type 3c).
⭐ On imaging (MRCP/ERCP), ductal strictures and upstream dilations create a classic "chain of lakes" appearance of the main pancreatic duct.
Clinical Consequences - System Shutdown
- Progressive Organ Failure: Fibrosis destroys both exocrine (acinar) and endocrine (islet) cells, leading to irreversible functional decline.
- Local Complications:
- Vascular: Splenic/portal vein thrombosis, pseudoaneurysms.
- Biliary: Obstructive jaundice from common bile duct stricture.
⭐ High-Yield: Chronic pancreatitis significantly increases the risk of pancreatic adenocarcinoma, with a cumulative risk of up to 4% over 20 years.
High‑Yield Points - ⚡ Biggest Takeaways
- Irreversible pancreatic damage from recurrent inflammation, leading to fibrosis and calcification.
- Chronic alcohol abuse is the most common etiology in adults.
- Pathogenesis involves ductal obstruction by protein plugs, leading to increased pressure and ischemia.
- Results in progressive loss of both exocrine (malabsorption, steatorrhea) and endocrine (diabetes mellitus) function.
- Key genetic predispositions include mutations in CFTR, SPINK1, and cationic trypsinogen (PRSS1).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

