Overview & Pathophysiology - Pancreas Under Fire
- A chronic fibro-inflammatory process driven by immune dysregulation, often mimicking pancreatic cancer.
- Two distinct subtypes:
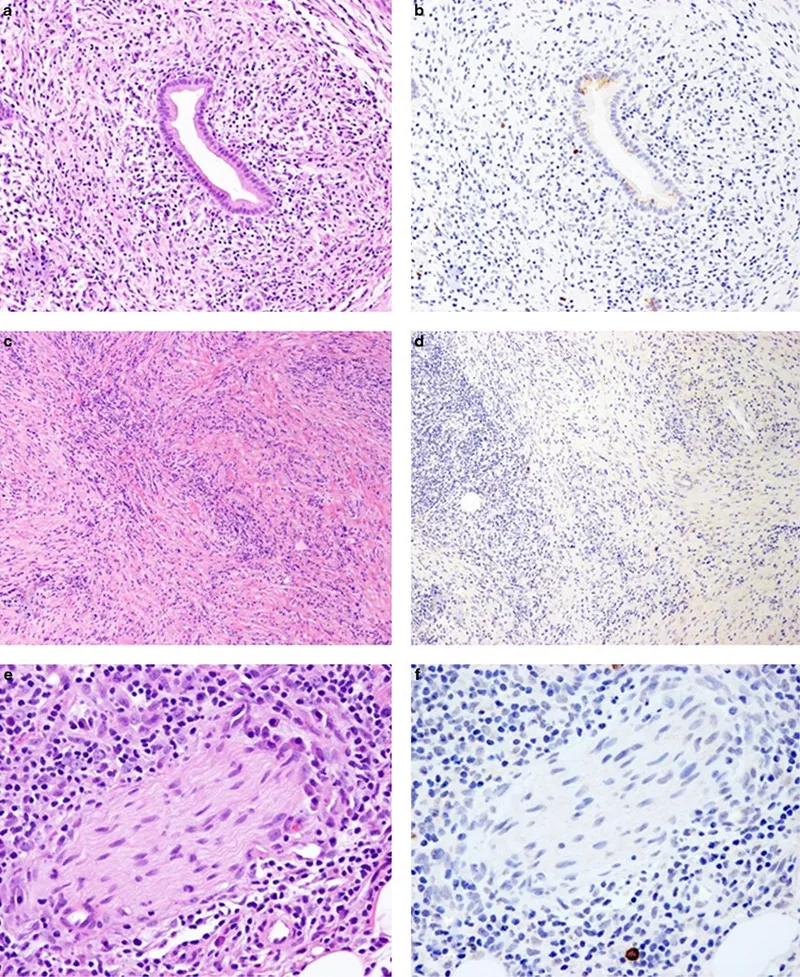
- Type 1 (Lymphoplasmacytic Sclerosing Pancreatitis): A manifestation of systemic IgG4-related disease (IgG4-RD). Typically affects males >60 years. Histology shows dense lymphoplasmacytic infiltrate, storiform fibrosis, and obliterative phlebitis.
- Type 2 (Idiopathic Duct-Centric Pancreatitis): A pancreas-specific disorder strongly associated with IBD (UC > Crohn's). Not related to IgG4. Histology shows neutrophilic infiltration of the ductal epithelium (granulocytic epithelial lesions or GELs).
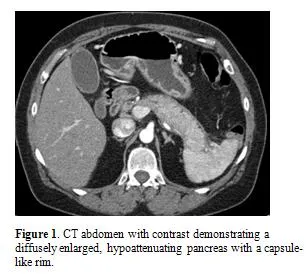
⭐ Type 1 AIP characteristically presents with a diffusely enlarged, featureless, "sausage-shaped" pancreas on imaging and is highly responsive to steroid therapy.
Clinical Presentation & Diagnosis - The Great Pretender
- Presents insidiously, often mimicking pancreatic cancer.
- Painless obstructive jaundice (most common presentation).
- Mild, recurrent abdominal pain or back pain; weight loss.
- Two distinct types:
- Type 1 (IgG4-related): Affects older males (>60), involves other organs (bile ducts, retroperitoneum, salivary glands), and shows ↑ serum IgG4.
- Type 2 (Idiopathic Duct-Centric): Affects younger patients, is strongly associated with IBD (especially Ulcerative Colitis), and has normal IgG4 levels.
- Key Investigations:
- Imaging: Diffusely enlarged, "sausage-shaped" pancreas with a featureless border and a surrounding capsule-like rim on CT/MRI.
- Serology: ↑ Serum IgG4 (>135 mg/dL) is highly suggestive of Type 1.
⭐ Often presents as painless obstructive jaundice, making it a key mimic of pancreatic adenocarcinoma. Biopsy is often required for differentiation.
- Diagnosis: Based on 📌 HISORt criteria (Histology, Imaging, Serology, Other organ involvement, Response to therapy).
Histology & Types - Two Faces of Inflammation
| Feature | Type 1 AIP (LGPS) | Type 2 AIP (IDCP) |
|---|---|---|
| Histology | Lymphoplasmacytic Sclerosing Pancreatitis (LGPS); dense periductal lymphoplasmacytic infiltrate, storiform fibrosis, obliterative phlebitis. | Idiopathic Duct-Centric Pancreatitis (IDCP); ductal neutrophilic infiltration (Granulocytic Epithelial Lesion - GEL), minimal fibrosis. |
| Serum IgG4 | ↑↑ Elevated in >80% | Normal |
| Systemic | IgG4-Related Disease (IgG4-RD); affects bile ducts, salivary glands, kidneys. | Pancreas-specific; rarely other organs. |
| Association | IgG4-RD | Inflammatory Bowel Disease (IBD), esp. Ulcerative Colitis (~30%). |
| Relapse | Common post-steroids | Rare |
Treatment & Management - Cooling the Flames
- Primary Goal: Induce remission, prevent relapse, and manage complications (e.g., biliary strictures).
⭐ Rituximab is increasingly used as a first-line agent for induction or for steroid-refractory/dependent disease, especially in Type 1 AIP, due to its high efficacy and steroid-sparing effects.
- Often mimics pancreatic cancer but features a "sausage-shaped" pancreas on imaging and elevated serum IgG4 levels (in Type 1).
- Type 1 is part of a systemic IgG4-related disease, affecting other organs like bile ducts and retroperitoneum.
- Type 2 is pancreas-specific and strongly associated with inflammatory bowel disease (IBD), particularly ulcerative colitis.
- Histology shows lymphoplasmacytic sclerosing pancreatitis (Type 1) or duct-centric inflammation (Type 2).
- Hallmark feature is a dramatic response to corticosteroids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

