Indications for RRT - The 'AEIOU' Vowels
📌 AEIOU
- Acidosis: Severe, refractory metabolic acidosis (e.g., pH < 7.1).
- Electrolytes: Symptomatic or severe, refractory hyperkalemia (e.g., K⁺ > 6.5 mEq/L with EKG changes).
- Intoxications: Acute poisoning with a dialyzable substance.
- 📌 SLIME: Salicylates, Lithium, Isopropanol, Methanol, Ethylene glycol.
- Overload: Refractory fluid overload (e.g., pulmonary edema unresponsive to diuretics).
- Uremia: Symptomatic manifestations.
- Uremic pericarditis.
- Uremic encephalopathy (asterixis, confusion, seizure).
⭐ Uremic pericarditis is an absolute indication for immediate dialysis, regardless of the BUN and creatinine values.

RRT Modalities - The Kidney's Helpers
- Hemodialysis (HD): Blood filtered externally via an artificial membrane (dialyzer). Requires vascular access.
- Access: AV Fistula (best), AV Graft, or Central Venous Catheter (highest infection risk).
- Schedule: Typically 3-4 hours, 3x/week in-center.
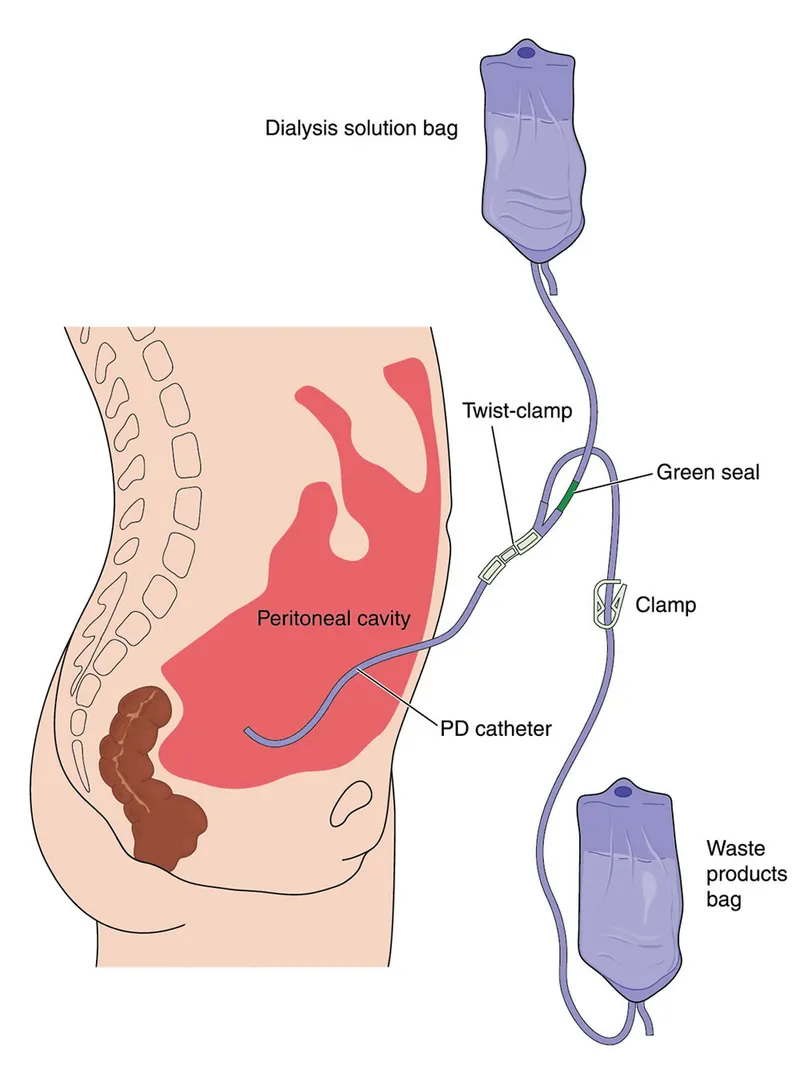
- Peritoneal Dialysis (PD): Uses the peritoneal membrane as the endogenous filter. Dialysate is instilled into the peritoneal cavity.
- Types: Continuous Ambulatory (CAPD) or Automated (APD).
- Major Risk: Peritonitis (cloudy effluent, abdominal pain).
- Continuous RRT (CRRT): Slow, continuous filtration for hemodynamically unstable ICU patients.
| Feature | Hemodialysis (HD) | Peritoneal Dialysis (PD) |
|---|---|---|
| Location | Center/Hospital | Home |
| Principle | Diffusion/Convection | Osmosis/Diffusion |
| Pros | High efficiency | Lifestyle flexibility |
| Cons | ↓ BP, access issues | Peritonitis, hyperglycemia |
Hemodialysis vs. Peritoneal - The Great Debate
| Feature | Hemodialysis (HD) | Peritoneal Dialysis (PD) |
|---|---|---|
| Location | Hospital or dialysis center | Home-based, daily |
| Access | AV fistula/graft or central venous catheter | Tenckhoff catheter (peritoneal) |
| Schedule | 3-4 hours, 3 times/week | Continuous (CAPD) or nightly (APD) |
| Mechanism | Solute diffusion across a semipermeable membrane in an external dialyzer. Rapid fluid/solute removal. | Peritoneal membrane is the endogenous dialyzer. Slower, more physiologic process. |
| Complications | Hypotension, muscle cramps, disequilibrium syndrome, access-related infection/thrombosis. | Peritonitis (cloudy fluid, abdominal pain), hyperglycemia, catheter site infection. |
Complications - When Good Filters Go Bad
-
Hemodialysis (HD)
- Hypotension: Most common acute complication from rapid ultrafiltration.
- Dialysis Disequilibrium Syndrome: Cerebral edema from rapid solute removal. Presents with headache, nausea, confusion, seizures.
- Access Issues: Infection (S. aureus), thrombosis, stenosis, aneurysm.
- Chronic: Dialysis-related amyloidosis (DRA) from ↑ β2-microglobulin deposition.
-
Peritoneal Dialysis (PD)
- Infection: Peritonitis (cloudy effluent, abdominal pain), exit-site/tunnel infections.
- Metabolic: Hyperglycemia (dextrose in dialysate), dyslipidemia.
- Mechanical: Hernias, dialysate leaks, catheter obstruction.
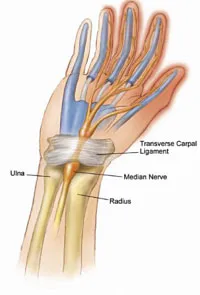
⭐ High-Yield: Dialysis-related amyloidosis (DRA) classically presents with carpal tunnel syndrome, scapulohumeral periarthritis, and bone cysts. It is a result of β2-microglobulin accumulation over years of dialysis.
High‑Yield Points - ⚡ Biggest Takeaways
- Urgent dialysis indications follow the AEIOU mnemonic: severe Acidosis, Electrolyte imbalance (K⁺ >6.5), Intoxication, fluid Overload, and Uremic symptoms (pericarditis, encephalopathy).
- AV fistula is the preferred hemodialysis access due to the lowest infection and thrombosis risk.
- Hypotension is the most common hemodialysis complication; peritonitis is the major risk with peritoneal dialysis.
- Dialysis disequilibrium syndrome results from rapid urea removal causing cerebral edema.
- CRRT is reserved for hemodynamically unstable patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

