Pathophysiology - Leaky Kidney Chaos
- Primary Insult: Damage to glomerular basement membrane (GBM) & podocyte foot processes.
- Core Defect: Loss of negative charge & size barrier → massive leakage of plasma proteins.
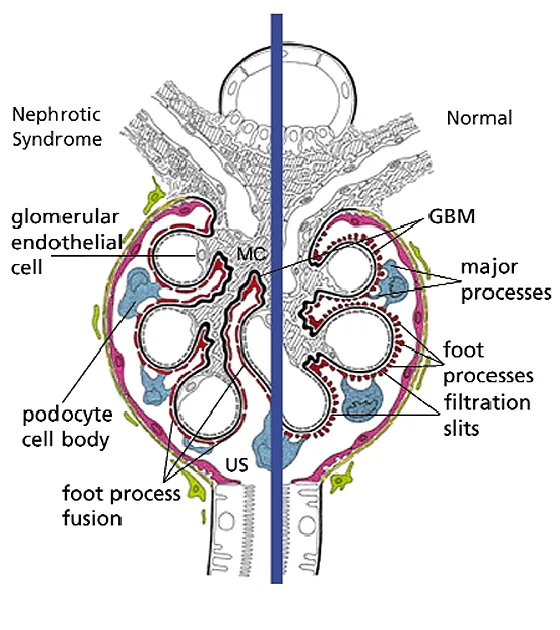
- Consequences:
- Edema: Periorbital, pitting, can lead to anasarca.
- Hyperlipidemia: ↑ liver production of lipids.
- Lipiduria: Oval fat bodies in urine (Maltese cross sign).
- Thrombosis Risk: ↑ loss of Antithrombin III in urine.
⭐ The hypercoagulable state, particularly renal vein thrombosis, is a classic and dangerous complication due to urinary loss of anticoagulant factors.
Etiology - The Usual Suspects
-
Primary Glomerular Disease (Idiopathic)
- Minimal Change Disease (MCD): Most common cause in children.
- Focal Segmental Glomerulosclerosis (FSGS): Most common cause in adults of African ancestry; associated with HIV, heroin use, obesity.
- Membranous Nephropathy: Most common cause in Caucasian adults.
- Membranoproliferative Glomerulonephritis (MPGN): Mixed nephrotic-nephritic picture.
-
Secondary Causes
- Systemic Disease: Diabetes Mellitus (most common secondary cause), SLE, Amyloidosis.
- Infection: Hepatitis B & C, HIV.
- Drugs: NSAIDs, penicillamine, gold salts.
- Malignancy: Lymphoma (MCD), solid tumors (Membranous).
⭐ In an older patient (>60 yrs) with new-onset nephrotic syndrome, suspect Membranous Nephropathy and screen for an underlying solid tumor (e.g., lung, colon).
Diagnosis - Puffy Patient Puzzle
- Urinalysis: Initial screen shows proteinuria. Key finding is heavy proteinuria: >3.5 g/24h or urine protein/creatinine ratio (UPCR) >3.5.
- Blood Tests:
- Hypoalbuminemia: Serum albumin <3 g/dL.
- Hyperlipidemia: ↑ LDL, ↑ cholesterol.
- Microscopy: Lipiduria with oval fat bodies.
⭐ Under polarized light, oval fat bodies containing cholesterol esters appear as classic “Maltese crosses.”
- Kidney Biopsy: Gold standard to identify the specific underlying glomerular disease (e.g., MCD, FSGS, MN).
Management & Complications - Damage Control Duty
-
General Management
- Diet: Salt restriction (<2 g/day), fluid restriction.
- Proteinuria: ACE inhibitors or ARBs.
-
Specific Therapy
- Edema: Loop diuretics (furosemide).
- Hyperlipidemia: HMG-CoA reductase inhibitors (statins).
- Thrombosis Prophylaxis: Consider anticoagulation if albumin is <2.5 g/dL or with other risk factors.
-
Key Complications
- Thromboembolism: Due to loss of antithrombin III. Most common is renal vein thrombosis.
- Infection: Loss of immunoglobulins (IgG) increases risk from encapsulated bacteria (e.g., S. pneumoniae).
⭐ In a patient with nephrotic syndrome, the sudden onset of flank pain, hematuria, and fever should raise high suspicion for renal vein thrombosis.
- Nephrotic syndrome is defined by massive proteinuria (>3.5 g/day), hypoalbuminemia, generalized edema, and hyperlipidemia/lipiduria.
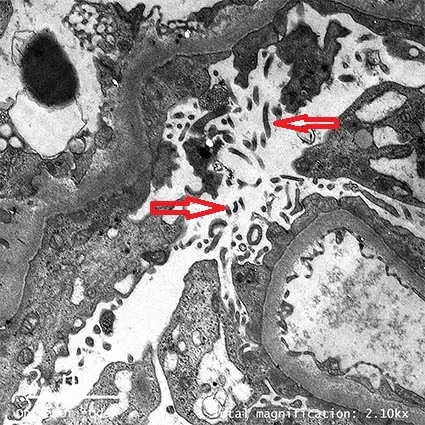
- The core pathology is podocyte injury, which compromises the glomerular filtration barrier, leading to protein loss.
- Minimal Change Disease is the most common cause in children and shows effacement of foot processes on EM.
- Membranous Nephropathy is the most common primary cause in white adults.
- FSGS is the most frequent cause in African American and Hispanic adults.
- Major complications include thromboembolism and increased susceptibility to infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

