Etiology & Risks - Seeds of Malignancy
- Cirrhosis: The single most dominant risk factor. Over 80% of HCC cases arise from pre-existing cirrhosis, regardless of the underlying cause.
- Chronic Viral Hepatitis:
- Hepatitis B (HBV): Directly oncogenic.
- Hepatitis C (HCV): Induces HCC primarily via cirrhosis.
- Metabolic & Toxic insults:
- Non-alcoholic fatty liver disease (NAFLD/NASH).
- Alcohol-related liver disease.
- Aflatoxin B1 exposure (Aspergillus mold).
- Genetic Disorders:
- Hereditary Hemochromatosis.
- Alpha-1 antitrypsin deficiency.
⭐ HBV can cause HCC without cirrhosis by integrating its DNA into host hepatocytes.
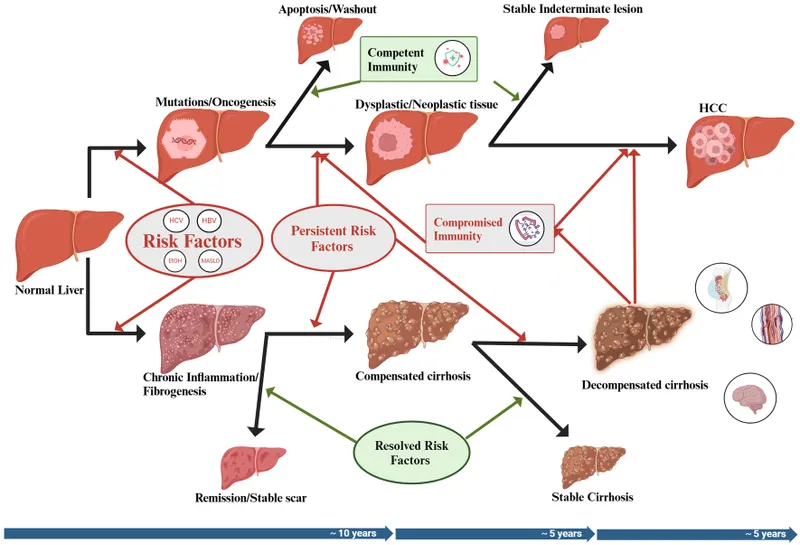
Clinical Presentation - The Silent Progression
- Often asymptomatic until advanced stages, growing silently within a cirrhotic liver.
- Sudden decompensation in a previously stable cirrhotic patient is a classic red flag.
- New or worsening ascites, jaundice, or hepatic encephalopathy.
- Nonspecific constitutional symptoms may appear late:
- RUQ pain or a palpable mass.
- Significant, unintentional weight loss.
- Early satiety.
- Paraneoplastic Syndromes can be the first sign:
- Erythrocytosis (↑EPO)
- Hypercalcemia (↑PTHrP)
- Hypoglycemia
- Watery diarrhea, hypokalemia (↑VIP)
⭐ Suspect HCC in any patient with cirrhosis who suddenly decompensates.
Diagnosis & Staging - The Malignancy Map
-
Screening (At-Risk: Cirrhosis):
- Ultrasound +/- AFP every 6 months.
-
Diagnosis:
- Imaging: Multiphasic CT/MRI is key.
- Arterial phase hyperenhancement.
- Venous/delayed phase washout.
- Tumor Markers:
- AFP >20 ng/mL is suggestive.
- AFP >400 ng/mL is highly specific.
- LI-RADS: Standardizes reporting on imaging.
- Imaging: Multiphasic CT/MRI is key.
⭐ In a cirrhotic patient, classic imaging findings (arterial hyperenhancement, venous washout) are diagnostic for HCC, making a biopsy often unnecessary.
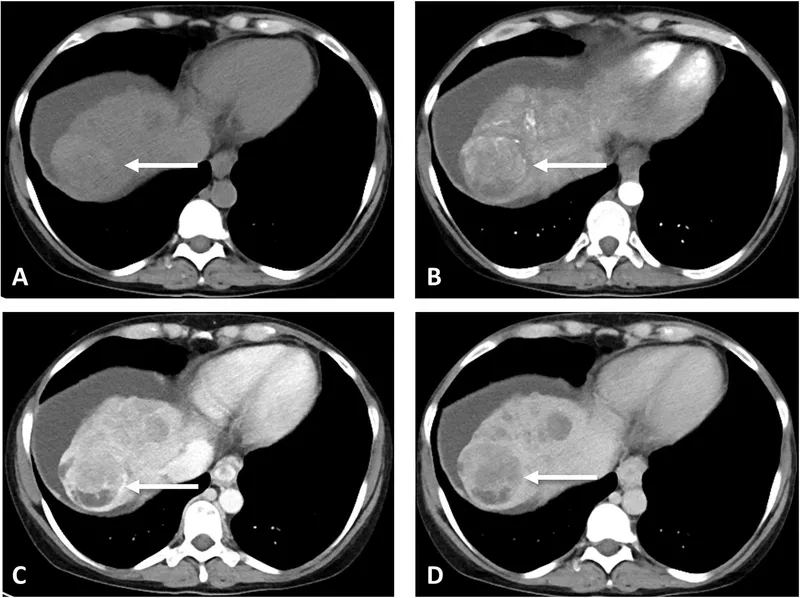
- Staging: Barcelona Clinic Liver Cancer (BCLC) system guides treatment.
Management - The Treatment Gauntlet
Treatment is stratified by the Barcelona Clinic Liver Cancer (BCLC) staging system, guiding the therapeutic approach from curative to palliative intent.
- Early Stage (Curative): Resection, liver transplant (within Milan criteria: 1 tumor <5 cm, or ≤3 tumors <3 cm), or ablation (RFA/MWA).
- Intermediate Stage:
⭐ Trans-arterial chemoembolization (TACE) is the standard for multifocal HCC without vascular invasion or metastasis. It is palliative, not curative, but can bridge patients to transplant.
- Advanced/Terminal Stage: Systemic therapy (e.g., Atezolizumab + Bevacizumab) for advanced disease; best supportive care for terminal illness.
High-Yield Points - ⚡ Biggest Takeaways
- Chronic hepatitis B/C and cirrhosis are the primary risk factors.
- Screen high-risk patients with ultrasound +/- AFP every 6 months.
- Alpha-fetoprotein (AFP) is the key tumor marker, but can be normal.
- Hallmark on imaging: arterial phase hyperenhancement and portal venous washout.
- Early-stage disease may be cured with resection or transplantation.
- Advanced HCC is treated with tyrosine kinase inhibitors like sorafenib.
- Associated with paraneoplastic syndromes like erythrocytosis and hypercalcemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

